Using newborns’ own umbilical cords as shunts for heart surgery

Cardiac surgery is reducing the use of plastic — starting with an operation for newborns who have life-threatening heart disease generally called single ventricle.
Single ventricle is so dangerous because it means only one of the heart’s two ventricles can adequately pump blood. Typically, affected infants undergo open-heart surgery to receive a Blalock shunt, which is a skinny tube made of PTFE — a synthetic polymer — that re-routes their blood flow to the lungs so enough oxygenated blood can get to their bodies. But when blood is exposed to foreign material, such as a plastic shunt, clots can form very easily.
This fall,a clinical trial at Boston Children’s Hospital will use patients’ own umbilical veins to create the shunt instead of plastic tubing.
Countering clotting
Clots in Blalock shunts pose a serious threat. “All of the blood flow to the lungs is dependent on that shunt staying open,” says Sitaram Emani, MD, who is leading the trial along with his colleague David Hoganson, MD.
If there is a clot, the blood oxygen level can drop so low that the infant needs emergency surgery to survive. “We now know clots occur more often than we thought — up to 20 percent of newborns have some form of clotting,” says Emani. “That’s why we’re so meticulous about using blood thinners.”
But blood thinners have a downside: increased bleeding.
“We’re essentially poisoning the whole system with anti-clotting agents,” Emani explains, “and preventing blood from clotting blood in places where it’s supposed to clot.”
A novel use for the umbilical vein
That’s where the umbilical vein comes in. The umbilical vein carries oxygenated blood from the placenta to a growing fetus via the umbilical cord. At birth, this vein closes when the cord is cut and the baby’s own circulatory system takes over.
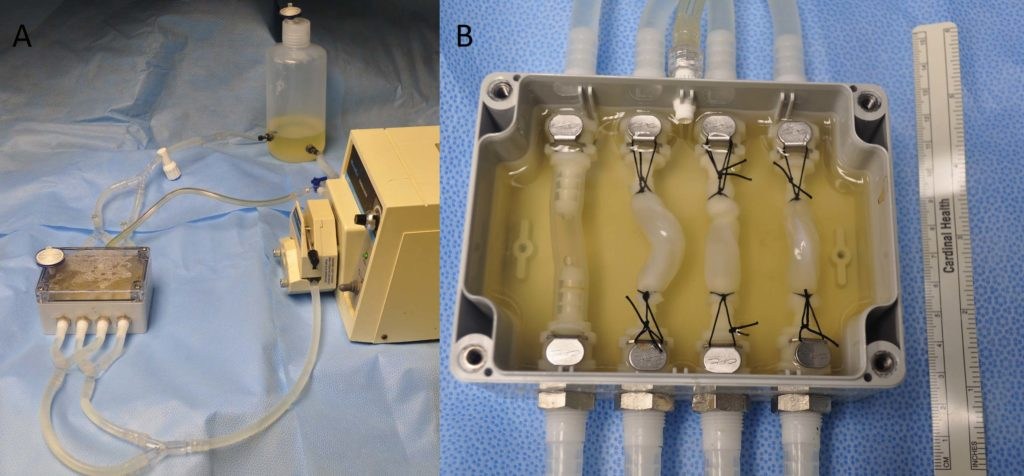
Like all blood vessels, the umbilical vein is lined with a protective layer called endothelium. “This helps blood flow smoothly through the vessel without clotting,” Emani explains. Umbilical veins can be set aside at birth and stored for later surgical use in a special device that provides nutrients.

“We have proven that not only can we get usable vein (with endothelium) from the cord at the time of delivery, but we can keep that tissue alive long enough to be used in single ventricle surgery, which is typically four to five days after birth,” says Emani. He and Hoganson presented these results at the American Association for Thoracic Surgery Annual Meeting this spring.
Emani and Hoganson also proved that the preserved veins were clot-resistant and were strong enough to withstand the mechanical pressure of blood circulation in the body.
Umbilical veins can be adjusted for size by placing an adjustable stent on their outside, which has no direct contact with blood. “We can then go back in when the child is a little bigger, and balloon-dilate the stent to expand the tissue,” explains Emani.
The hope is that preserved umbilical veins can be used in a variety of cardiac interventions. Emani predicts they may be useful to treat pulmonary atresia, aortic valve disease or any condition that requires reconstruction of valves or arteries in newborns.
“This is really just the beginning in terms of using placental and umbilical tissue for cardiac reconstruction,” he says.
The trial is now open and accepting patients.
Learn more about the Fetal Cardiology Program and Department of Cardiac Surgery.
If you are a physician with a complex-care patient to refer, call Boston Children’s priority line (1-844-BCH-PEDS).
Related Posts :
-

Beyond average-based medicine: HIE as a blueprint for data-informed care
Historically, outcome prediction in medicine has followed a familiar formula: run a clinical trial, publish the results, guide care based ...
-

Biventricular repair linked to better outcomes in superior-inferior ventricles treatment
The complexity of superior-inferior ventricles — a condition in which one ventricle is positioned on top of the other — has often ...
-

A reunion of the heart: Grace and Amy bond through HLHS
At first glance, Grace and Amy have a pretty typical friendship: they joke around, cheer each other on, and keep ...
-

First-of-its-kind pressurization test could improve Ross procedure outcomes
The Ross procedure is a preferred surgery to treat severe aortic valve disease. The procedure replaces the failing valve ...