A taste of childhood: One family’s journey to an IV-free diet
Children with short bowel syndrome often miss out on childhood’s simple and delicious pleasures, like birthday cake, pizza, and ice cream. But Dr. Lissette Jimenez and the team at the Center for Advanced Intestinal Rehabilitation (CAIR) at Boston Children’s Hospital are working to change that.
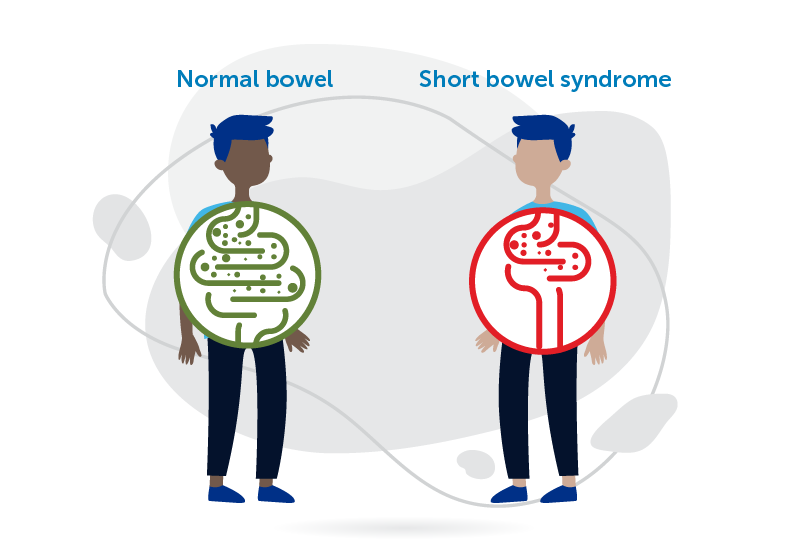
Short bowel syndrome is caused by the loss or lack of function of the small intestine, large intestine, or both, making it difficult for a child with the condition to absorb the proper nutrients needed to grow and thrive. As a result, those with short bowel syndrome rely on parenteral support, which is nutrition and fluids given intravenously (IV). Meena’s daughter is one of those children.
Meena’s daughter was diagnosed with short bowel syndrome 11 years ago while still in the womb. She is able to eat by mouth but has relied on supplemental parenteral nutrition (PN) her whole life. Recently, she started a new medical therapy, teduglutide (GATTEX), in an effort to wean off IV nutrition support.
Teduglutide is a medication that mimics GLP-2, a gastrointestinal hormone that stimulates and regulates the growth of intestinal tissue such as villi. Intestinal villi are finger-like structures that line the small intestine and allow the body to absorb nutrients. Teduglutide has been shown to increase the surface area of these villi, enhancing the ability to absorb fluids and nutrients.
A game-changing therapy
To learn more about the long-term outcomes of GATTEX, Dr. Jimenez is leading a multi-center registry among children with short bowel syndrome. The registry focuses on understanding whether and how patients like Meena’s daughter respond to the therapy and also examines its long-term safety.
“This study will allow us to understand how well GATTEX aids in a patient’s ability to wean off parenteral nutrition,” says Dr. Jimenez. “Our long-term goal is to improve children’s ability to absorb nutrients and wean off parenteral support.”
GATTEX was approved in 2019 for use in children 1 year of age and older, but Meena had been following developments around the medication long before that. She knew when the time was right that her daughter would be a good candidate.
“I knew this medicine would be a game-changer,” she says. Her daughter started GATTEX in 2020, and as Meena reports, “the results have been amazing.”
“Every patient is unique,” advises Dr. Jimenez. “What it means to be a success with GATTEX is different for every patient.”
For Meena’s daughter, success means about a 60 percent decrease in reliance on parenteral nutrition, less IV fluid support, and ultimately life with fewer limitations. For the first five years or so of her life, the family avoided travel due to her complicated feeding needs. But over time they have ventured to Disney World, Chicago, London, Amsterdam, and other places.
Meena is grateful for the difference GATTEX has made in her daughter’s ability to absorb nutrients and move away from parenteral nutrition. She advises parents of children on PN to encourage eating by mouth as much as possible.
“[For my daughter,] one Cheerio became a bowl of Cheerios,” she says. “Now she’s trying different food on her own; her favorites are cheese fondue and Mexican.”
Learn more about the Center for Advanced Intestinal Rehabilitation or make an appointment.
Teduglutide is FDA approved for pediatric patients 1 year of age and older.
Related Posts :
-

Leading the way: Ava’s experience with teduglutide
Ava Orsini visits Boston Children’s Hospital every two weeks. It’s more time than any kid wants to spend ...
-

Doing everything possible for Gabby: A team approach to short bowel syndrome
Gabriel “Gabby” Lopez loves everything hot and spicy. “He will eat a ghost pepper without hesitation,” says his mother, Mayra. “...
-

Growing up with short bowel syndrome: Follow-up care matters
Short bowel syndrome, a serious condition in which a child lacks sufficient small intestine to absorb the nutrients the body ...
-

Genetic causes of congenital diarrhea and enteropathy come into focus
Congenital diarrheas and enteropathies are rare and devastating for infants and children. Treatments have consisted mainly of fluid and nutritional ...





