The brightest rainbow follows the darkest storm: Our PVS journey

Caroline is our rainbow baby, born after the loss of another child, the light and color arising after a storm passes. A rainbow baby lifts a family in desperate need of lifting. It is a beautiful thing that I hope you never experience.
Caroline was born on Dec. 10, 2015. Just three months later, my wife Maleia and I found ourselves trailing an emergency medical helicopter flying our daughter to Iowa City. No words can fully describe the emotional pain we felt as we drove in stunned silence. Why is this happening again? We had already lost more than anyone should have to bear.
Two years earlier, our son Ben, almost 4 months old and already greatly beloved by his two older sisters as well as his parents, was just beginning to laugh and smile. Over several weeks, Ben had drifted lower on the growth charts, and our pediatrician suggested admitting him to the local children’s hospital to figure out once and for all the best formula to keep him healthy and growing. We thought.

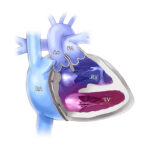
Ben rapidly declined in his first few days in the hospital. Increasingly intense testing revealed the truth: pulmonary vein stenosis (PVS). The same day the diagnosis was made, Ben died — March 21, 2014.
Pulmonary vein stenosis? In kids? I did not learn about this in medical school, residency, or fellowship. Maybe in adults, after atrial fibrillation treatment, but kids? Infants?
Grief for Ben hit me hard. I beat myself up wondering if earlier intervention would have helped more. What good was all my medical training? Should I have not known? Should I have not been able to do something? Grief would creep up when I least expected it. Simple everyday events became emotional minefields.
We learned to stop at the Build-A-Bear Workshop any time we came near a mall. Making a wish, kissing the heart, and giving the bear life — this child-sized routine came to help our daughters process their grief. Each stuffed creation brought them a little closer to the brother they lost.
We adults needed a different place to turn to with our grief, and we found it at The Compassionate Friends, a support network for people grieving the loss of a child. I took strange comfort from seeing another parent tear up as she explained that she still grieved the loss of her child more than 20 years later. That assured me the hole in my heart would never completely heal — I did not want it to — and that I was not alone.

In the eye of the hurricane
This is where our family was when Caroline was born, and she brought our family joy we desperately needed. We thought the absolute worst of the storm was passing. However, really, we were in the eye of the hurricane. A fierce storm still raged just behind our backs.
The first time Caroline threw up formula, dad-me thought, “Oh no! That’s what Ben did.”
Logical, evidence-based doctor-me thought, “PVS is a one-in-one-million diagnosis. It’s not an inherited disease. All kids spit-up formula, Doug.”
As time passed, Caroline drifted down the growth curve. Our pediatrician urged us to do an echocardiogram and a chest x-ray. As a radiologist, I will never forget seeing Caroline’s chest x-ray. Normal sized heart — and the ugliest pulmonary edema pattern imaginable. In 18 years and tens of thousands of chest x-rays, I had only seen this pattern once.
Ben.
I did not need the echo (echocardiogram), CTA (computed tomography angiography), or cardiac catheterization to tell me. I knew.
PVS.
Shock, sadness, fear… words fail. Grief roared back, a category five hurricane. I did not feel anything. I cried, but the hollowness inside me was the worst. Even four years later, it is hard to describe the brutality of that emotional emptiness.
There was no time right then, with the x-ray and testing, to process much about the experience we were suddenly thrown into. There was too much to do. Decisions had to be made now that it was clear my daughter, my family, and even my community, would have to fight this dragon.
How bad was Caroline’s PVS? Could it be something else? Do we even have a week? Should we transfer her to Des Moines or Iowa City? How could we even begin to explain to our older girls, amid their existing grief?
Anxiety, sadness, and fear dominated our thoughts while we decided on the University of Iowa and followed our tiny rainbow to a larger hospital in search of any ray of hope. Hope was in short supply, though. University of Iowa pediatric cardiologists confirmed PVS and offered two choices: Simply love on Caroline for another month. Two at the most. Or, take a chance and transfer her to one of only a handful of hospitals in the world that attempt to treat PVS in children, Boston Children’s Hospital.
We chose choice two AND loved on her as hard as we could. Every. Single. Month.

A lessening surge
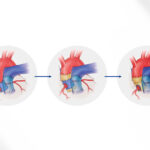
That is where Caroline’s story diverges from Ben’s. Caroline, too, needed massive support in the cardiac ICU (intensive care unit). She came in on a Sunday morning and was an emergency add-on case by Monday morning. They found severe disease in three veins, with some atretic veins. One vein somehow kept Caroline alive. Balloons opened her veins and were a rickety, unstable bridge that got Caroline to cardiac surgery a week later. Many medicines — imatinib, bevacizumab, sildenafil, sirolimus, losartan, Lasix — became part of Caroline’s life.
We celebrated Caroline’s 4-month birthday. Then her 5-month, and her 6-month. We did not know how many of these we would get — we were not at all sure she would reach her first birthday. However, we did.
For two very difficult years, our family lived split between two cities, to keep Caroline within a mile of Boston Children’s. It worked. Our storm surges gradually lessened and PVS passed.

Caroline is “almost 5” years old — her words. She swings like a monkey from a gymnastic beam in our home, builds Lego creations, chases her sisters, and started remote preschool last fall. Best of all, we are finally back together as a family, living under one roof.
I thank Caroline’s pediatric cardiologist and chief dragon-slayer, Dr. Kathy Jenkins, as well as Drs. Ryan Callahan, Chris Baird, John Kheir, Jim Lock, and nurse practitioner Christina Ireland for pushing back against this previously lethal disease for children and families around the world. Your dedication and continual push for progress has produced the advances that have saved my daughter’s life. Saved my family. Saved me.
Dr. Doug Lake is a radiologist in Ames, Iowa, father of three girls, and author of “Esophagus Attack! – The 3-Step Method to Enjoy Eating Again.” His full story was originally published in Children, an international, peer-reviewed, open access journal of pediatrics published monthly online, and edited for Answers.
Related Posts :
-

Biventricular repair linked to better outcomes in superior-inferior ventricles treatment
The complexity of superior-inferior ventricles — a condition in which one ventricle is positioned on top of the other — has often ...
-

A reunion of the heart: Grace and Amy bond through HLHS
At first glance, Grace and Amy have a pretty typical friendship: they joke around, cheer each other on, and keep ...
-

First-of-its-kind pressurization test could improve Ross procedure outcomes
The Ross procedure is a preferred surgery to treat severe aortic valve disease. The procedure replaces the failing valve ...
-

The ‘Trach Chapter’: Isabella’s journey with bronchopulmonary dysplasia
Isabella’s life has been anything but ordinary. Born at just 27 weeks gestation and weighing only 1 pound, 4 ounces, Isabella has ...