Mermaid Caitlyn and her mer-doctor face interstitial lung disease

Our daughter Caitlyn’s first year-and-a-half of life was a puzzle. She was getting sicker and sicker and no one near our home in New York could figure her out. After a period of unexplained rashes and weight loss, our pediatrician’s office said to us, “Something’s wrong and we don’t know what it is. Put her in the car and drive her to Boston Children’s Hospital.”
I love my kids more than anything in the world, and there’s not a single thing I wouldn’t do for them — including driving to Boston for Caitlyn’s care. So that’s just what we did.
When we arrived, we met with rheumatologist Dr. Fatma Dedeoglu and dermatologist Dr. Ruth Ann Vleugels. From that first day, everyone has been amazing. Dr. Dedeoglu told us, “Even if we don’t have a clear cut answer today, we won’t give up looking for answers and I promise you, you will leave here with a management plan.”
We finally had a team that could help.
Interstitial lung disease
Caitlyn has since spent a good amount of time inpatient at Boston Children’s. She knows everyone and loves coming to see them, but it’s still really hard for her to be sick and stuck in the hospital, away from home and her five older siblings.
Then last year, when Caitlyn was 4, she was getting admitted a lot for croup and hypoxia, or low oxygen. That’s when pulmonologist Dr. Alicia Casey got involved. She suspected interstitial lung disease (ILD), which was confirmed through testing soon after.

Caitlyn is now on oxygen 24 hours a day and we still come to Boston more than we’d like. It’s been a really, really rough ride, but despite all the hospital admissions, Caitlyn manages to push through and keep fighting. And so does her team. Even when I call them 4,000 times with problems, they’ve never once turned away from us or given up on Caitlyn.
Whenever we’re inpatient, Caitlyn’s pulmonology team stops in to check in on her, whether they’re on service or not. One day, while Caitlyn was in intensive care, Dr. Casey came by for a visit. Through her pain, Caitlyn shared the details of a dream she had where she and Dr. Ryan Perkins were mermaids, swimming in Hawaii. In the dream, Dr. Perkins was a blue mermaid and Caitlyn was pink.
A dedicated pulmonology team makes a mermaid’s dream come true
A few days later, Dr. Casey showed up in Caitlyn’s room with a surprise gift — a pink mermaid costume. Caitlin was all smiles! But there was more, Dr. Casey said. We started to hear music from “The Little Mermaid” playing in the hallway, and a lot of laughter from the nurses station. At that point, I knew Dr. Casey had something up her sleeve but I could have never guessed what.
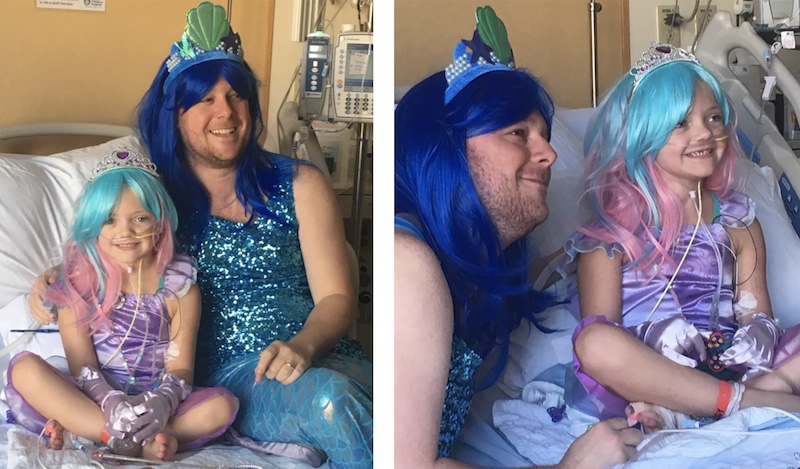
In comes Dr. Perkins dressed up as a blue mermaid, trailed by Caitlyn’s primary pulmonology team, including Dr. Casey, nurse Virginia Dimakis and child life specialist Jennifer Nguyen. Watching my daughter’s eyes light up was indescribable. I have not seen her light up that way in a long time. Even though she had a chest tube and was really struggling, her smile, her eyes … everything was just shining. That moment was literally a dream come true for her.
The importance of quality of life
Caitlyn still talks about the day Dr. Perkins dressed up as a blue mermaid. She told her beloved pediatrician, Dr. William Fredette, all about it. She keeps the photos in her bedroom at home, and has laminated copies she brings with her to Boston every time she’s admitted. And of course she wears the mermaid costume all the time. It’s a fight to get it off her!
Aside from being over-the-top brilliant, skilled, and caring, Caitlyn’s care team realizes that quality of life is a huge thing. That is so important. My daughter may be sick and in the hospital a lot, but she is still a normal 5-year-old kid. They went way above and beyond that day to make my little girl smile. It wasn’t something they had to do, by any means, but they did it. And it meant the world to us.
Learn more about our Interstitial Lung Disease Program.
Related Posts :
-

Four things you should know about MAPCAs treatment
As the first grandchild in her family, Hannah Homan is in demand for frequent visits. She was also the focus ...
-

A case for Kennedy — and for rapid genomic testing in every NICU
Kennedy was born in August 2025 after what her parents, John and Diana, describe as an uneventful pregnancy. Soon after delivery, ...
-

Treating MAPCAs with unifocalization surgery and cardiology care
Children born with a rare form of tetralogy of Fallot (ToF) face a challenging type of congenital heart ...
-

The journey to a treatment for hereditary spastic paraplegia
In 2016, Darius Ebrahimi-Fakhari, MD, PhD, then a neurology fellow at Boston Children’s Hospital, met two little girls with spasticity ...





