After four unsuccessful heart surgeries, Nicholas finds hope

When Brenna and Lorenzo Degano arrived in Boston with their son, Nicholas, last April, it was with a feeling of restrained hope. After four unsuccessful heart surgeries in California, they were hesitant to put their son through a fifth surgery not knowing if the outcome would be any different.
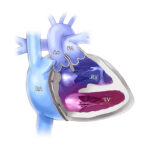
Nicholas was diagnosed at age 7 months with congenitally corrected transposition of the great arteries (CCTGA), an extremely rare congenital heart defect. In CCTGA, the heart’s two lower chambers (ventricles) and the valves and arteries that are attached to them are reversed. This can lead to problems with heart rhythm, heart valves and heart failure.
“When we learned Nicholas had CCTGA our world came crashing down,” says Brenna. “While he didn’t need immediate treatment, that felt like both a blessing and a curse: We were happy he didn’t need to be whisked away for surgery right away, but were faced with making hard decisions about his treatment options.”
Tough treatment decisions
The team at their local children’s hospital suggested they wait until Nicholas was having symptoms before treating his condition. Brenna did some research online and decided to move his care to another children’s hospital in California. That team suggested the best course of treatment was to perform several pulmonary artery banding operations to prepare Nicholas’ heart for a double-switch procedure. They hoped the double-switch would “correct” his blood flow and prevent heart failure in the future.

The Deganos decided to move forward with this approach and Nicholas’ first surgery was scheduled for December 2010. That was followed by two more surgeries in 2011 and 2012.
“He had three surgeries within 20 months, and nothing was changing his ventricle, it wasn’t getting stronger,” says Brenna. “The team suggested a fourth pulmonary artery banding procedure, but after the third unsuccessful surgery, we were drained. We told them we just couldn’t do it.”
At that point, Nicholas was doing OK, so they decided to wait and give his heart more time to improve. A year later, they went back for a check-up, and nothing had changed. The team suggested waiting a few more years. Finally, in 2017 the doctors told the Deganos that Nicholas’ heart would never be ready for the double-switch unless he had a fourth pulmonary artery banding.
“It felt like the pressure was on. They said it was important to do the double-switch before puberty or he could go into heart failure,” says Brenna. Nicholas was 10.
Reaching a tipping point
Still, they were frightened and hesitant to put Nicholas through another procedure. Ultimately, a fundraising event at Nicholas’ new school provided the tipping point.
“They were running laps around the track to raise money,” says Brenna. “Nicholas was really struggling because of his heart and couldn’t keep up with his friends.”
After the event, Nicholas told Brenna he wished he had the double-switch so he could run as fast as his friends. “That was a definitive moment for me and we decided to move ahead with the procedure.”
Nicholas had a fourth pulmonary artery banding in March of 2017. “Almost right away we could tell something wasn’t right,” says Brenna. “I could see that he was really struggling. He had no stamina or endurance. He would just come home from school and sleep, and his lips and fingernails looked purple all the time.”

Eight months later, they learned his left ventricle was in heart failure because the band was too tight. “His surgeon said he thought it was OK to leave Nicholas in state of heart failure for six to nine months to see if his heart would improve. I felt defeated and thought maybe there was another path.”
A second opinion in Boston brings hope
That’s when they decided to reach out to cardiologist Dr. Gerald Marx at Boston Children’s Hospital. They had contacted him a few years earlier, but decided to remain in California for Nicholas’ care. “Dr. Marx set up a phone consult with us right away,” says Brenna. “He told us that he would not recommend leaving Nicholas in heart failure. We agreed.”
They made plans to travel to Boston to meet with Dr. Marx and Dr. Pedro del Nido, chief of Cardiac Surgery. “Dr. del Nido thought we had a small window of opportunity in which to perform the double-switch. It was his opinion that if we waited too much longer, his heart would be in bad shape, and surgery would not be possible.”
After running a whole gamut of tests to make sure Nicholas’ heart could withstand the procedure, Dr. del Nido and his team performed a double-switch operation on Nicholas on April 3, 2018.
Finally, a sense of relief
“Before he was even awake we could already see a difference,” says Brenna. “His lips and fingernails were pink instead of purple. It was obvious to us that this surgery was what was needed. We felt relief for the first time.”

Nicholas recovered quickly and was out of the hospital in seven days. He and his family returned home to California a few weeks later. “For the first time in his life, he could run the mile in school,” says Brenna. “And recently he was able to beat his goal of running it in under 10 minutes, by running it in 8 minutes, 43 seconds.” He’s also back to playing baseball, a sport he had to give up for two years.
In the year since Nicholas’ surgery, Brenna has also noticed lots of other changes. “He just looks different. He’s blossoming into what he was always meant to be,” she says. “We don’t think that would have been possible if we hadn’t gone to Boston. It wasn’t just a lifesaver for Nicholas, but for our whole family.”
Learn more about the Department of Cardiac Surgery.
Related Posts :
-

Biventricular repair linked to better outcomes in superior-inferior ventricles treatment
The complexity of superior-inferior ventricles — a condition in which one ventricle is positioned on top of the other — has often ...
-

A reunion of the heart: Grace and Amy bond through HLHS
At first glance, Grace and Amy have a pretty typical friendship: they joke around, cheer each other on, and keep ...
-

First-of-its-kind pressurization test could improve Ross procedure outcomes
The Ross procedure is a preferred surgery to treat severe aortic valve disease. The procedure replaces the failing valve ...
-

Four things you should know about MAPCAs treatment
As the first grandchild in her family, Hannah Homan is in demand for frequent visits. She was also the focus ...