A complex repair for Ruby’s heart

When Rebecca and Michael Stewart learned their baby would be born with a congenital heart condition, they reacted as any expectant parents would, with shock and fear. But they quickly moved into action, focused on finding the best care for their daughter before her birth.
“At about 22 weeks into my pregnancy, Ruby was diagnosed with truncus arteriosis and an interrupted arch,” says Rebecca. “Her condition was very severe, so our local doctors referred us to a larger hospital in Charleston, South Carolina, and we met with the surgeons there.”
However, Rebecca, who is a nurse, was concerned with the limited number of truncus patients treated at the hospital every year. The couple decided to begin looking for a second opinion at a hospital that had a higher volume of patients and more experience with the surgery.
A second opinion in Boston for truncus arteriosis surgery
“We reached out to Boston Children’s Hospital, and had a phone consult with Dr. Wayne Tworetzky, director of the Fetal Cardiology Program,” says Rebecca. “As soon as we got off the phone with Dr. Tworetzky, I told my husband, ‘We’re going to Boston.’”
Rebecca was impressed with Dr. Tworetzky’s knowledge and transparency in discussing Ruby’s condition, as well as with the number of patients successfully treated at the hospital each year. “As a nurse, I really appreciated that Dr. Tworetzky spoke with me at my level. He didn’t sugarcoat anything, but was personable and honest.”
The couple made plans to travel to Boston for Ruby’s delivery in January of 2020, as Rebecca approached her 37th week of pregnancy.
A team approach
“We met with the whole team over two days, including Dr. Christopher Baird, the surgeon who would be performing Ruby’s surgery,” says Rebecca. “He does a lot of work on arches and valves, and he was really great. We felt like we were in very good hands.”

The team came up with a plan to induce Rebecca at 39 weeks. On January 28, Ruby was born at 8 pounds. She was scheduled for surgery the next day, on January 29.
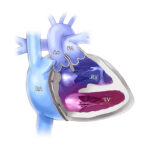
The surgery involved patching her interrupted aortic arch, closing a ventricular septal defect (VSD), placing a conduit, and manipulating her truncal valve to reduce leaking.
“During surgery, we found there was an additional large muscular ventricular septal defect that would have been difficult to reach surgically,” says Dr. Tworetzky. “To address this issue, Dr. Nicola Maschietto from our Cardiac Catheterization Program placed a ventricular septal defect closure device under ultrasound guidance. This was a true collaborative effort between cardiac surgery, interventional cath, and imaging.”
‘The best experience ever’
“It was a long, complex surgery, but Dr. Baird was very pleased with the outcome, and Ruby did great,” says Rebecca. “It was the best experience ever. Every single person we met in Boston was amazing and treated us so well,” says Rebecca. “It was especially noticeable to me as a nurse, since I’m used to caring for other people. The culture of the team in Boston was amazing to me, just awesome.”
Three weeks later, the family was on a plane bound for home, and Ruby’s big brother, Matthew, got to hold her for the first time.

Thriving and meeting milestones
Now, nearly 6 months old, Ruby is growing, meeting milestones, laughing, and talking. Rebecca says you’d never know she was born with a heart condition. “She’s such a sweet, loving baby, you’d never know how much she’s been through in her short life. She’s our miracle baby.”
At some point, Ruby will need to travel back to Boston to have her conduit replaced, most likely when she’s 2 or 3. Until then, she’s being followed by her local cardiologist, who shares her test results with Dr. Baird and her team in Boston.
“We feel like we have a great team supporting us,” says Rebecca. “I would highly recommend the team in Boston to anyone, especially anyone who is afraid or concerned. It’s the best choice we ever made.”
Learn more about the Fetal Cardiology Program, the Department of Cardiac Surgery, and the Maternal Fetal Care Center.
Related Posts :
-

Biventricular repair linked to better outcomes in superior-inferior ventricles treatment
The complexity of superior-inferior ventricles — a condition in which one ventricle is positioned on top of the other — has often ...
-

A reunion of the heart: Grace and Amy bond through HLHS
At first glance, Grace and Amy have a pretty typical friendship: they joke around, cheer each other on, and keep ...
-

First-of-its-kind pressurization test could improve Ross procedure outcomes
The Ross procedure is a preferred surgery to treat severe aortic valve disease. The procedure replaces the failing valve ...
-

Four things you should know about MAPCAs treatment
As the first grandchild in her family, Hannah Homan is in demand for frequent visits. She was also the focus ...