Biventricular repair linked to better outcomes in superior-inferior ventricles treatment
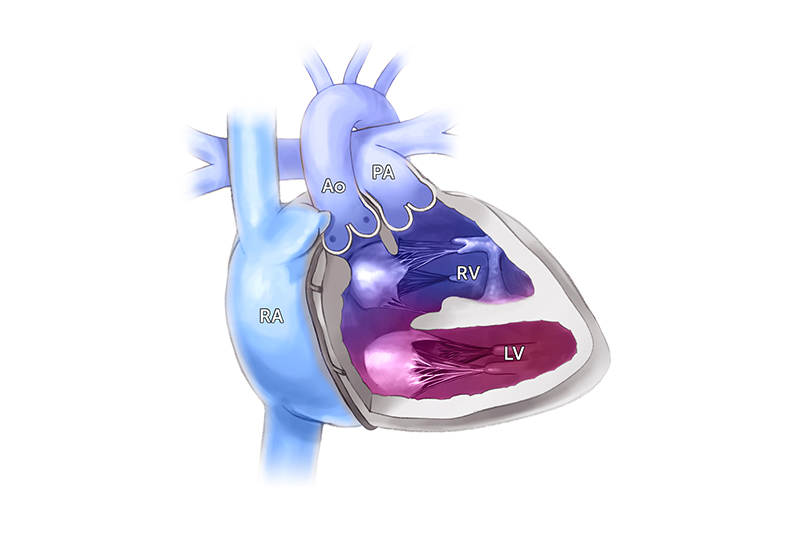
The complexity of superior-inferior ventricles — a condition in which one ventricle is positioned on top of the other — has often limited surgical treatment.
But Boston Children’s heart specialists recognized an opportunity to make treatment for the rare condition more accessible to children. Their solution has been a procedure the hospital is at the forefront of developing: biventricular repair.
By using surgical techniques they’ve devised and by making the most of advanced surgical planning tools such as 3D modeling of the heart, they’ve found that biventricular repair can improve the outcomes of superior-inferior ventricles treatment. In fact, their new research indicates it might be more effective at treating the condition than single-ventricle surgery.
“Superior-inferior ventricles are a challenge because the left ventricle is often unnaturally far away from the aorta, and that poses a significant hurdle for any kind of reconstruction,” says cardiac surgeon Sitaram Emani, MD. “But we’ve developed techniques to overcome that and make biventricular repair feasible for more children.”
Single-ventricle surgery has limitations
With even the most complex congenital heart defects (CHDs), the left and right ventricles are still almost side by side, allowing surgeons to take advantage of that close positioning when rerouting or separating blood flow as part of a repair. But surgeons don’t have that advantage when they need to reconfigure blood flow to treat superior-inferior ventricles — which can significantly affect blood flow and is associated with complex CHDs such as transposition of the great arteries (TGA) and double outlet right ventricle (DORV).
“With superior-inferior ventricles, the heart is twisted in a way that the ventricles are in different locations, and that makes it difficult to understand blood outflow and how to create a pathway connection from a ventricle to the arteries,” says cardiologist Rebecca Beroukhim, MD. “It’s hard to visualize that spatial relationship when planning surgery.”
When heart specialists think that creating a biventricular circulation is too complicated and potentially risky, they often recommend single-ventricle surgery, which includes the Fontan procedure. But while that surgery initially has less risk, single-ventricle circulation can cause health issues later in life. A Boston Children’s study of 10 years’ worth of patient outcomes for several conditions confirmed that single-ventricle circulation was more associated with the onset of liver disease than biventricular circulation.
That study validated Boston Children’s heart specialists’ longstanding belief that biventricular repair is the preferred approach when possible. Their constant development of the procedure means more patients with complex conditions can benefit from a biventricular circulation or even a one-and-a-half ventricular circulation.
Study shows advantages of biventricular repair
As co-directors of Boston Children’s Complex Biventricular Repair Program, Beroukhim and Emani wanted to verify if that approach also made sense for the treatment of superior-inferior ventricles. “Over the years, we shifted our treatment strategy for the condition from single-ventricle management to biventricular repair,” Emani says. “So we wanted to understand and confirm whether it had benefits.”
Their recent study of 119 patients — published in the Journal of the American College of Cardiology — found that biventricular repair is, in fact, feasible in children who have superior-inferior ventricles. Over the long term, patients who had biventricular repair experienced better outcomes, including not needing a heart transplant, than those who had single-ventricle surgery.
Even though the ventricles are in a unique position, quite often they are healthy and normal-sized, making those patients ideal candidates for biventricular repair.
“If a child has two good-sized ventricles, it’s better to use them both in circulation, which will help prevent the long-term complications that we see in Fontan patients,” Beroukhim says.
3D models and proven techniques make a difference
The challenge, then, is overcoming the complexity of surgery. Beroukhim, Emani, and their Heart Center colleagues believe they have done that by simplifying the process. First, advanced 3D modeling of a patient’s heart anatomy and the computer simulation of blood flow gives surgeons a detailed visual guide to how they can reconstruct a superior-inferior ventricular anatomy with precision. “It helps us understand what the spatial relationships of the ventricles and arteries are,” Beroukhim says.
In the operating room, Emani and the surgery team use biventricular repair techniques they’ve developed or refined, including the baffling of a heart wall to redirect blood flow, the repositioning of the aorta or pulmonary artery roots, and the resection of obstructing tissue. Also, as members of the Congenital Heart Valve Program, the surgeons have experience repairing valves, which Emani says can be a challenge with superior-inferior ventricles.
The study compared only five years’ worth of outcomes, but Beroukhim and Emani say the findings still show great promise in what biventricular repair can do for superior-inferior ventricles — especially if a child’s ventricles are properly sized and can handle the work of a biventricular blood flow.
“The technical complexity of surgery shouldn’t be a deterrent for biventricular repair,” Beroukhim says.
Refer a patient to the Complex Biventricular Repair Program.
Related Posts :
-

Conduction tissue mapping is shown to significantly reduce heart block
New research by Boston Children’s validates an innovative approach to mapping the heart’s invisible conduction tissue during surgery. ...
-

Every heart has a story. See how we care for them all.
It’s easy to think of the heart as a common denominator — everyone has one — but no two hearts are ...
-

A surgeon's last-minute trip to Sri Lanka reduces children's wait for needed heart repair
Last year, Dr. Christopher Baird got an offer he couldn’t refuse — something that happens often as he travels the ...
-

Treatment for a complex congenital heart defect gives Alyvia 'endless energy'
She may be just 3 years old, but Alyvia Parker is already making a difference for other kids with congenital ...





