PICU Up! Program aims to increase mobility in ICUs

For decades, clinicians believed the most appropriate care for critically ill pediatric patients was sedation and rest. But in recent years, the tides have changed. Studies in adults have shown that sedation and immobility lead to increased mortality and morbidity, longer stays in the intensive care unit (ICU), increased risk of ICU delirium, and a longer time on a ventilator. Many researchers believe the same risks hold true for pediatric patients.
Based on this emerging data, the PICU Up! Program at Boston Children’s Hospital aims to increase mobility in even the sickest patients and to begin to move the dial on changing the culture of care in the ICU.
“The PICU Up! Program was created by Sapna Kudchadkar, MD, PhD, at Johns Hopkins University several years ago,” says Sarah Goldberg, MD, Cardiac Intensive Care Unit (CICU) physician and PICU Up! representative at Boston Children’s. “When clinicians at Boston Children’s learned about the program, they thought it would be a nice fit here.”
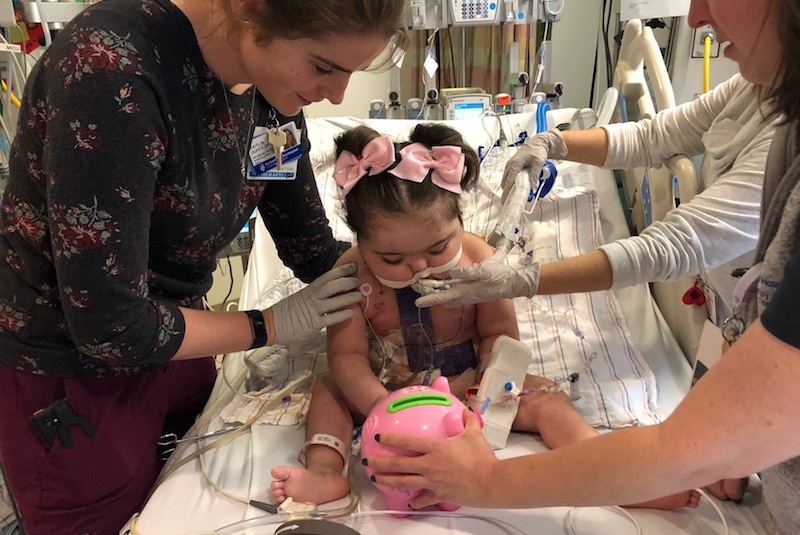
The effort to bring PICU Up! To Boston Children’s Hospital was spearheaded by Megan Geno, PT, DPT, PCS, from the Department of Physical and Occupational Therapy and Mary-Jeanne Manning, MSN, APRN, PNP-BC, CCRN, from the Medical-Surgical Intensive Care Unit (MSICU). Goldberg got involved in the program about a year ago, based on her research interest in ICU delirium, which the program hopes to reduce.
Algorithm assigns levels of illness and appropriate interventions
“A major part of the program is an algorithm that assigns patients to specific levels of illness, from 1 to 3, which prescribes the level of interventions that patient should be getting,” says Goldberg. “For example, even with the level 1 patients, the most critically ill, there are small interventions we can do to increase their mobility are awareness, such as repositioning them every two hours and elevating their head. We also introduce physical and occupational therapy, and try to orient them to day/night cycles.”
As patients move up to levels 2 and 3, the amount of mobility and rehabilitation increases. Clinicians from multiple disciplines work together to help patients gain strength and recover. “It’s really about shifting the culture to empower the staff to help patients be more active and get them off of sedating medications,” says Goldberg. “With this program, even patients who are ventilated are able to do more, including sitting up in chairs and possibly standing. That’s something I didn’t see a few years ago. People are getting much more comfortable with the idea.”
Goldberg talks about highlights of the program.
New study looks at strategies and outcomes
The CICU and MSICU at Boston Children’s recently started participating in a pilot stepped-wedge multicenter randomized study started at Johns Hopkins to investigate the implementation strategies for an early mobility program in ICU as well as short-term outcomes.
There are three hospitals formally participating in the trial with Johns Hopkins. “We’re the only cardiac ICU in the entire study, which makes us a little unique,” says Goldberg, who is the CICU site principal investigator for the study. “It will be the first study looking at rehabilitation practices in the pediatric setting in terms of outcomes and the first time we’re going to have a large enough patient population to say that this actually created positive outcomes for patients. It’s very important in changing the overall culture of pediatric intensive care.”
Read more clinical care updates from Boston Children’s.
Related Posts :
-

A reunion of the heart: Grace and Amy bond through HLHS
At first glance, Grace and Amy have a pretty typical friendship: they joke around, cheer each other on, and keep ...
-

First-of-its-kind pressurization test could improve Ross procedure outcomes
The Ross procedure is a preferred surgery to treat severe aortic valve disease. The procedure replaces the failing valve ...
-

Four things you should know about MAPCAs treatment
As the first grandchild in her family, Hannah Homan is in demand for frequent visits. She was also the focus ...
-

Treating MAPCAs with unifocalization surgery and cardiology care
Children born with a rare form of tetralogy of Fallot (ToF) face a challenging type of congenital heart ...