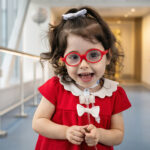
Incredible Teddy: Thriving with CDH

Andi Lodico left for the hospital at 1 a.m., in labor with her second child. She didn’t return home for two months. Just a few weeks earlier, she and her husband, Phil, had been at a routine ultrasound appointment when they received some troubling news. Their baby, Teddy, appeared to have a rare and potentially life-threatening condition called congenital diaphragmatic hernia (CDH). In CDH, a hole is present in the diaphragm, the muscle that the body uses to breathe. This can cause the intestines and other abdominal organs to move into the chest, which prevents normal lung development.
“The doctor told us that I should plan to deliver in a major hospital in Boston or Philadelphia,” says Andi. In the meantime, she and Phil traveled some 40 miles from their home to Albany for further testing. There, the news was more promising: “They said that the diagnosis of CDH was a false positive and that Teddy would be fine,” she remembers. “We held on to that assumption and stayed in New York.”

A juggling act
But almost as soon as Teddy was born, it was clear that something was very wrong. Even though he was full term and appeared healthy, he couldn’t breathe on his own, had pulmonary hypertension, and was placed on a ventilator. When he was just 12 hours old, the infant was transported to Boston Children’s Hospital. With no room in the air ambulance, Andi and Phil had to follow by car, giving their permission to put their son on extracorporeal membrane oxygenation (ECMO), advanced technology that functions as a replacement for a critically ill child’s heart and lungs while they await surgery.
Once the couple arrived, the reality of the situation sunk in. “I had thought we could all go home in a few days,” says Andi. “The doctors told us to plan to be there at least a few months.” The anxiety of having an extremely sick infant combined with the stress of being away from their daughter, Esther, then only a toddler herself. “I suddenly started wondering how we could possibly manage it all,” she admits. “I began to feel anxious that we had been sent to Boston and were now three hours away from home.”

‘In the most amazing place’
That anxiety soon melted into gratitude. “The doctors were so confident and reassuring, and the nurses were very nurturing, both to Teddy and to us,” says Andi. “We were blown away that everyone considered our needs as a family, too — we knew we were in the most amazing place.”
While a social worker helped the Lodicos get settled at the Yawkey Family Inn and a child life specialist helped support their daughter, Teddy’s care team formulated a plan. At two days old, he underwent surgery to repair the CDH. On July 4, he was able to come off ECMO — “a really meaningful Independence Day,” says Andi.
After two months in the hospital, Teddy finally went home. “We were used to so much clinical support, so it was a little scary,” says Andi. “But ultimately, we felt very confident because Teddy had fought through everything he had faced so far. We knew there was something really special about him.”

Paying it forward
Now 9 years old, Teddy loves reading, skiing, swimming, playing baseball, and riding his bike. There have been no signs of pulmonary hypertension or re-herniation since his surgery, and he only has to return to the CDH Program’s clinic — as well as to cardiologist Dr. Mary Mullen in the Pulmonary Hypertension Program — every couple of years. Esther is both protective and proud of Teddy, as his is younger brother, Tucker. “It’s hard to believe how great he’s doing,” says Andi. “We’ve nicknamed him Incredible Teddy.”
Today, the family is paying their good fortune forward through the aptly named Incredible Teddy Foundation, a nonprofit that raises awareness about CDH and provides financial assistance to eligible families. “It’s easy to go into debt from the costs associated with long hospitalization,” says Andi. “We want to help ease that hardship for other families.”
Learn about the CDH Program.
Related Posts :
-

The ‘Trach Chapter’: Isabella’s journey with bronchopulmonary dysplasia
Isabella’s life has been anything but ordinary. Born at just 27 weeks gestation and weighing only 1 pound, 4 ounces, Isabella has ...
-

A unique marker for pericytes could help forge a new path for pulmonary hypertension care
Pulmonary arterial hypertension (PAH) is a rare condition that’s difficult to treat. The hallmarks of the disease — narrowing of ...
-

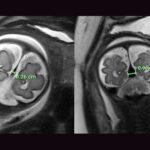
Could the falcine sinus hold the key to vein of Galen outcomes?
A Boston Children’s Hospital study uncovers how fetal magnetic resonance imaging (MRI) could be a game-changer in predicting outcomes ...
-

Modifying macrophages in the lung could head off pulmonary hypertension
In the 1980s, when Stella Kourembanas, MD, began her career in neonatology, she cared for newborns with pulmonary hypertension, a ...