Thinking – and operating – outside the box: Bypassing Saoirse’s aneurysm

Saoirse just turned 3. There was a big to-do for her birthday, complete with family flying to Massachusetts from Ireland for the occasion. The celebration was big because Saoirse has a lot to celebrate. About six months ago, doctors discovered an unstable aneurysm in her brain, and within days she underwent surgery to treat the bulging blood vessel. Today, thanks to a bold approach to treatment by Dr. Alfred See and others in the Cerebrovascular Surgery and Interventions Center (CSIC) at Boston Children’s Hospital, Saoirse is healthy, happy, and living her best 3-year-old life.
“Mama, my head hurts”
Saoirse’s mom, Jess, didn’t think too much of it when Saoirse started complaining of headaches last fall. Saoirse also had a low-grade fever and nausea, so Jess assumed it was a virus. But she got nervous when Saoirse still complained of headaches even after the fever and nausea faded.
“She’d say, ‘Mama, my head hurts,’” Jess says. “I’d ask where, and she would always — every single time — point right to the front of her head.”
Jess consulted Saoirse’s pediatrician, who agreed that ongoing headaches in a child that age was uncommon and referred them to the CSIC team to obtain an MRI. Almost immediately after Saoirse’s scan, Dr. See and CSIC co-director, Dr. Ed Smith, came out to discuss the results. They said that the MRI scan showed ballooning in a vessel on the right side of Saoirse’s brain that had the potential to rupture — a condition known as a hemorrhagic stroke. They recommended immediate treatment.
Bypassing traditional aneurysm surgery
One of the most common interventions for aneurysms is clipping, where a metal clip is placed across the affected part of the vessel to cut off its blood supply. In children, however, aneurysms often affect the whole blood vessel, not just one part. In these cases, the clip needs to block normal blood vessel to treat the aneurysm. Although clipping is effective, it can increase the risk of ischemic stroke because the blocked vessel doesn’t allow enough blood flow to reach the area of the brain beyond it.
To help prevent such a stroke, neurosurgeons often use an approach called revascularization, or STA-MCA bypass. STA-MCA bypass takes the superficial temporal artery (STA), which lies next to the scalp, and attaches it to the middle cerebral artery (MCA) in the brain. This new connection creates a pathway for blood flow, helping prevent stroke or brain damage. Dr. See felt bypass was the best option for Saoirse because it potentially mitigated her two biggest risks: rupture of the aneurysm and stroke from restricted blood flow.
“We could have prioritized just clipping the aneurysm, which was the most obvious and probably the most life-threatening risk,” Dr. See says. “But if we didn’t also consider preventing a stroke, we could have left her with new deficits.”
But there was one caveat: bypass is a common surgical approach in adult patients but extremely rare in children, partly due to how small their blood vessels are and the length of the surgery.
“Historically, bypass on a child as young as Saoirse wouldn’t be attempted, or would be something where you might ask an adult-care neurosurgeon to do it alongside the pediatrics team,” says Dr. See. “Whereas, at Boston Children’s — given our volume and our expertise — we can keep it all in-house. And with Saoirse, Dr. Smith and I both saw her in clinic and followed her day in and day out, so we knew her pretty well. This really helped when it came time to do the bypass; with her it seemed reasonable to attempt the bypass option, even though that meant that it would be a longer surgery than if we just clipped her aneurysm.”
At first, the idea of taking such an advanced approach was daunting to Jess and her husband, Paul, but Dr. See and the CSIC team discussed the process in detail.
“Dr. See explained to us that bypass would give her the best outcome; he was willing to go the extra mile and beyond,” Jess says.
Thriving and grateful after surgery

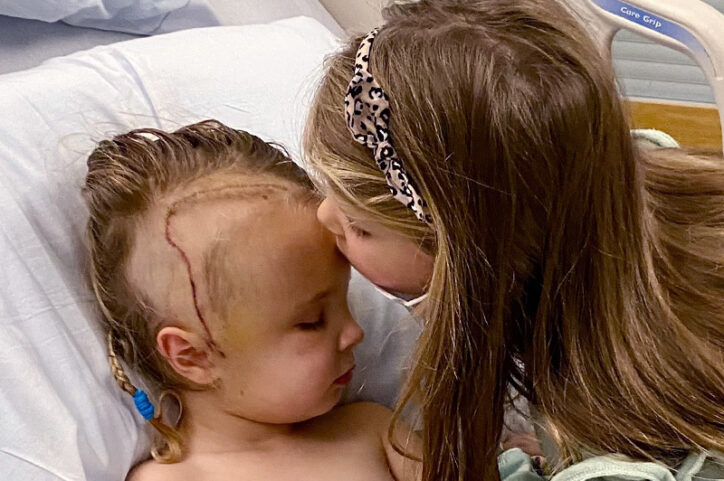
After traditional aneurysm clipping, physical or cognitive deficits — including attention, memory, and executive functioning problems — are common due to lack of blood flow to the brain. Saoirse, however, was on her feet within days and home shortly after. Today, she’s back to all her favorite activities, including skiing, swimming, gymnastics, and playing with her older sister, Aoife. Jess credits Saoirse’s quick recovery to Dr. See’s decision and confidence in doing a bypass.
“It’s completely miraculous,” Jess says. “All because they did this heroic surgery on a 2-year-old.” She adds that it almost feels like the experience never even happened.
“We’re forever in his debt,“ she continues. “We gave him our daughter, and he gave her right back to us in the same shape.”
Learn more about how we treat aneurysms at the Cerebrovascular Surgery and Interventions Center.
Related Posts :
-

Varsity blues: How AVM radiation therapy got Greta back to sports
Want to find Greta? Try the hockey rink, or softball field, or volleyball court. Where won’t you find her? ...
-

Austin’s story: Raising awareness after treatment for pediatric stroke
In May, 11-year-old Austin Rizzo led the pack in a two-mile road race of his own creation. But the race, ...
-

Years in the making: Team performs successful fetal intervention for VOGM
On an ordinary Wednesday in March, a team of specialists from two institutions made the extraordinary happen: a first-of-its-kind intervention ...
-

Changing the world: Baby Denver leads the way after first-of-its-kind procedure for VOGM
Denver Coleman is less than 2 months old, but she’s already helped blaze a trail for other children and families, ...