Inspired research in newborn lung disease: Stella Kourembanas, MD
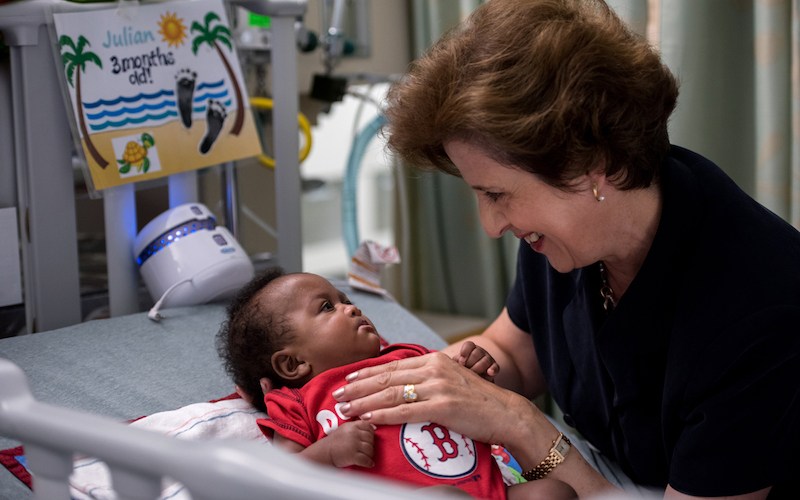
Stella Kourembanas in the NICU with Julian (photos: Katherine Cohen)
During the NICU rotation of her clinical training, Stella Kourembanas, MD, sat at the bedside of newborn babies with hypoxia. The newborns weren’t getting enough oxygen and were suffering from pulmonary hypertension — abnormally elevated blood pressure in the lung’s blood vessels. What was triggering these patients’ disease?
Kourembanas decided her fellowship research would focus on determining how hypoxia triggers the blood vessels to become abnormal. She built her career, showing how hypoxia affects the endothelial cells that line blood vessels: what genes are turned on, how they regulate interaction between cells and how that affects the lung vasculature.
My research in the lab is driven by what I see at the bedside. What drives me right now is to find a cure for bronchopulmonary dysplasia. Working in the NICU, you get inspired.
As a physician scientist, she has contributed to the improvement of outcomes for pulmonary hypertension. Much has changed since she began her research in the 1980s. “Pulmonary hypertension had an 85 percent mortality,” she says. “If you fast forward to today, the mortality is less than 10 percent.”
In recent years, Kourembanas has focused on finding an effective treatment for bronchopulmonary dysplasia (BPD), a chronic lung disease of infants, especially preterm infants. Because advanced neonatal care is allowing smaller and smaller preterm babies to survive, the rate of BPD is increasing.

Because their lungs are underdeveloped, premature infants need mechanical support to breathe. But providing oxygen artificially to underdeveloped lung tissue can cause it to stretch, thicken, scar and become inflamed, leaving babies with BPD more susceptible to future chronic lung disease and increased rates of hospitalization due to flu, asthma and other respiratory problems. The tissue damage can result in stunted or arrested lung development, which in turn affects development of the other major organs, the most vulnerable being the brain. Treatments have been helpful, but not curative.
Stem cell factors to reverse lung injury
Kourembanas’s current research is looking at how stem-cell-based therapies can be used to redirect or reprogram lung tissue development. Working with mesenchymal stem cells isolated from the umbilical cord of newborns, she has found that the signaling factors from the cells’ exosomes (microscopic packets of proteins, nucleic acids and other materials) stimulate normal cell development and have the potential to reverse lung injury.
Kourembanas intends to take these discoveries from her laboratory’s collaborations and bring them to clinical application. “What drives me right now, what inspires me is to find a cure for BPD,” she says. “If I can make an impact on BPD, I will feel like I contributed something. It’s the work of many people. My research in the lab is driven by what I see at the bedside. Working in the NICU, you get inspired. It’s just an unparalleled environment.”
Related Posts :
-

The ‘Trach Chapter’: Isabella’s journey with bronchopulmonary dysplasia
Isabella’s life has been anything but ordinary. Born at just 27 weeks gestation and weighing only 1 pound, 4 ounces, Isabella has ...
-

Modifying macrophages in the lung could head off pulmonary hypertension
In the 1980s, when Stella Kourembanas, MD, began her career in neonatology, she cared for newborns with pulmonary hypertension, a ...
-

My son is a NICU GraD: Here’s what I’ve learned
My husband and I aren’t first-time parents, but when our twins were born nine weeks early a year ago, ...
-

Mending injured hearts: Lessons from newborns?
When the heart is injured, as in a myocardial infarction, the damaged heart muscle cannot regenerate — instead, scar tissue forms. ...