PDA transcatheter closure in preemies

The problem of how to close a patent ductus arteriosus (PDA) in premature babies is not new. Medications don’t always work and surgery can be associated with substantial risk for these vulnerable patients. This has led many neonatologists to recommend that the PDA not be closed until a child is older, or to wait for it to close spontaneously.
A novel approach offers new options
But a new transcatheter approach has been a successful option for some preemies with PDA. And a team of clinicians at Boston Children’s Hospital is one of the first in the country — and the only in New England — to be trained on the procedure using a new device, the Amplatzer Piccolo by Abbott, after it was granted FDA approval in January 2019.
“We have been using a transcatheter approach to close the ductus in older children for many years, but the devices were all too large for the preemie population,” says Diego Porras, MD, chief of the Cardiac Catheterization Program at Boston Children’s. “This device is smaller than the size of a pea, and clinical trials found it was safe for use in preemies.”
A dedicated team offers expertise
However, he says that because this population of preemies is so vulnerable, the company released the product only to specific centers, including Boston Children’s. “They asked us to create a dedicated team to be trained in the procedure,” says Porras.
Joining Porras on the team is cardiologist Kevin Friedman, MD, who runs echocardiography during the procedure; Francis Fynn-Thompson, MD, cardiac surgeon; Kimberly Chamberlain, CPNP; Philip Levy, MD, neonatologist; and Juan Ibla, MD, cardiac anesthesiologist.
The team received training and started offering the approach as an option for PDA closure in preemies in 2019. So far, they have performed the procedure on a handful of patients.
“if someone at another hospital decides they want a ductus closed, they call us, and we get imaging from them or get imaging here and look at it to see if they are a candidate anatomically,” says Porras. “If they are, we bring the patient over into our NICU. Usually we transport them the day before, get them settled, and then do the catheterization procedure the next day.”
“Normally, closing the PDA, you use artery and vein access, but these patients are so small that arterial access would increase the risk substantially,” explains Porras. “So the way you have to do it is solely through the vein. This means a lot of the procedure is guided through echocardiography instead of angiography.”
“We’re just starting our experience here, but we’ve already performed the procedure on seven patients under 2 kilograms and another 4 or 5 above 2 kilograms.”
Diego Porras, MD
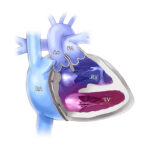
He says that another procedural difference in this population is where the device is placed. “With older patients, a disc is placed inside the aorta through the pulmonary artery, which isn’t possible with small preemies. In these patients, we place the whole device inside of the ductus in order to avoid obstructing the aorta or the left pulmonary artery. So we need to be careful to position it in exactly the correct spot and make sure it’s secure while it’s still attached to the delivery cable.”
Once the device has been placed, it remains in the body, so there is no need to go back in and replace it later in life. It’s made of Nitinol, a titanium-nickel alloy that is MRI compatible, an important consideration for premature patients.
Minimizing stress to vulnerable infants
Porras says the procedure is pretty quick, “What we’ve seen is that once venous access is secured, it takes less than 15 minutes in average to complete the procedure, which minimizes the stress in this vulnerable population.”
Another benefit of the procedure is it carries less risk of bleeding. “With most caths we do, we give the patient heparin, but these patients are so small that we try to do the procedure quickly and not give any blood thinners, further reducing the risk of bleeding.”
Porras says the weight indication for the device is from 700 grams to 2 kilograms, though he says it’s possible to perform the procedure on preemies who weigh less.
“We’re just starting our experience here, but we’ve already performed the procedure on seven patients under 2 kilograms and another 4 or 5 above 2 kilograms,” he says. “So far, all the PDAs have been closed safely and the patients have done well after the procedure.” Porras says the ideal time range for placement is 2 to 3 weeks of age, but older patients are also candidates. “The hope is that, as we learn more about this procedure and increase the number of cases, we will be able to show that this may be a safer, minimally-invasive option to close the PDA in preemies,” says Porras.
Learn more about the Cardiac Catheterization Program.
Related Posts :
-

Biventricular repair linked to better outcomes in superior-inferior ventricles treatment
The complexity of superior-inferior ventricles — a condition in which one ventricle is positioned on top of the other — has often ...
-

A reunion of the heart: Grace and Amy bond through HLHS
At first glance, Grace and Amy have a pretty typical friendship: they joke around, cheer each other on, and keep ...
-

First-of-its-kind pressurization test could improve Ross procedure outcomes
The Ross procedure is a preferred surgery to treat severe aortic valve disease. The procedure replaces the failing valve ...
-

Four things you should know about MAPCAs treatment
As the first grandchild in her family, Hannah Homan is in demand for frequent visits. She was also the focus ...