Ellery’s story: The mystery of opsoclonus myoclonus syndrome

Ellery was a normally developing 2-year-old when her skills took a dramatic shift backwards last winter. “She started wobbling when she walked, like someone who had had a few beers,” says her mom, Maura. “Then she developed tremors in her hands, couldn’t put a spoon to her mouth and she stopped playing with any of her toys.”
Confused and concerned, Maura and her husband, Brad, brought Ellery to her pediatrician. “At first, her doctor thought maybe she had ingested something by mistake, but all the tests came back negative,” says Maura.
A fall leads to more testing — and a diagnosis
Ellery’s gross and fine motor skills continued to steadily decline, until she fell at daycare and Maura received a call from her provider, concerned Ellery might have a concussion. A follow-up visit with her pediatrician and further testing at Boston Children’s Hospital — including a brain MRI and lumbar puncture — yielded no answers. Ellery didn’t have a concussion, but there was still no clear answer as to what was causing her mysterious symptoms.
Yet, it was clear something was wrong, and Ellery was admitted to Boston Children’s for further observation and testing. After a three-day inpatient stay, she was diagnosed with acute cerebellar ataxia. “The doctors explained her symptoms are in line with this diagnosis and it is caused by a virus. We were told it typically resolves itself and we should see improvement in a week or two,” says Maura. “They sent her home with appointments for both physical therapy (PT) and occupational therapy (OT), and a follow-up appointment with neurology in three months.”

Rage attacks raise new questions
But after a week Ellery wasn’t improving — in fact, she seemed to be getting worse. “She started having frequent rage attacks, lasting up to three hours and we were unable to console her or distract her. Along with the daytime rage, she would wake up multiple times in the middle of the night in fits of rage. No one was sleeping and we were desperate for more answers,” says Maura. Since Ellery had always been a laidback kid and a great sleeper, Maura and Brad knew something was terribly wrong.
They called the Neurology Department and got an earlier appointment with Boston Children’s neurologist Dr. Elizabeth Barkoudah. It was her last appointment on the Friday before Christmas.
“Dr. Barkoudah confirmed that Ellery had all the signs of acute cerebellar ataxia, but told us to call right away if we noticed any rapid eye movement.”
While spending Christmas with family, Ellery declined even more — having sustained rage attacks and unable to walk, eat, or speak clearly — not a typical toddler during the holidays. “We got home the day after Christmas, and Ellery told us she wanted to go to sleep before she ate dinner, so I laid down with her in bedroom and saw her eyes fluttering back and forth rapidly. It was terrifying,” says Maura. “I was able to get it on video and sent it to the neurologist on call, who told us to come to the emergency room right away.”
A new diagnosis: Opsoclonus myoclonus syndrome
Once at Boston Children’s, Ellery was diagnosed with opsoclonus myoclonus syndrome (OMS), a rare neurological condition. The next day, they met with Dr. Mark Gorman, a neurologist who specializes in OMS.
“Dr. Gorman told us that in about 50 percent of kids with OMS, the condition is caused by a neuroblastoma, a type of cancerous tumor,” says Maura. “So they did a full-body MRI at the time and then another follow-up in August, which did not show any evidence of a neuroblastoma. So, Ellery’s cause of OMS is likely due to an autoimmune response where her body’s immune system attacked her cerebellum.”
Of note, Maura has type 1 diabetes, which is also an autoimmune condition. Dr. Gorman says this might be more than a coincidence. “We think there may be a genetic component to OMS and are conducting a research study looking at family history of autoimmune disorders paired with sophisticated genetic analyses using whole genome sequencing of children with OMS and their parents. We have found a higher rate of autoimmune disorders in first- and second-degree relatives of children with OMS.”
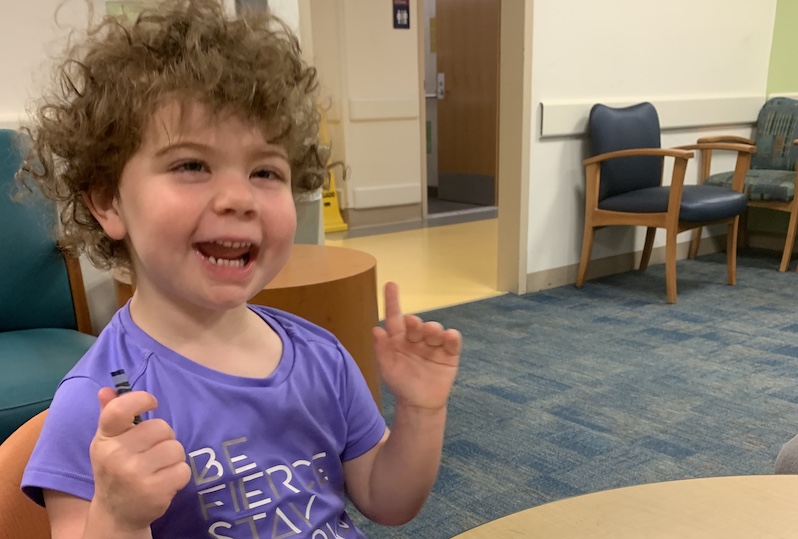
Return to home and school
After ringing in the New Year in the hospital, Ellery was able to return home after a 10-day inpatient stay. She still had a PICC line to deliver the intravenous immune globulin (IVIG) and steroids she needed for treatment. With the help of family and friends, Maura and Brad navigated the next few months caring for Ellery in their Boston apartment. Because Ellery was still having symptoms, it wasn’t safe for her to return to daycare, but she was doing weekly PT and OT.
It was a slow process, but gradually Maura and Brad saw incremental improvement. “She slowly became steadier on her feet, and wasn’t having so many rage attacks,” says Maura. Once a week, Maura and Ellery would visit her daycare so she could practice walking and playing with her friends.

At the beginning of May, Ellery returned to daycare. These days, she can walk, run, and jump. “That first jump was the best thing I ever saw,” says Maura. She still has a significant tremor and struggles with balance and other fine motor skills, but is working on it in OT and PT. “It’s frustrating for her because she loves playing with small horse figurines, her favorite toys,” says Maura. “But she’s found ways to make it work within her limits and she doesn’t give up.”
Ellery no longer has a PICC line, but visits the infusion center every four weeks for her IVIG and takes daily oral steroids. She also recently received a second round of treatment, called rituximab. Dr. Gorman hopes the combination of treatments will help combat her symptoms.
“She takes a few steps forward and then slides back a bit,” says Maura. “We’ve learned from Dr. Gorman that’s typical for others with OMS. But she’s done better than I thought she would. She is laughing, smiling and playing. We didn’t think we would ever see that again.”
Looking to the future
The long-term goal is for Ellery to be symptom- and medication-free. “There’s not a clear path to that goal, because OMS is such a rare disease and no two cases are alike,” says Maura. “But we are taking each step of progress as a milestone towards that goal.”
Children with OMS face a high risk of cognitive impairment and learning difficulties, and only time will tell what long-term effects Ellery will face. There will always be a risk for a relapse and each relapse can have a lasting impact on her cognitive function. To support Ellery’s cognition and learning, Dr. Gorman’s educational specialist, Catherine “Kitty” Petty, has helped the family enroll Ellery in an integrated preschool program that caters to her learning style and physical needs.
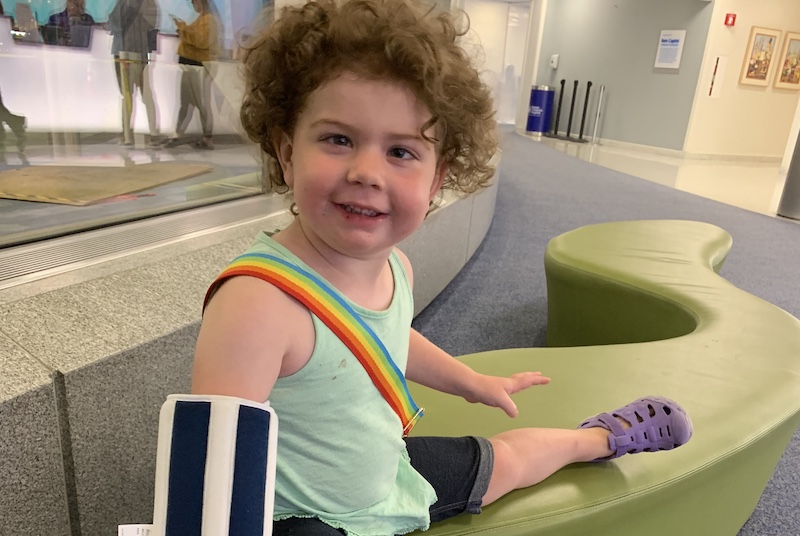
“We credit Dr. Gorman and everyone at Boston Children’s Hospital for the fact that she was diagnosed and began treatment so quickly,” says Maura. “I always tell people how fortunate we are to live in Boston. I’m not sure where we’d be right now if we lived somewhere else.”
Learn more about the Department of Neurology.
Related Posts :
-

A case for Kennedy — and for rapid genomic testing in every NICU
Kennedy was born in August 2025 after what her parents, John and Diana, describe as an uneventful pregnancy. Soon after delivery, ...
-

The journey to a treatment for hereditary spastic paraplegia
In 2016, Darius Ebrahimi-Fakhari, MD, PhD, then a neurology fellow at Boston Children’s Hospital, met two little girls with spasticity ...
-

The dopamine reset: Restoring what’s missing in AADC deficiency
In March 2023, a young girl came to Boston Children’s Hospital unable to hold up her head — one striking symptom ...
-

Thanks to Carter and his family, people are talking about spastic paraplegia
Nine-year-old Carter may be the most devoted — and popular — sports fan in his Connecticut town. “He loves all sports,” ...





