One in 5 million: Nathan’s rare diagnosis and happy recovery

Nathan Asselin was a happy baby with no apparent health problems when he became ill just before his birthday in April of this year.
“He didn’t seem himself the night before, then he woke up with a fever on the day of his birthday,” says his mother, Danielle. “He sat on the floor eating his birthday cake, but we could tell he didn’t feel well.”
Initial COVID-19 concerns
Initially, Danielle and her husband, Nicholas, worried that maybe Nathan had coronavirus, but then his fever went away. The next day, which was Easter, brought a whole new set of symptoms. “He couldn’t sit up at all on his own, and his eyes were moving all over the place,” says Danielle. “He also had constant tremors, and he was rocking, like he had no control over his body.”
Their doctor put them in touch with the Department of Neurology at Boston Children’s Hospital. “We got on a Zoom call with the on-call neurologist, Dr. Michael Fayad, and showed him some video of Nathan,” says Danielle. “He told us come in in two hours.”
When the family arrived at the hospital, Nathan was admitted and they met Dr. Mark Gorman, director of the Pediatric Neuro-immunology Program, and two other members of his neurology team.
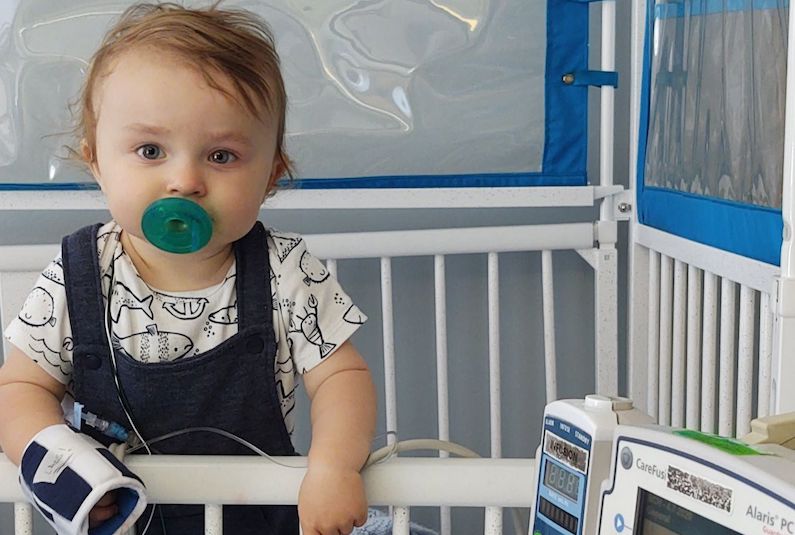
Diagnosis: OMS and an adrenal gland tumor
“Dr. Fayad contacted me as the on-call inpatient neurologist, with the suspicion that Nathan’s symptoms pointed to opsoclonus-myoclonus syndrome (OMS), a very rare — 1 in 5 million children — disorder,” says Dr. Gorman. “I also happen to specialize in OMS, so within 24 hours of Nathan’s admission, we had confirmed the diagnosis, identified the cause was an adrenal gland tumor, and started treatment for the OMS with intravenous immune globulin (IVIG).”
Because it is so rare, diagnosis of OMS can often be delayed for weeks or months, and that delay may be associated with a worse outcome. “It was great to be able to work as a team to diagnose and treat Nathan so quickly, despite the challenges of the pandemic,” he says.
Dr. Gorman and his team connected Nathan’s family with oncologist Dr. Suzanne Shusterman of Dana-Farber/Boston Children’s Cancer and Blood Disorders Center and surgeon Dr. Farokh Demehri to coordinate treatment for his tumor.
While the Asselins were relieved to have a diagnosis for their son, they were frightened to hear he would need surgery to remove the tumor. “It was scary to think that they were going to remove a whole organ from our baby, but Dr. Demehri told us that the best course of treatment was to remove the whole adrenal gland, since he would be fine with one,” says Danielle. “We were discharged from the hospital knowing he would need surgery in a week. It was a little overwhelming, but we knew it had to be done.”

A smooth surgery
The day of the surgery went much easier than they had expected. “Dr. Demehri was able to go in and remove the gland laparoscopically,” says Danielle. “Overall, it was a really great experience and Dr. Demehri was just phenomenal — he’s the reason we were able to get through the experience.”
Nathan was able to go home a few days after surgery, but has been continuing his IVIG treatment for OMS at the Waltham campus every four weeks, along with a steroid. He also underwent a round of immunotherapy treatment with the drug rituximab.
Virtual check-ins
The family has been following up with Nathan’s doctors mainly through virtual visits, though they did see Dr. Gorman for an in-person visit in July. “It’s been great to use Zoom to meet virtually with his doctors, so we don’t have to drive all the way into city,” says Danielle. “We’re happy to continue to meet that way as long as his symptoms are manageable.”
So far, they’ve seen a big improvement in his eyes, and he’s now able to pull himself up, a skill he was just starting before he got sick. “His coordination was the first thing that went when he got sick, but now he’s cruising all over the place and eating on his own with a fork,” says Danielle. “It’s exciting to see him making his own decisions.” Physical therapy sessions at the Waltham campus with Heather Molind have also been helping Nathan regain his skills and track his progress.

However, they will be keeping a close eye on him over the next two years, and if any of his symptoms come back, such as “dancing” eyes or balance issues, they understand he may need to have more treatment.
“So far, he’s right on track, and we’re keeping in close contact with Dr. Gorman and his other doctors to make sure we keep him on track,” says Danielle. “We are so thankful for Dr. Gorman and Nathan’s infusion team. They have really helped make all the rough moments and hard conversations much easier.”
Learn more about the Pediatric Neuro-immunology Program and the Dana-Farber/Boston Children’s Cancer and Blood Disorders Center.
Related Posts :
-

Ellery’s story: The mystery of opsoclonus myoclonus syndrome
Ellery was a normally developing 2-year-old when her skills took a dramatic shift backwards last winter. “She started wobbling when ...
-

Mapping ‘neighborhoods’ in aggressive childhood brain tumors
The third-most common kind of childhood brain tumor, supratentorial ependymoma, is an aggressive cancer that often returns after surgery and ...
-

A true hero’s journey: How a team approach helped Wolfie overcome pancreatitis
Wolfgang, affectionately known as “Wolfie,” is a bright and energetic 7-year-old with a quick wit and a love for making ...
-

A toast to BRD4: How acidity changes the immune response
It started with wine. Or more precisely, a conversation about it. "My colleagues and I were talking about how some ...





