Maya is moving ahead after thyroid cancer
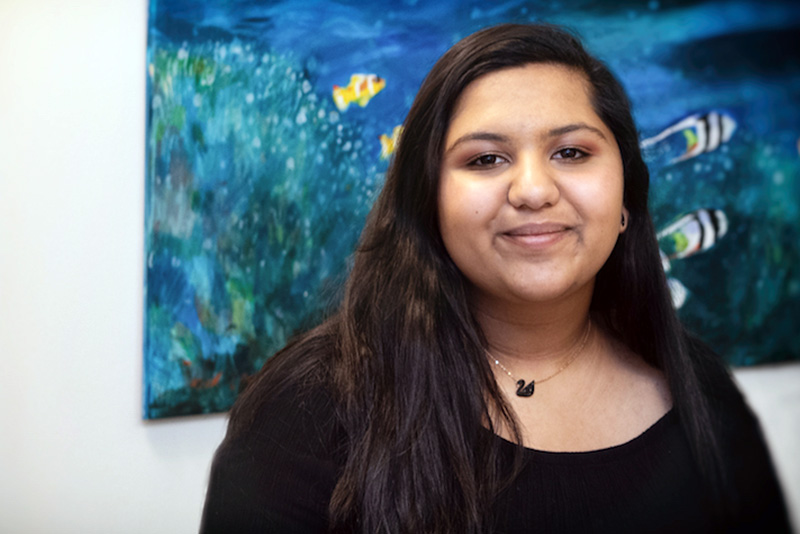
For Maya Rao, 15, a playful accident last Thanksgiving led to the discovery of thyroid cancer. As she and her older sister, Deepti, fooled around, happy to be reunited for the holiday, Deepti’s long hair — gathered in a bun — softly hit Maya on her neck. It seemed innocuous enough, but then she developed pain and minor swelling in her throat. Thinking she might have strep throat, her parents, Umesh and Pushpa, made an appointment with her pediatrician.
After a strep test came back clear, Maya’s pediatrician decided to check her thyroid gland with a blood test and ultrasound. That evening, the Raos got a phone call from their pediatrician they couldn’t have imagined just a few days earlier.
“She told us that it looked like thyroid cancer and that he had already made an appointment for Maya at Boston Children’s Hospital,” says Umesh. In that moment, numb with the shock of the possible diagnosis, he didn’t think to ask why Maya’s doctor had recommended the hospital. “I’m an engineer,” he explains. “I just started executing what we needed to do.”

‘Dad, it’s fine’
The reason for the referral became clear almost as soon as the family arrived at Boston Children’s Thyroid Center from their home in New Hampshire. There, Dr. Biren Modi, one of the center’s co-directors, greeted the Raos — and then asked to speak directly with Maya. He explained that thyroid cancer is highly treatable and has a high survival rate. “He made everything easy to understand and was very reassuring,” remembers Umesh. “We all felt so comfortable with him.”
When an ultrasound and fine needle aspiration confirmed the diagnosis, surgery was scheduled for late January. Surgery for thyroid cancer typically involves the entire thyroid gland, along with any affected lymph nodes in the neck. Maya took it in stride: “She said, ‘Dad, it’s fine. Nothing’s going to happen to me,’” says Umesh.
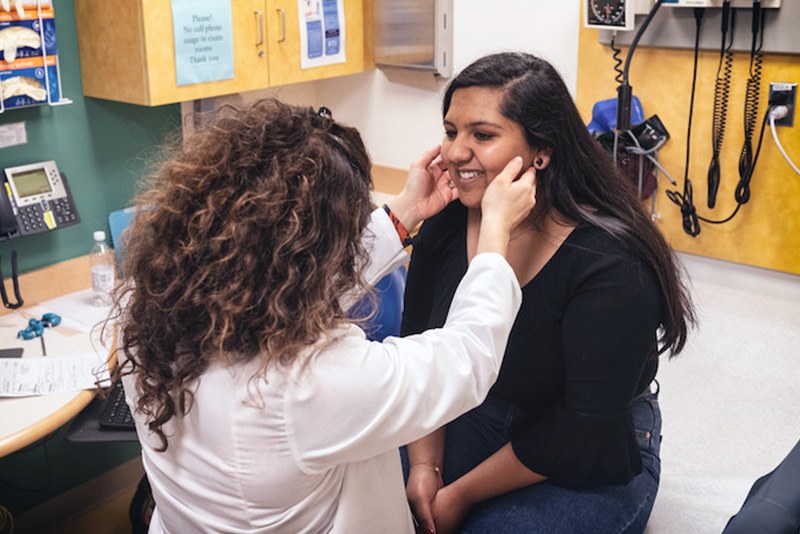
Surgery for thyroid cancer
After the 12-hour procedure, Dr. Modi greeted Umesh and Pushpa with a handful of Hershey’s kisses. “He said, ‘I don’t know about you guys, but I could definitely use one,’” remembers Umesh. But Maya wasn’t out of the woods yet. Although Dr. Modi was able remove all of her thyroid and most of the affected lymph nodes, the cancer was too attached to Maya’s trachea to fully eliminate. Worse, he worried that her vocal cords had been compromised, as the tumor was completely encasing the delicate nerve which controlled their function.
While Maya recovered in the intensive care unit (ICU) that night, the staff also tended to her parents, getting them settled so they could stay with their daughter. Early the next morning, Dr. Modi was back, ready to keep fighting for Maya. “He was very transparent with us and explained everything to us in a really professional but down-to-earth way,” says Umesh. “He has kids too, and that made our experience so much more personal and meaningful.”

A phenomenal recovery
Fortunately, follow-up studies to evaluate her vocal cords show continued improvement, and Maya’s recovery since then has been “phenomenal,” say her parents. Umesh recalls a classic example of the teen’s laidback attitude: His colleagues finally convinced him to leave her bedside and have a pizza in the family room at the ICU. “I had hardly taken my first bite when Maya called me and whispered, ‘Dad, come here right now,’” he says. After rushing back to his daughter’s side, he found her out for a stroll with a nurse. “She was up and walking around for the first time after surgery and wanted me to see it,” he laughs.
Now a high school freshman, Maya continues to impress her parents with her maturity and toughness. She’s taking all honors classes, but also enjoys hanging out with her friends and rowing on her school’s team. “She’s a really happy kid,” says Umesh. “Everything is looking up.”
Learn about the Thyroid Center.
Related Posts :
-

Mapping ‘neighborhoods’ in aggressive childhood brain tumors
The third-most common kind of childhood brain tumor, supratentorial ependymoma, is an aggressive cancer that often returns after surgery and ...
-

How a meniscal transplant made me a Boston sports fan
I was in kindergarten when my knee started popping and cracking. My parents and I didn’t know it at ...
-

Hard and beautiful at the same time: Five lessons of raising a medically complex child
When they learned they were expecting a baby, Michelle and Stephen Strickland were delighted. The South Carolina couple looked forward ...
-

‘Challenge accepted’: Sophia takes on a brain tumor
In 2023, Sophia Mordini landed the role of a lifetime. A competitive dancer, the 12-year-old would play Clara in her company’...





