Amazing Grace: Toddler receives life-changing care for cloacal anomaly
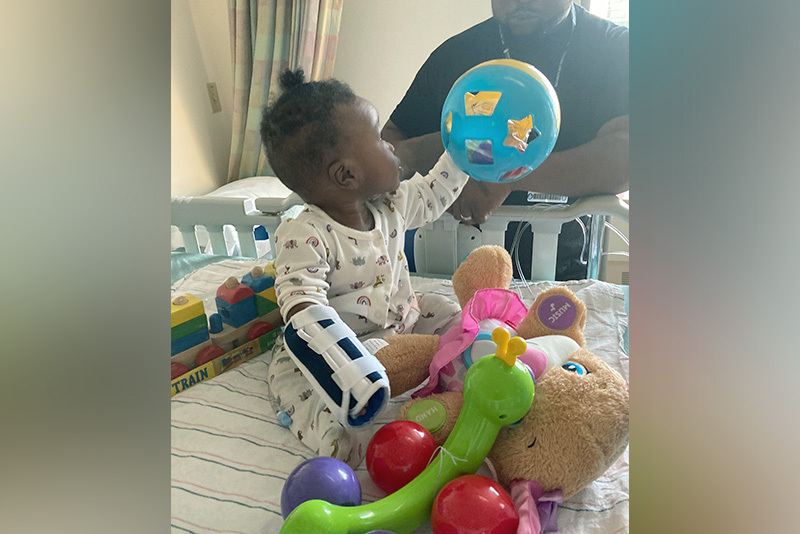
Grace Brown loves playing with her six brothers and sisters, watching educational TV shows, and just being an average toddler. But by some accounts, she shouldn’t be here at all. “We were told before she was even born that she wasn’t likely to survive,” says her mother, K’Shayla.
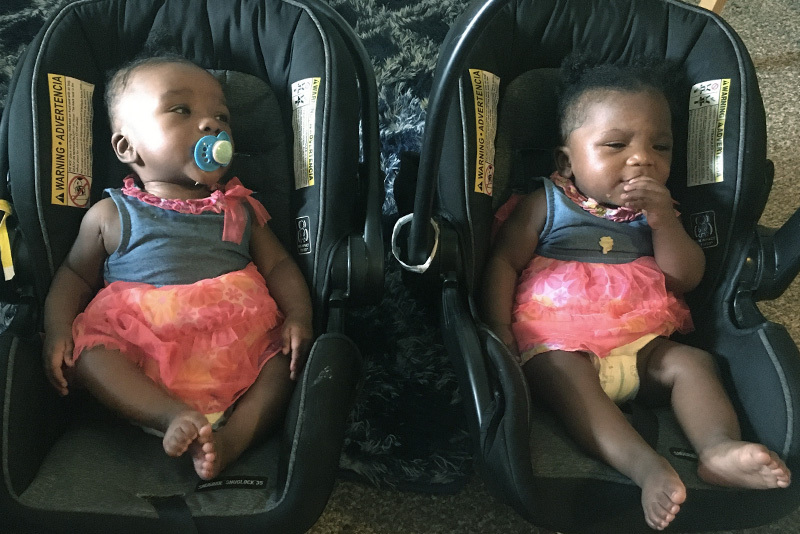
After Grace — and her twin sister, Mercy — were born prematurely at just 29 weeks, her condition became even more concerning. Although Mercy was healthy, Grace had a number of challenges: Among other problems, she had hydrops fetalis (a condition in which large amounts of fluid build up in a baby’s tissues and organs), hydronephrosis (a condition where urine backs up into the kidneys), and her chest wasn’t developing properly. She also had a cloacal anomaly, a type of anorectal malformation in which the rectum, vagina and urologic structures join into one common channel.
“She was so fragile that she stopped breathing and had to be resuscitated,” remembers K’Shayla. “She needed to be intubated and placed on oxygen.”
A life-changing decision
After about three months, the team at Grace’s local hospital said she could go home. But K’Shayla and her husband, Jonathan, were worried — they could see that Grace needed more care than their hospital could provide, and asked for a second opinion. After speaking with Dr. Belinda Dickie, director the Colorectal and Pelvic Malformation Center, they opted to transfer Grace to Boston Children’s Hospital.
That decision was life changing — and possibly lifesaving, says K’Shayla. “Before, we honestly didn’t know if Grace would make it. To find out that there’s a surgeon who specializes in cloacal anomalies — and that this condition isn’t rare to her at all — was a blessing. We learned that there was hope.”
A minimally invasive approach
In Boston, Dr. Dickie and the center’s associate director, Dr. Erin McNamara, used a less-invasive approach to repairing Grace’s cloacal anomaly. Known as a laparoscopic approach to rectal mobilization and urogenital separation, it requires smaller incisions and has the potential to result in faster recoveries, shorter hospital stays, and less pain medication.
The procedure repaired the anomaly — but it also uncovered something unexpected: a growth that turned out to be cancerous. Fortunately, Dr. Dickie was able to remove it and Grace is now cancer free. “She really found the growth by chance,” says K’Shayla. “We’re so grateful she caught it.
Finding hope
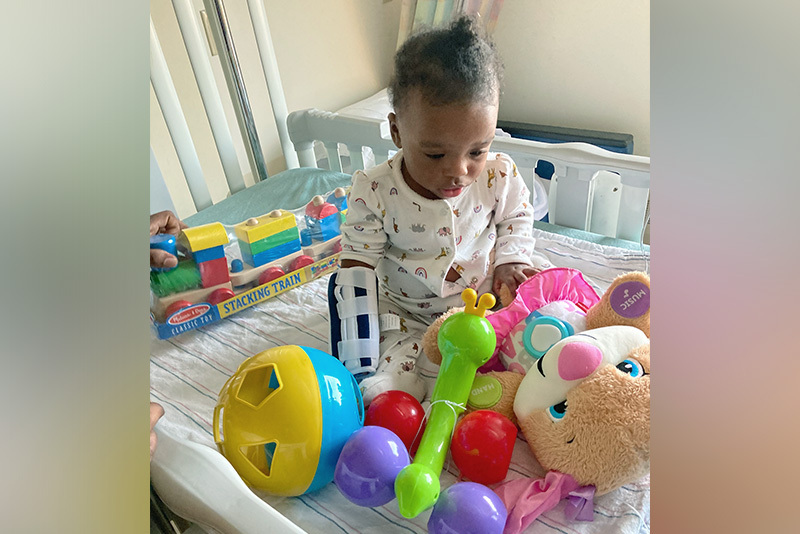
Today, Grace is “doing amazing,” says her mom. She turns 2 in September and is walking, pooping — a big milestone for kids with cloacal anomalies — and ready to start daycare. She returns to see Dr. Dickie and the team for occasional follow-ups.
While she might seem like a typical kid, her family understands that she’s anything but — and they want other families to know there’s hope, too. “Always ask for a second opinion, have faith, and listen to your gut,” says K’Shayla. “Go to the place that gives you hope.”
Learn more about the Colorectal and Pelvic Malformation Center or make an appointment.
Related Posts :
-

Laparoscopic approach to cloacal malformation repair found safe in eligible patients
A minimally invasive surgical approach called laparoscopic rectal mobilization and urogenital separation appears to be a safe alternative to open ...
-

Answers for Aubree: Finding support for OEIS
Michelle and Stephen Strickland are used to having questions about their infant daughter, Aubree’s, health. After all, Aubree was ...
-

Staff Spotlight: Meet Paula Cruz
Paula Cruz is a registered nurse in the Colorectal and Pelvic Malformation Center at Boston Children’s Hospital. The center ...
-

'Finally in the right place': Peyton’s journey to Boston
When Peyton Miklas comes to Boston Children’s Hospital for an appointment, she isn’t just seeing Dr. Belinda ...