Enjoying life, finally free of seizures

Kristen Grip stood in the middle of the basketball court, motionless. Around her, the action continued as usual — the smack of the ball on the polished wood floor, the rush of her teammates as they darted back and forth, the satisfying swish and shout of victory as someone made a basket. Yet the high school freshman stared vacantly into space, her only movement a small tap of her fingers together.
Later, after the coach had blown a whistle and halted the game, Kristen learned that it had happened again: she’d had another seizure. Embarrassed and frustrated, she bid her friends farewell and headed to the school nurse’s office, where she would sleep off the exhaustion until her parents arrived to bring her home.
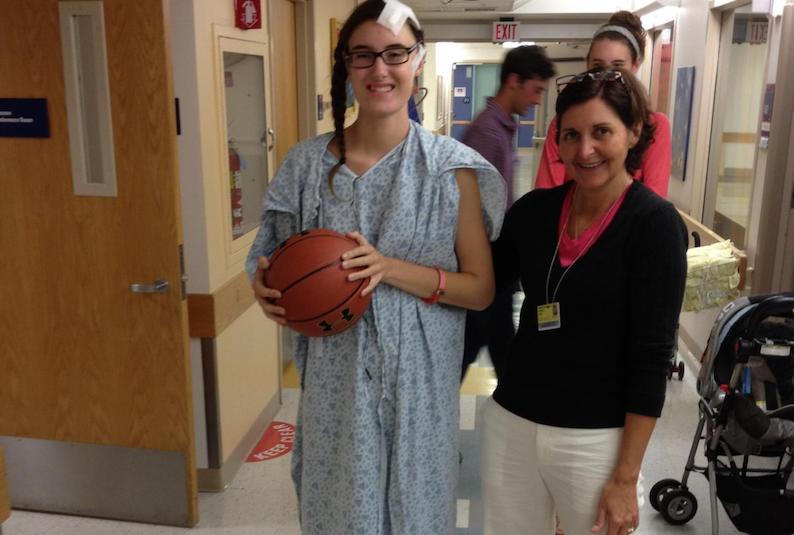
Feeling like a zombie
A year earlier, Kristen had been diagnosed with complex partial seizures (now called focal dyscognitive seizures). This type of seizure, which can last between 30 seconds and 3 minutes, can cause people to abruptly stop what they are doing, stare blankly, and lose awareness of their surroundings. They may also perform involuntary actions, such as moving their mouths, rubbing their hands or blinking their eyes, and may be tired and unable to remember the seizure afterward.
Although Kristen had been prescribed medication, it made her feel both cranky and “like a zombie,” she remembers. Worse, she was still experiencing between eight and 12 seizures a month, often during school or basketball practice. “I just wasn’t able to live life like everyone else,” she says. This was particularly obvious to her because she and her twin sister were taking many of the same classes and doing the same activities, and this was the first time she could not keep up.

Taking a chance
That began to change when Kristen’s physician in the Epilepsy Center at Boston Children’s Hospital, Dr. Annapurna Poduri, raised the topic of surgery at the end of their first consultation. A procedure called a focal resection can reduce and sometimes eliminate seizures in patients who haven’t responded well to medication or other approaches. “Dr. Poduri has always been willing to take chances and try different approaches to help me,” says Kristen.
To many adults — let alone a teenager — the concept of brain surgery is frightening. But Kristen forged ahead. “I definitely wanted to have the surgery. At first, my family was surprised, but we all knew this was my best option,” she says. “My parents and my three siblings were very supportive of me.”

Like night and day
Epilepsy surgery is typically preceded by intensive inpatient testing to determine the part of the brain where seizures are originating and how close that region is to important functions, such as speech and memory. Based on the findings, Dr. Poduri and Kristen’s neurosurgeon, Dr. Joseph Madsen, with input from a multidisciplinary team dedicated to epilepsy surgery, agreed that it would be best that she remain awake during the procedure. This approach allows clinicians to more accurately remove the section of tissue responsible for the seizures without damaging function in the surrounding area. “My mom found the idea of that pretty upsetting,” says Kristen. “But I thought, ‘If I have to do this, I’m going to do everything I can to make it work.’”
That commitment has paid off. Now a senior in college, Kristen has been seizure-free for five years. “I’ve been able to maintain a 3.0 academic average and enjoy playing sports again,” she says. “It’s unreal how different my life is now.”
A dedicated volunteer with several organizations, she plans to do a year of service after she graduates, and wants others to understand the value of putting their health first. “I would tell kids to not be afraid to take a chance. Even if the testing or treatment seems scary, think about your goals,” she says. “I wouldn’t be on this path of wanting to help other people if I hadn’t gone through what I did. Every seizure-free day is a good day.”
Learn more about the Epilepsy Center.
Related Posts :
-

Small gains with big meaning: Loic’s story of deep brain stimulation for PKAN care
Loic, 5, lives in Montana with his parents, Sherine and Mark, and his sister, Selah. He loves Spider-Man, sushi, and the ...
-

Mapping ‘neighborhoods’ in aggressive childhood brain tumors
The third-most common kind of childhood brain tumor, supratentorial ependymoma, is an aggressive cancer that often returns after surgery and ...
-

The dopamine reset: Restoring what’s missing in AADC deficiency
In March 2023, a young girl came to Boston Children’s Hospital unable to hold up her head — one striking symptom ...
-

“Princess June” reigns supreme over Rasmussen syndrome
What do you call a “girly” 5-year-old who adores dolls and frilly nightgowns? If you’re one of June Pelletier’...





