First-ever drug trial reverses some signs of aging in progeria
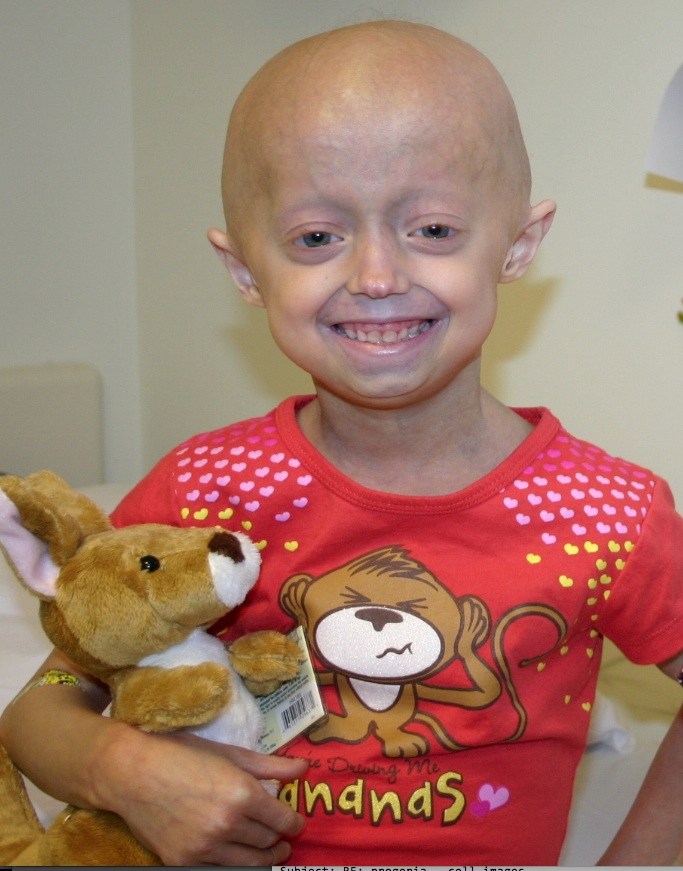
The children came from all over the world: 28 families from 16 countries, speaking over a dozen languages. They faced a grim prognosis: death at an average age of 13 from cardiovascular disease. Not the congenital heart defects we so commonly see in babies coming to Boston Children’s Hospital, but the kind of disease you might find in an 80-year-old: atherosclerosis, heart attacks, strokes.
The children represented three-quarters of the then-known world population with Hutchinson-Gilford Progeria Syndrome, or progeria—a rare, fatal genetic condition in which children seem to age prematurely. When they began arriving at the Clinical Translational Study Unit at Boston Children’s in 2007, most had already lost body fat and hair, had the thin, tight skin typical of elderly people, and were suffering from hearing loss, osteoporosis, hardening of the arteries, stiff joints and failure to grow.
They came every four months, two flying in per week on the dime of the Progeria Research Foundation (PRF). All received lonafarnib, a drug originally tested as a treatment for malignant brain tumors. And the results, announced this week in the Proceedings of the National Academy of Sciences, so far look good.
After two years of treatment, 1 in 3 children had greater than a 50 percent increase in annual weight gain, or had stopped losing weight and started gaining. More than a third had less blood vessel stiffness, a risk factor for strokes and heart attacks. And many had improved bone density and flexibility and better hearing.
Amazingly, it was just in 2003 that the gene that’s mutated in progeria was first discovered, by a team led by Francis Collins, MD, PhD, now director of the National Institutes of Health.
“Within a relatively short time frame, we went from having no idea what caused this disease just 10 years ago to finding the genetic cause and developing a treatment that demonstrates benefit in a clinical trial,” says Collins. “This rate of progress is remarkable and inspires hope that treatments for other rare diseases may also be possible.”
Repurposing a failed cancer drug
The gene discovery quickly led to a better understanding of the disease: In 2004, Collins and colleagues showed that the mutation, affecting a protein called lamin A, causes the cell nucleus to distort. Instead of its normal round shape, it resembled a bunch of grapes—apparently causing the cell to “age” before its time. Then in 2005, Collins’s team reversed this effect by preventing a molecule called a farnesyl group from attaching to the mutated lamin A.
“They found that if you use lonafarnib, suddenly cells become normal looking,” says Mark Kieran, MD, PhD, director of pediatric medical neuro-oncology at the Dana-Farber/Children’s Hospital Cancer Center, principal investigator on the progeria clinical trial at Boston Children’s.
As it happened, Kieran had been testing lonafarnib in children with malignant brain tumors. Since lonafarnib prevents farnesyl groups from being added onto other molecules, it seemed like a promising cancer treatment, since the addition of a farnesyl group activates the cancer-causing Ras oncogene.
Unfortunately, lonafarnib failed as a cancer treatment, but Kieran gained experience with using it in children. So when the Progeria Research Foundation learned of Collins’s discoveries and decided to run a clinical trial of the lonafarnib for progeria, Kieran was chosen to lead it.
Collins’s lab continues to study the molecular genetics of progeria to learn more about how the disease works. About a year ago, the lab showed that another drug, rapamycin, causes the abnormal, farnesylated lamin A molecule to be destroyed outright in progeria cells—reversing the same cell defects as lonafarnib, but through different means.
Kieran and colleagues have nearly completed a triple-drug trial—lonafarnib plus two other drugs used for diseases of old age: the cholesterol-lowering drug pravastatin and zoledronic acid, used in osteoporosis. Now Kieran hopes to launch a third trial adding a drug closely related to rapamycin.
Progeria and us
Meanwhile, Collins and others have found evidence that while progeria is exceedingly rare—striking an estimated 1 in 4 million children, or perhaps 100 in the world—it may have lessons for aging in general.
For example, research has shown that the mutant lamin A interferes with cell division, that it may cause the chromosomes to be disorganized, and that it may both enhance and be exacerbated by damage to telomeres (the tips of chromosomes)—all factors known to cause cellular aging.
“Looking in older and older normal people, one of the things we see is that the amount of this abnormal lamin A goes up in your body,” adds Kieran. “It’s almost like one of the clocks in the body that tells cells you’re getting older.”
Some lamin A mutations might even be beneficial: A meta-analysis published this year looked at genetic variants of lamin A across large populations, including centenarians, and found one to be significantly associated with longevity.
Related Posts :
-

A case for Kennedy — and for rapid genomic testing in every NICU
Kennedy was born in August 2025 after what her parents, John and Diana, describe as an uneventful pregnancy. Soon after delivery, ...
-

The journey to a treatment for hereditary spastic paraplegia
In 2016, Darius Ebrahimi-Fakhari, MD, PhD, then a neurology fellow at Boston Children’s Hospital, met two little girls with spasticity ...
-

Thanks to Carter and his family, people are talking about spastic paraplegia
Nine-year-old Carter may be the most devoted — and popular — sports fan in his Connecticut town. “He loves all sports,” ...
-

Genomic sequencing transforms a life: Asa’s story
Asa Cibelli feels like he’s been reborn. The straight-A middle schooler plays basketball and football, does jiu jitsu, is ...





