Healing hearts under a watchful eye

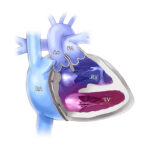
Cardiac surgery is performed using visual landmarks inside the heart. There are specialized conduction tissues that run underneath the surface, which are important for the heart’s rhythmic beating. Cardiac surgeons operate with these landmarks in mind to avoid injury to conduction tissue, but locating these tissues can be challenging.
Fiberoptic confocal microscopy technology inside the heart
One of the potential complications of cardiac surgery is injury to the cardiac conduction tissue, which can result in conduction abnormalities that necessitates pacemaker placement. AK Kaza, MD, a pediatric cardiac surgeon and director of the Neonatal Cardiac Surgery Program at Boston Children’s Hospital, describes the reality of this outcome for a child, “It means a lifetime of pacemaker and cardiac lead change outs, potential for infection, which can ultimately impact life expectancy and exercise tolerance.”
Twelve years ago, Kaza was asked to assist a colleague investigating gap junctions, myocytes, and novel imaging technologies for identifying these structures. The collaboration inspired Kaza. He hypothesized that using fiberoptic confocal microscopy to directly visualize conduction tissue during cardiac surgery could reduce the risk for injury to these pathways.
Over the next decade, Kaza and his colleagues studied fiberoptic confocal microscopy in mouse, sheep, and human tissue, refining the technology for use intraoperatively. He explains, “It’s about a millimeter or so in diameter and can be used inside the heart to see where the conduction tissues are,” he says. Ultimately, Kaza concluded this imaging modality could, indeed, become a crucial adjunct in cardiac surgery.
From the lab to the operating room
Transitioning from the laboratory to a clinical setting mandates rigorous compliance with regulatory and federal institutional guidelines.
“Obviously, the bottom line is patient safety,” says Kaza. “We want to do this, but we want to do this with the objective that we can improve on the status quo.”
Kaza looked to the Institutional Centers for Clinical and Translational Research (ICCTR) for help. “For a busy clinician like me to understand the nuances of all these regulatory affairs takes several hundred hours,” he says. Cindy Williams, DNP, RN, PNP, NE-BC, co-director of the ICCTR Experimental Therapeutics and Interventional Trials Center (ET/IT), organized a team to assist Kaza, ensuring his imaging technology was implemented safely.
The collaboration proved to be invaluable for Kaza. With ICCTR on board, he received FDA and institutional approval to initiate the pilot study. Promising results from this study allowed Kaza and his research team to move on to the next phase of the grant — a randomized clinical trial comparing complication rates for children undergoing cardiac surgery, with and without the aid of fiberoptic confocal microscopy as a guide.
Reflecting on his experience, Kaza says, “Within a few months of working with ICCTR, we were able to surmount a lot of hurdles; hopefully, in about five years or so, this technology will be used widely.”
Learn more about the Department of Cardiac Surgery.
Related Posts :
-

Biventricular repair linked to better outcomes in superior-inferior ventricles treatment
The complexity of superior-inferior ventricles — a condition in which one ventricle is positioned on top of the other — has often ...
-

A reunion of the heart: Grace and Amy bond through HLHS
At first glance, Grace and Amy have a pretty typical friendship: they joke around, cheer each other on, and keep ...
-

First-of-its-kind pressurization test could improve Ross procedure outcomes
The Ross procedure is a preferred surgery to treat severe aortic valve disease. The procedure replaces the failing valve ...
-

Promising advances in fetal therapy for vein of Galen malformation
In 2024, Megan Ingram* of California and her husband were preparing for the birth of their third child when a 34-week ...