Predicting feeding difficulties in children with esophageal atresia: A proactive approach
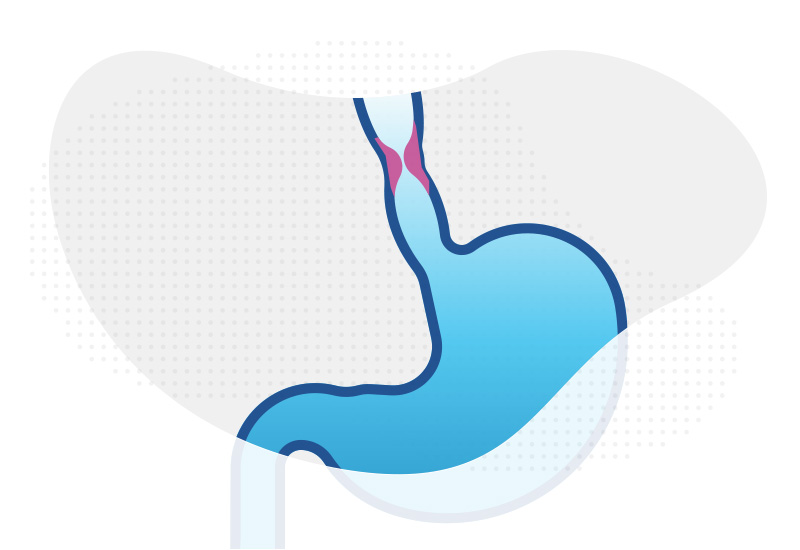
Children with esophageal atresia are at risk for developing anastomotic strictures, or areas of esophageal narrowing, following surgical repair. Clinicians have long assumed that such strictures can cause dysphagia and feeding difficulties, but it isn’t clear whether the severity of feeding difficulties is related to the severity of a stricture.
Now, findings of a recent study from Boston Children’s Esophageal and Airway Treatment (EAT) Center may prompt a paradigm shift in this thinking — and could someday offer gastroenterologists and others a clear guide for predicting feeding challenges in children with esophageal atresia.
Study finds clear relationship
According to guidelines released in 2016, there is no clear link between the severity of anastomotic narrowing and severity of feeding difficulties. However, the evidence supporting this statement was limited to expert opinion. “Our experience in the EAT Center is a bit different,” explains gastroenterologist Jessica Yasuda, MD. “We’ve observed that children with more severe feeding challenges also tend to have more severe strictures.”
To learn more, Yasuda and her colleagues analyzed data from 330 children with repaired esophageal atresia who had been seen in the EAT Center between 2019 and 2021. Of these children, 97 partially or fully depended on feeding tubes. The team found that anastomotic strictures were the only potentially modifiable risk factor for feeding tube dependence in these children — even after adjusting for factors such as nutritional status, age, and comorbidities. What’s more, the severity of a stricture was significantly associated with feeding tube use.
The study, published September 5, 2022, in Diseases of the Esophagus, is the largest of its kind to systematically explore this relationship.
Takeaways for your practice
While more research is needed to confirm these findings, they have potential critical implications for the management of pediatric esophageal strictures. Currently, many centers don’t treat strictures until they become symptomatic, which could lead to delays in addressing feeding difficulties.
“Our approach at Boston Children’s — especially for long-gap or complex surgical patients at high risk for stricture — is proactive rather than reactive,” explains Yasuda. The EAT Center team recommends the following.
- Children at high risk for strictures: evaluate with endoscopy one month after surgical repair for esophageal atresia to begin dilations for developing strictures
- Children at low risk for strictures and without symptoms: Assess with esophagram within three to six months of repair to ensure severe strictures aren’t developing
“We’ve found this tactic helpful in assessing strictures, rather than taking a one-size-fits-all approach of waiting for symptoms of feeding difficulties to emerge,” says Yasuda.
Learn more about the Esophageal and Airway Treatment Center or refer a patient.
Related Posts :
-

Beyond limits: A staged approach to jejunal interposition
By the time Chase Essex arrived at Boston Children’s Hospital in 2016, he had reached what most clinicians would consider ...
-

At the intersection of research and clinical care: Celebrating our female gastroenterologists
In honor of Women’s History Month and National Doctor’s Day, we’re celebrating just a few of the ...
-

Game-changing surgical procedure results in zero-percent TEF re-recurrence rate
A tracheaesophageal fistula (TEF) is a congenital defect in which an abnormal connection forms between a child’s esophagus and ...
-

Taking treatment of long-gap esophageal atresia to the next level: Refining innovative techniques
The surgeons in the Esophageal and Airway Treatment Center at Boston Children’s Hospital are pioneers in developing and refining ...