We didn’t give up hope: Emily’s fighting chance with her lung transplant

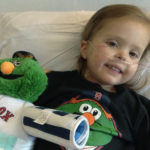
Emily lights up every room she’s in with her giggles and confidence — not to mention her sparkly painted nails and glittery makeup. At 6 years old, she’s able to win people over with her bright smile and electric personality.
All this is made possible because Emily was given the gift of life — an organ donation in what seemed to be impossible circumstances. “It was during one family’s darkest hour that Emily was given the ability to continue to live,” shares Stephanie, Emily’s mom.
Faced with challenges from the start
When she was born, Emily was diagnosed with pulmonary hypertension, abnormally high blood pressure in the arteries of the lungs. As a result, her lungs were not strengthening, so she remained in her local NICU in Maine for eight weeks. “She came home on oxygen, and she was stable for the first two years of her life,” explains Stephanie.
In February 2019, when Emily was 2, she appeared to be healthy, growing stronger, and no longer needed oxygen. But just a month later, she came down with a cold and was admitted back into the hospital. “We didn’t think we’d be there long, but her lungs kept getting worse,” shares Stephanie. Emily was intubated after a couple of days, and her doctors realized she needed more care than what they could offer.
Emily was quickly transferred to Boston Children’s Extracorporeal Membrane Oxygenation (ECMO) Program for treatment using advanced technology that functions as a replacement for a critically ill child’s heart and lungs. “We didn’t think she’d need to be on ECMO, but her lungs just failed.” For two weeks, there was no improvement in Emily’s lung function — she was only getting worse.
Finding strength in the darkest hours
A lung biopsy came back showing that Emily had interstitial lung disease, a group of rare lung diseases that range from mild to severe that make it difficult to breathe. “We still don’t know if it was genetic or just damage from her previous diagnoses,” explains Stephanie. “But we knew that her lungs were not going to be able to recover on their own — we truly thought we were going to lose her.”
It was an ECMO specialist, named Mark Brown, at Boston Children’s that stepped in and gave Stephanie and her family hope. “He looked at us and said, ‘We haven’t even begun to fight. Boston Children’s doesn’t give up hope.’” Very quickly, Emily met with Boston Children’s Pediatric Transplant Center to learn if she was a candidate for a lung transplant.
Stephanie shares that Dr. Francis Fynn-Thompson saved Emily’s life by innovating a surgery to get her on the list. “Dr. Fynn-Thompson designed a surgery with cannulas that were able to make Emily a candidate for surgery — and she was quickly listed as a candidate shortly after.”
About the procedure, Dr. Fynn-Thomspon shares, “Given that she would have an unknown duration of wait time for the donor organs, I decided to use Berlin Heart ventricular assist device cannulas to cannulate her centrally to veno-venous (VV) ECMO. This allowed her to be extubated and rehabilitated while waiting for her transplant. Before this point, we had not taken this approach and cannulation strategy with a patient waiting for lungs.”
Hope was never lost
This is where Emily’s hero — her organ donor — enters their story. Her hero was only 22 months old when she became Emily’s second chance. Just 36 hours after being listed as a candidate for an organ transplant, Emily matched and was able to receive a lung transplant — a miracle turnaround time. It was a successful procedure, and Emily hasn’t experienced any signs of transplant failure in the four years since her surgery.
“Boston Children’s doesn’t stop fighting for your family until you tell them you’re done. Emily was very sick, but they did everything possible to save her life,” shares Stephanie. “As of now, we’ve been given four extra years with Emily, years we didn’t think possible, thanks to her donor and the team at Boston Children’s.”
To find out how to become an organ donor, register here. Visit the Pediatric Transplant Center.
Related Posts :
-

A true heart of gold: Jeremiahs' heart transplant journey
With sirens wailing, Angelie and her husband sped through traffic, anxious to get to the city in time. The police ...
-

After a marathon year, let’s make organ donation part of our new normal
Six years ago, an organ donor saved my daughter’s life. Cora was born with a congenital heart defect called ...
-

From Virginia to Boston for a kidney transplant: Joshy’s story
Joshy Buchheit is a lot like most 4-year-old boys. He loves playing in the mud, riding his scooter, and keeping ...
-

Looking for clues to improve the life of a transplanted organ
The Transplant Research Program (TxRP) at Boston Children’s Hospital is the only pediatric transplantation research program in the U....