From Virginia to Boston for a kidney transplant: Joshy’s story

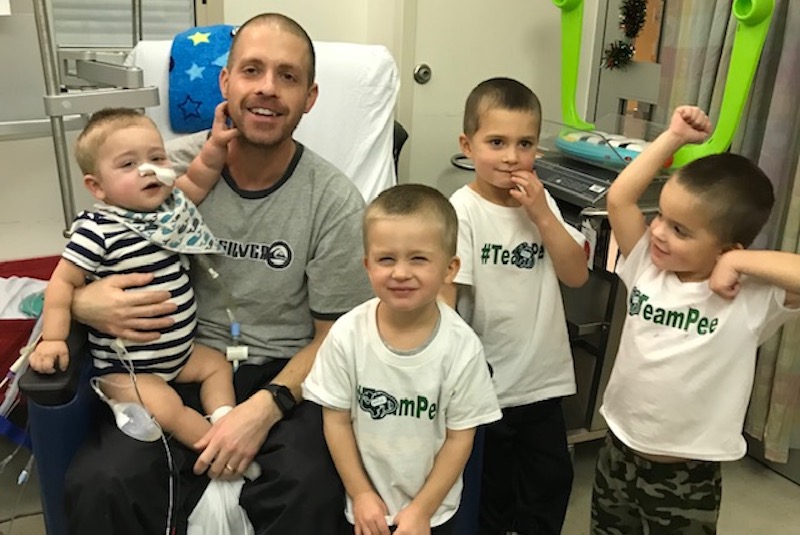
Joshy Buchheit is a lot like most 4-year-old boys. He loves playing in the mud, riding his scooter, and keeping up with his three older brothers, Joseph, Ethan, and Evan. But what sets Joshy apart is that he was born with end-stage renal disease (ESRD) and had a kidney transplant when he was just 20 months old.
Joshy’s transplant journey began before he was born. His parents, Jen and Ryan, learned at Jen’s 17-week ultrasound that he has a condition called hydronephrosis, a swelling of the kidneys caused by posterior urethral valves.
“At first, my local doctors in Virginia weren’t too concerned, and then I had a follow-up ultrasound and we learned that he had very little amniotic fluid surrounding him,” says Jen. “The doctors still didn’t seem too concerned, but it was concerning to us. Ryan has very good intuition and he thought we should get a second opinion, so we did.”
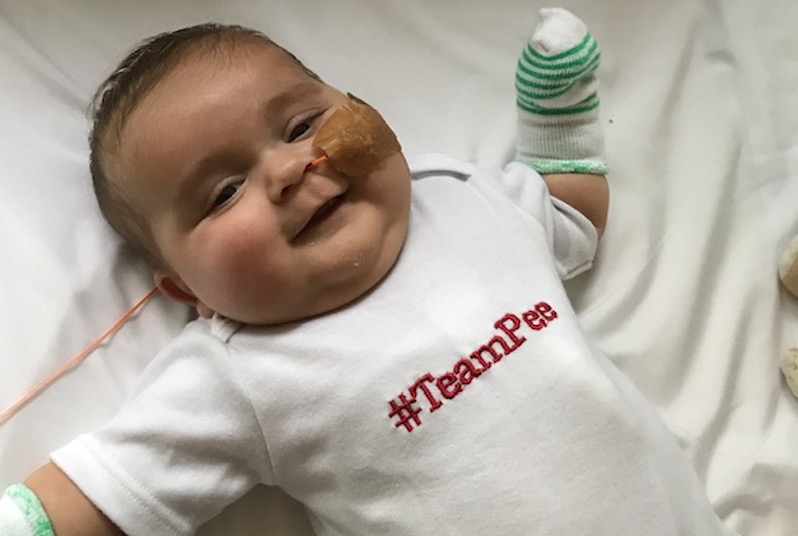
A second opinion for hydronephrosis in Boston
After looking at several pediatric hospitals online, they reached out to the Maternal Fetal Care Center (MFCC) at Boston Children’s. “Ryan called and spoke with Lauren Farqui from the MFCC and she was so kind and helpful,” says Jen. “She put us at ease.”
The couple decided to travel to from Virginia to Boston in January 2017 for a consult. “Lauren helped us schedule appointments for extensive rounds of ultrasounds and booked appointments with a pediatric nephrologist, Dr. Deborah Stein, and a pediatric urologist, Dr. Michael Kurtz.”
Jen says that was the first time they realized the true severity of Joshy’s situation. “It was the first time anyone had talked to us about end-stage renal disease or dialysis. We decided then that I would need to stay in Boston for the rest of my pregnancy. I knew it would be hard to be separated from Ryan and the boys, but we wanted to give Joshy the best chance possible, and we knew that meant being in Boston.”
Birth, surgery, and dialysis
So while Ryan returned home to their other sons, Jen remained in Boston, anxiously awaiting Joshy’s birth. He was delivered at 37 weeks at Brigham and Women’s Hospital and transferred to Boston Children’s, where he remained in the intensive care unit (ICU) for three months.
“He had his first surgery to clear his post-urethral valve three days after his birth,” says Jen. “And because his lungs weren’t developed, he was on the highest level of breathing support possible, which damaged his lungs.”
Because Joshy’s kidneys weren’t working properly, he had to be placed on peritoneal dialysis one month after his birth. “It was crazy to see this tiny baby hooked up to all of these tubes and machines that are really meant for adults,” says Jen. “And while he needed the dialysis to keep him alive, we knew it was never a permanent solution — ultimately we knew he needed a kidney transplant — but he needed to get stronger and bigger first.”
It was also a difficult time for his family — at the time of dialysis, he had just a 50 percent chance of surviving his first year. But after a few months, and a few back-and-forth visits from Ryan, Jen and Joshy moved back home to Virginia with the rest of the family. Joshy was still on dialysis for 12 hours a day. But overall, he was doing okay, and the family was happy to be back together.

Ready for a kidney transplant
As Joshy got bigger and continued to do well, his doctors in Boston did a complete transplant workup to prepare for an eventual kidney transplant. After much consideration, it was determined that Ryan would be his donor.
“We knew that we would not get his transplant anywhere else but Boston Children’s,” says Jen. “But we also knew our family couldn’t be separated again, so we decided to move our whole family to Boston before the surgery.”
In March 2018, the family moved to Norwood, a suburb of Boston, to get the older boys settled in before school started in the fall. After the move, Joshy spent about 16 weeks inpatient at Boston Children’s for breathing problems, and ultimately needed a tracheotomy to help him breathe.
Finally, one of Joshy’s nephrologists, Dr. Avi Traum, and the transplant team at Boston Children’s decided he was big enough and well enough to undergo the transplant, and it was scheduled for November 2018 with surgeons Heung Bae Kim and Khashayar Vakili.
“I was genuinely excited about the transplant, not emotional,” Jen says. “And I wasn’t worried about Joshy or Ryan. What was crazy is that I felt totally comfortable during the transplant — I knew all of his nurses, doctors, child life therapist, and respiratory therapist by name from previous admissions. So many of them have known Joshy since his birth, so I felt like we had family and friends watching over him.”
After his transplant, Jen and Ryan noticed almost immediate changes in Joshy. “He smelled different and his skin texture changed,” says Jen. “I realized I had never seen his face free of tubes. And once he lost all of the excess fluid, I noticed he had a dimple on his cheek we couldn’t see before.”

Reckoning with the past, looking toward the future
Jen says they also began to reckon with just how sick he had been. “I realized after his transplant that he would have died if we hadn’t brought him to Boston. It also opened our eyes to a world we didn’t know anything about, and the struggles of other children and families who need transplants.”
In 2019, the family moved back to Virginia, on a piece of land large enough for Joshy and his brothers to run around and play freely — and a bedroom large enough to hold all of Joshy’s equipment. He still uses a ventilator for help breathing and a gastronomy tube (G-tube) to give him nutritional support. “Since the transplant he’s developed like crazy,” says Jen. “He started standing up, talking, and sleeping better. He’s also growing taller, and acting like a regular kid.”

Joshy is followed by local nephrologist in Virginia but receives most of his care from the kidney transplant team in Boston, which includes Dr. Traum and his colleagues Dr. Nancy Rodig, Dr. Michael Somers, and Dr. Michael Ferguson, as well as an entire team of clinicians who specialize in the care of children with this condition.
“Everyone on his team is so accessible,” says Jen. “I know I can reach out to his transplant coordinator JoAnn Morey or any of his team members whenever I have a question. And if he needs care, we’re ready to drive him up to Boston at any moment. We would not go anywhere else. They are truly miracle workers.”
Learn more about the Kidney Transplant Program and the ESRD Program.
Related Posts :
-

Can we tip the immune system toward transplant tolerance?
First in a two-part series on transplant tolerance. Read part two. Although organ transplant recipients take drugs to suppress ...
-

Four things to know about your child’s kidneys
If you’re like most parents, you probably know that the kidneys filter waste from the body and produce urine. ...
-

‘We never stopped believing’: Benny’s journey with liver cancer
Earlier this year, 12-year-old Benny helped his dad, Ben, build a deck around his family’s pool. Moving boards, handing ...
-

‘A football game changed my life’: Jamison’s non-directed kidney donation
When recess is your favorite school subject, and you’re so naturally funny that the adults in your life belly ...





