Two neuroscience rock stars elected to the National Academy of Medicine

Beth Stevens, PhD, and Elizabeth Engle, MD, are the latest Boston Children’s Hospital researchers to be elected to the prestigious National Academy of Medicine. Their election, together with Daphne Haas-Kogan, MD, brings Boston Children’s total number of current NAM members to 22. Both scientists hail from the F.M. Kirby Neurobiology Center at Boston Children’s and are on the faculty of Harvard Medical School.
Membership in the NAM, formerly the Institute of Medicine, is considered one of the highest honors in the fields of health and medicine. The NAM serves as an adviser to the nation and the international community. Its members are chosen for their accomplishments and contributions to the advancement of the medical sciences, health care, and public health.
Immune cells in brain wiring
NAM recognized Stevens for her pioneering work on how the brain is wired in early life and how the nervous and immune systems interact in health and in disease. A 2015 MacArthur “genius” grant winner, Stevens has transformed how neuroscientists view the brain’s glial cells. Scientists used to see glia as mere support cells, and frankly didn’t give them much thought.

But Stevens has shown that microglia, which are also part of the immune system, are active players in developing brains. They fine-tune the synapses (connections) between neurons by literally “eating” them, which is why she calls them Pac Man of the brain.
More recent work in the Stevens Lab suggests that microglia may be wrongly activated later in life. This may contribute to synapse loss in diseases like Alzheimer’s and schizophrenia.

“A lot of synaptic loss happens in humans potentially years before you get memory loss or pathology,” Stevens explained in the Harvard Gazette. “If we can figure out a way to protect the synapses, it might slow the progression of the disease.”
The lab is also investigating whether microglial activity is altered in the developing brain in mouse models of autism. That disorder is thought to involve abnormal synapse development.
Eye movement as a window into the brain
Elizabeth Engle’s work is equally amazing. Early in her career, during her neurology residency, she saw a little boy whose eyes were frozen in a downward gaze. She wanted to find a solution to an inherited, socially isolating condition that others had written off. So Engle delved deep into genetic studies of eye-movement disorders, enrolling more than 900 subjects in her studies to date. She has identified a host of genetic mutations causing relatively common disorders like strabismus and more rare, complex disorders also involving symptoms such as facial weakness, deafness, loss of smell, and swallowing problems.

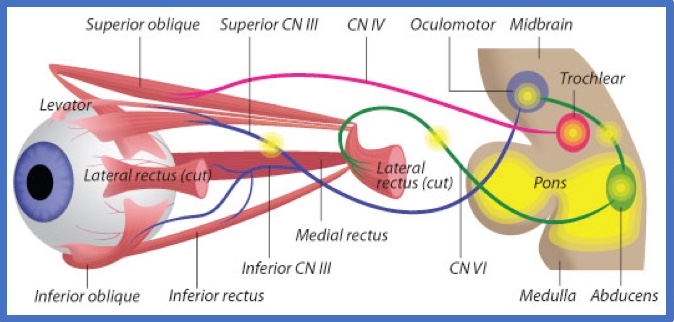
By modeling the genetic defects in zebrafish, mice, and neurons made from patients’ stem cells, Engle has added much new information about the functioning of the cranial nerves that innervate the eye muscles — and the nervous system as a whole.
“We’re the only lab in the world in this niche,” she said recently at a gathering for postdoctoral fellows, adding, “You want to push forward in something you believe in.”
Both Stevens and Engle are also Howard Hughes Medical Institute investigators and members of the Broad Institute of Harvard and MIT.
“We are exceptionally proud to have faculty members as distinguished as Elizabeth Engle and Beth Stevens, whose scientific contributions are truly transformative,” says Clifford Woolf, PhD, director of the F.M. Kirby Neurobiology Center. “It must be the year of neuroscience.”
Learn more about research in the F.M. Kirby Neurobiology Center
Related Posts :
-

Beyond average-based medicine: HIE as a blueprint for data-informed care
Historically, outcome prediction in medicine has followed a familiar formula: run a clinical trial, publish the results, guide care based ...
-

The hidden burden of solitude: How social withdrawal influences the adolescent brain
Adolescence is a period of social reorientation: a shift from a world centered on parents and family to one shaped ...
-

The journey to a treatment for hereditary spastic paraplegia
In 2016, Darius Ebrahimi-Fakhari, MD, PhD, then a neurology fellow at Boston Children’s Hospital, met two little girls with spasticity ...
-

The dopamine reset: Restoring what’s missing in AADC deficiency
In March 2023, a young girl came to Boston Children’s Hospital unable to hold up her head — one striking symptom ...





