Blood donations help Kit manage Diamond-Blackfan anemia — so she can dance, sing, and enjoy life

Every month, Kit Murdoch needs a blood transfusion to stay alive.
The 2-year-old has Diamond-Blackfan anemia, a rare genetic blood disorder that, if untreated, prevents blood from delivering oxygen through the body. While it has been a devastating diagnosis for Kit’s parents, they’re grateful for the specialized care she receives and are constantly amazed that people they will never meet are donating blood for her.
“There’s no substitute for donor blood,” Kit’s mom, Molly, says. “It’s easy to overlook that when you donate blood, you save lives. Donors are literally saving my child’s life. There’s no way around it: This is what Kit needs to be alive.”
A life-changing diagnosis for Kit’s family
When Kit was three months old, she became pale and lethargic and stopped eating. She fortunately had a cardiology appointment at a Boston Children’s satellite center in Weymouth, Mass., close to the family’s home in Bridgewater. (Kit was born with a ventricular septal defect, a hole in the wall that separates the heart’s two ventricles, but it eventually healed on its own.) Evaluating Kit’s new symptoms, the care team was alarmed by an EKG: Her organs were shutting down and she had a dangerously low level of hemoglobin, the critical red blood cell protein that carries oxygen to the body’s tissues.
Soon, Kit and Molly were in an ambulance headed to Boston Children’s main campus. There, Kit was diagnosed with Diamond-Blackfan anemia and received the first of a lifetime of blood transfusions. Steroid therapy that attempted to stimulate bone marrow to produce red blood cells was ineffective, so Kit has to rely on a steady flow of donated blood to keep her hemoglobin at safe levels.
“It was a shocking diagnosis, absolutely life altering,” Molly recalls. “I took a year off from work to wrap my head around it.”
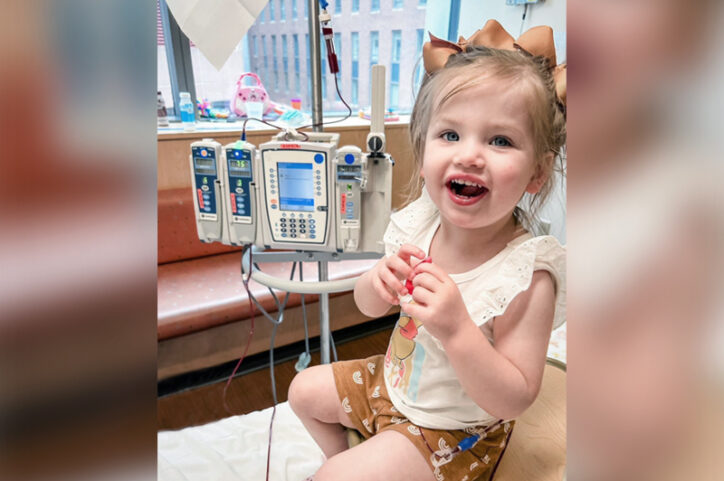
From fear to a birthday party for a medical device
Kit receives transfusions at the Jimmy Fund Clinic through the Dana-Farber/Boston Children’s Cancer and Blood Disorders Center, an integrated pediatric hematology and oncology program. Transfusions were initially difficult for young Kit. “She hated it. She was terrified of the needle,” Molly recalls.
But those fears subsided last year when a quarter-sized port was implanted in her chest, allowing new blood to enter directly into a vein and putting Kit at ease. It’s been such a welcome development that Kit and her family had a birthday party for the port on the one-year anniversary of its implantation. “She knows where her port is and why she has one,” Molly says. “She’s been helping the nurses access and clean it and be part of the process.”
Kit’s care team makes a lasting impression
Consistent blood transfusions can cause side effects, including an unhealthy overload of iron. To ensure Kit — who recently had her 30th transfusion — stays healthy, she undergoes iron chelation therapy overseen by her care team at Boston Children’s Bone Marrow Failure and Myelodysplastic Syndrome Program.
The team includes Dr. Grant Rowe, a blood disorder specialist who Molly says “has been phenomenal.” Nurse practitioner Karyn Brundige has been the family’s “guardian angel” for always having answers any time of day, even on Sundays. Mary Anne Milbert, a Department of Cardiology nurse practitioner, also has a special place in Molly’s heart for slipping a banana and granola bar into Kit’s diaper bag at the Weymouth facility that day, knowing Molly would probably not have a chance to eat once she got to Boston.
Overwhelmed by the generosity of strangers
Boston Children’s Blood Donor Center collects the donated blood that Kit receives. Kit and her family have developed close relationships with the center’s staff, including the blood donor technicians who work at the family’s annual blood drive in their hometown. Molly is grateful that people who the family might never meet readily give their blood to help Kit and others. “It is overwhelming,” Molly says. “We rely on other people, and they’re willing to do it.”

Molly wants those donors to know they help Kit enjoy singing, listening to music, taking dance classes, reading, cuddling, and spending time with her mom; dad, Sam; and 5-year-old sister, Lucy.
“Thank you for allowing my husband and me to focus on Kit’s medical care and be confident there will be blood in the blood bank every month,” Molly says. “Thank you for keeping Kit’s cheeks rosy, her lips pink, and her heart pumping. Thank you for giving Lucy a little sister to grow up with. Most of all, thank you for keeping Kit alive. You are all my heroes, and my family is forever grateful for each and every one of you.”
Make an appointment to donate blood and help children like Kit.
Related Posts :
-

Teaming up to fast track a novel gene therapy for Diamond-Blackfan anemia
Looking at Lindsay Krieg, it’s impossible to tell she has spent her entire 29 years in an out of hospitals ...
-

A potential Diamond-Blackfan anemia treatment swims into view
Zebrafish, besides being popular in aquariums, make good stand-ins for studying human diseases. They share about 70 percent of their genes ...
-

After 80 years, genetic causes of Diamond-Blackfan anemia come into view
In 1938, Louis K. Diamond, MD, and Kenneth Blackfan, MD, at Boston Children’s Hospital described a severe congenital anemia that ...
-

Stem cell workaround cracks open new leads in Diamond Blackfan anemia
Diamond Blackfan anemia (DBA) has long been a disease waiting for a cure. First described in 1938 by Louis K. ...