Radiology of COVID-19 infection in children: Imaging findings and recommendations

· Lung images in children with COVID-19 show unique features, including the halo sign.
· Chest X-ray and CT images differ significantly from early to late infection.
· New imaging guidelines recommend when to perform imaging studies on children with COVID-19.
As more children become infected with the coronavirus causing COVID-19, lung imaging shows that the disease has characteristic imaging findings in the pediatric population. And since the disease is so new, information about the most appropriate use of imaging has been lacking.
In a pair of original peer-reviewed papers, pediatric radiologists from Boston Children’s Hospital and other international pediatric thoracic imaging experts provide some details about what COVID-19 infection looks like in the lungs of children. And they provide a set of practical imaging guidelines for COVID-19 in children.
Five lung disorders compared
In the first paper, the authors compared the characteristic images of five new pediatric lung disorders: COVID-19, SARS, H1N1, MERS, and e-cigarette or vaping product use-associated lung injury (EVALI). They discovered that even though COVID-19 is caused by the same virus in adults and children, images of the lungs of children with the illness show some unique findings that are different from those seen in adults.
Their findings derive from studying COVID-19 imaging studies from other researchers as well as several cases treated at Boston Children’s and other co-authors’ hospitals around the world. This original work was published in the American Journal of Roentgenology. In addition, a podcast, “Pediatric COVID-19: What Radiologists Need to Know”, with first author Alexandra Foust, DO, and senior author Edward Y. Lee, MD, MPH, chief of the Division of Thoracic Imaging at Boston Children’s, summarizes the team’s findings.
Characteristic halo sign

“One of the main differences with COVID-19 in children is the presence of a “halo” sign on a chest image,” says Lee. “So far, they are only seen in pediatric cases, not in adults, and it appears early.”
The halo sign includes two parts: a central opacity (consolidation) which blocks out underlying lung structure with a ring-like surrounding hazy area referred to as ground-glass opacity (GGO).

The “halo” sign also appears in infectious aspergillosis or other fungal infections, particularly in immunocompromised children, so care should be taken when making a diagnosis.
“On chest X-ray, the most suggestive imaging pattern for COVID-19 in children is bilateral peripheral predominant GGO, or consolidation, in the mid and lower lung zones,” says Foust. However, X-rays may be normal also.
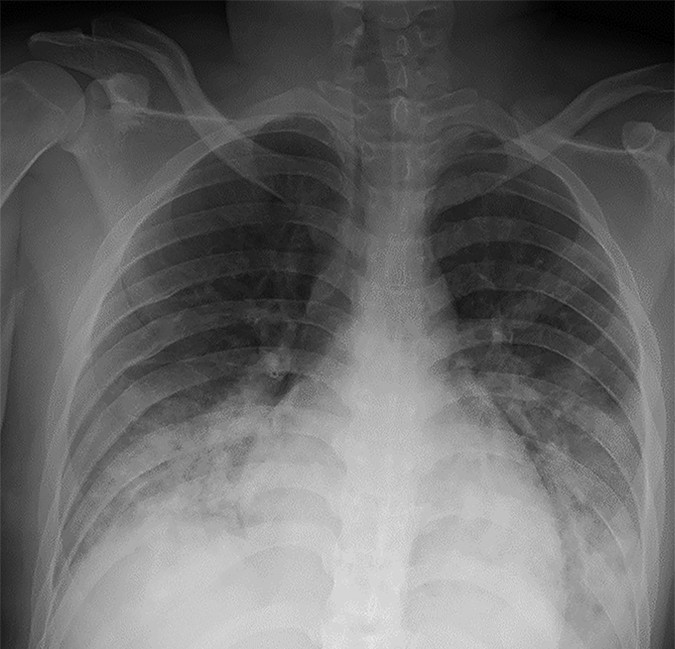
Chest computed tomography (CT) tends to provide more detail than X-ray and often shows a greater extent of disease.
“On chest CT, the most typical pattern includes bilateral GGO, or consolidation, in a peripheral subpleural location, predominantly in the mid and lower lung zones,” adds Foust.
Signs change as disease progresses
The authors also learned that the lung images change over time. In early stages, the halo sign may be the first indication of localized inflammation. As the disease spreads to surrounding alveoli, images take on patterns of diffuse ground glass. As the alveoli become filled with fluid or inflammatory cells, the ground glass becomes more consolidated until the infection appears to overwhelm lung structures.
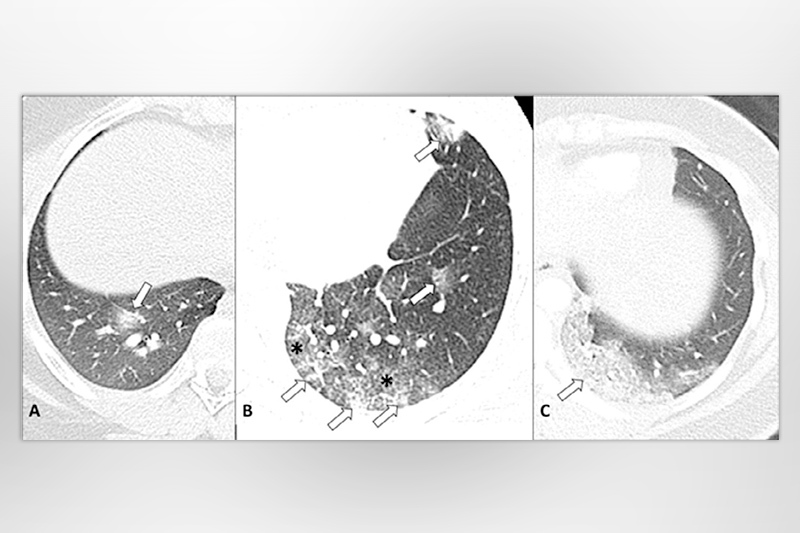
International perspective for imaging guidelines
To help guide the appropriate use of imaging for COVID-19 in children, authors from Boston Children’s participated in creating new recommendations on when to conduct imaging studies for COVID-19 in children. Their findings are published in the journal Radiology: Cardiothoracic Imaging.
“These recommendations are a practical guide for clinicians and radiologists that can properly optimize the use of imaging for possible screening and diagnosis of a child for COVID-19,” says Lee, who is corresponding author of the pediatric COVID-19 imaging guidelines.
The authors for these guidelines — which also includes experts from Hong Kong, Europe, Brazil, United Arab Emirates, and South Africa — created a set of five criteria to consider when deciding if an X-ray or CT should be ordered for a pediatric patient. “For consideration of imaging evaluation, we emphasize that you have to look at individual pediatric patients and situations as a whole rather than just focusing on disease itself,” says Lee.
The authors of the guidelines stress that the underlying medical problems in children to consider in COVID-19 are usually different from those in adults. “It’s not cardiovascular disease and diabetes like we see in adults,” says Lee. “Instead, it’s premature birth, underlying congenital disorders, or other infectious diseases like TB or HIV in some parts of the world.”
When to image?
To further guide treatment decisions, the authors created three separate recommendations for obtaining an initial image, performing images over time during COVID-19 infection, and imaging after recovery.
Over time, imaging studies should only be repeated when assessing a response to therapy, evaluating clinical deterioration, or assessing positioning of life support devices.
After a child recovers from infection — meaning symptoms disappear or test results are consistently negative — imaging is not recommended for asymptomatic patients with a mild disease course. It might be appropriate in children who initially had moderate-severe disease in the hospital and the clinician is concerned about permanent lung damage. And the authors recommend that post-recovery imaging is appropriate for children whose symptoms persist, resurface, or worsen to check for post-infectious lung injury.
Get more answers about Boston Children’s response to COVID-19.
Related Posts :
-

Promising advances in fetal therapy for vein of Galen malformation
In 2024, Megan Ingram* of California and her husband were preparing for the birth of their third child when a 34-week ...
-

The hidden burden of solitude: How social withdrawal influences the adolescent brain
Adolescence is a period of social reorientation: a shift from a world centered on parents and family to one shaped ...
-

A toast to BRD4: How acidity changes the immune response
It started with wine. Or more precisely, a conversation about it. "My colleagues and I were talking about how some ...
-

A unique marker for pericytes could help forge a new path for pulmonary hypertension care
Pulmonary arterial hypertension (PAH) is a rare condition that’s difficult to treat. The hallmarks of the disease — narrowing of ...







