Supercharged marrow transplant: Zebrafish reveal drugs that aid engraftment
Bone marrow transplantation, a.k.a. stem cell transplantation, can offer a cure for certain cancers, blood disorders, immune deficiencies and even metabolic disorders. But it’s a highly toxic procedure, especially when a closely matched marrow donor can’t be found. Using stem cells from umbilical cord blood banked after childbirth could open up many more matching possibilities, making transplantation safer.
Except for one problem. “Ninety percent of cord blood units can’t be used because they’re too small,” says Leonard Zon, MD, who directs the Stem Cell Research Program at Boston Children’s.
But what if the blood stem cells in those units could be supercharged to engraft more efficiently in the bone marrow and grow their numbers faster? That’s been the quest of the Zon lab for the past seven years, in partnership with a see-through zebrafish called Casper.
Because these fish are see-through, Zon and colleagues can image them to visually compare rates of engraftment when different chemicals are added to their water—in a high-throughput, automated test system.
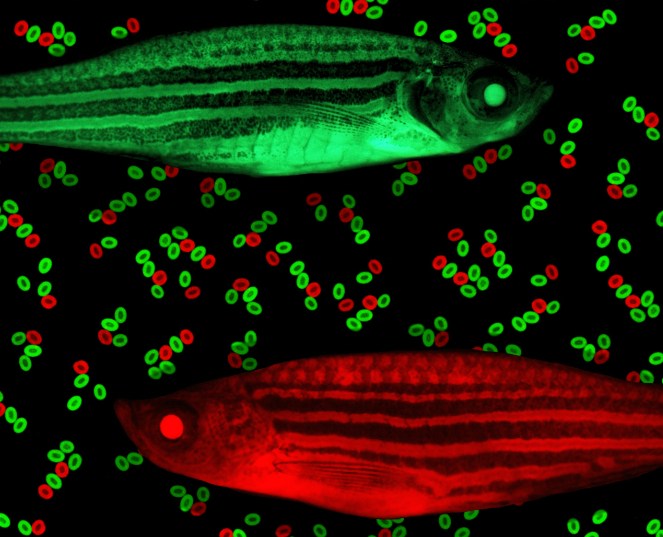
Red fish, green fish
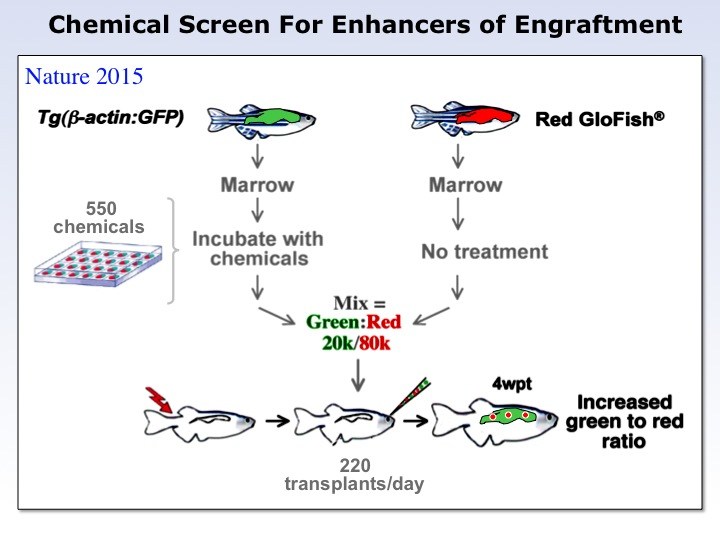
In what Zon fondly terms the “Dr. Seuss experiment,” described in the July 23rd issue of Nature, a team led by Pulin Li, PhD, Jamie Lahvic and Vera Binder, MD designated some of the zebrafish as donors and chemically tagged their marrow to glow either green or red.
They then removed some of the stem cells for transplantation, incubating the green cells with one of 550 test chemicals, but leaving the red cells untreated. They then injected a mix of treated and untreated stem cells into a cohort of recipient zebrafish. The researchers then tracked the cells’ activity and measured the green:red ratio in each fish.
“We call this a competitive transplant model because we can literally compete a green stem cell against a red stem cell and see what wins,” says Zon. “The expectation was that if chemical didn’t increase engraftment, all the fish would be equal parts red and green. But if it was effective, green marrow would predominate.”
That was the case for green marrow incubated with compounds known as epoxyeicosatrienoic acids, or EETs. EETs consistently produced green-glowing fish, boosting stem cell engraftment over thousands of marrow transplants.
“In a mouse system, this experiment would cost $3 million,” notes Zon. “In fish, it cost about $150,000.”
The team did conduct a smaller-scale set of mouse experiments, and confirmed EETs’ efficacy in promoting homing and engraftment of transplanted blood stem cells in a mammalian model.
From tank to bedside
Zebrafish have already helped Zon’s team screen for compounds that boost blood stem cell number—most notably prostaglandin, currently in several clinical trials under the name ProHema. What’s different here is that the new screen specifically sought candidate drugs that would increase the stem cells’ transplantability and engraftment.

EETs are chemical cousins of prostaglandin, and like prostaglandin they are essentially fats, are derived from arachidonic acid and are made during inflammation. Unlike prostaglandin, EETs appear to work by stimulating cell migration, an essential ingredient of engraftment, by activating a pathway known as PI3K. (This was demonstrated not just in fish and mice, but also in human blood vessel cells in a dish.)
“For years, people have thought that there are proteins and sugars that influence how stem cells migrate, but we’re finding that the lipids are really affecting the migration pathway,” says Zon.
After more studies to tease out how EETs work in human cells, Zon hopes to begin clinical trials in patients with cancer and blood disorders within the next two years. EETs would likely be tested in the setting of cord blood transplant to see if their use would make cord blood transplant a more viable option.
“Being able to get engraftment allows you to pick a smaller cord blood sample that might be a better match,” Zon says.
The lab is also investigating its other top hits from the zebrafish screen.
“Every new pathway that we find has the chance of making stem cell engraftment and migration even better,” says Zon. “I think we’ll end up being able to manipulate this process.”
Related Posts :
-

Mapping ‘neighborhoods’ in aggressive childhood brain tumors
The third-most common kind of childhood brain tumor, supratentorial ependymoma, is an aggressive cancer that often returns after surgery and ...
-

A true hero’s journey: How a team approach helped Wolfie overcome pancreatitis
Wolfgang, affectionately known as “Wolfie,” is a bright and energetic 7-year-old with a quick wit and a love for making ...
-

A toast to BRD4: How acidity changes the immune response
It started with wine. Or more precisely, a conversation about it. "My colleagues and I were talking about how some ...
-

Tough cookie: Steroid therapy helps Alessandra thrive with Diamond-Blackfan anemia
Two-year-old Alessandra is many things. She’s sweet, happy, curious, and, according to her parents, Ralph and Irma, a budding ...





