Libby’s story: Finding a surgical path to seizure control

Seven years ago, while my husband was visiting his parents in Washington, D.C., I traveled with our 3-year-old daughter, Libby, to Boston Children’s Hospital via ambulance from New Hampshire. Libby had been sick with a bad cold and had been acting unusually, with short episodes of rapid eye movement and stuttered speech.
An epilepsy diagnosis
After the emergency room at our local hospital confirmed my observations, they sent us to Boston Children’s. An MRI found she had cortical dysplasia, a common cause of epilepsy, and an electroencephalogram (EEG) confirmed epilepsy. At that point, the doctors prescribed the first of several anti-seizure medications. Life as we knew it had suddenly changed, we were numb and unable to comprehend what this meant, for Libby, our family, and her future.
Over the next few months, we spent a lot of time on 9 North under the care of an amazing team of nurses and doctors (including Drs. Arnold Sansevere, Jeffrey Bolton, Chellamani Harini, Heather Olson, and Mark Libenson, and are sure we are missing a few).
Medication first, then surgery
Initially, Libby had some response to the medication, though not total seizure control. The hope was to hold the line with medication as best as we could until Libby was older — around 8 — when we would schedule surgery. At that age, she’d be better able to understand the verbal instructions the doctors would give her to map the critical functions of her brain.
The team thought this would be the best approach due to the location of her seizure activity in the left temporal lobe, which is the area that controls language. As time went on, we had extended periods of seemingly good seizure control, however, there were days when she was having as many as 25 clinical focal seizures a day.
A new surgical plan
Two years later, when Libby was 5, her seizures spiraled out of control. It was July 2014, and we had just moved back to Virginia. We were scheduled to see a neurologist at Children’s National in Washington, D.C., on July 28 to coordinate Libby’s daily care and medicine plan while maintaining an eye toward surgery in Boston in a few years.
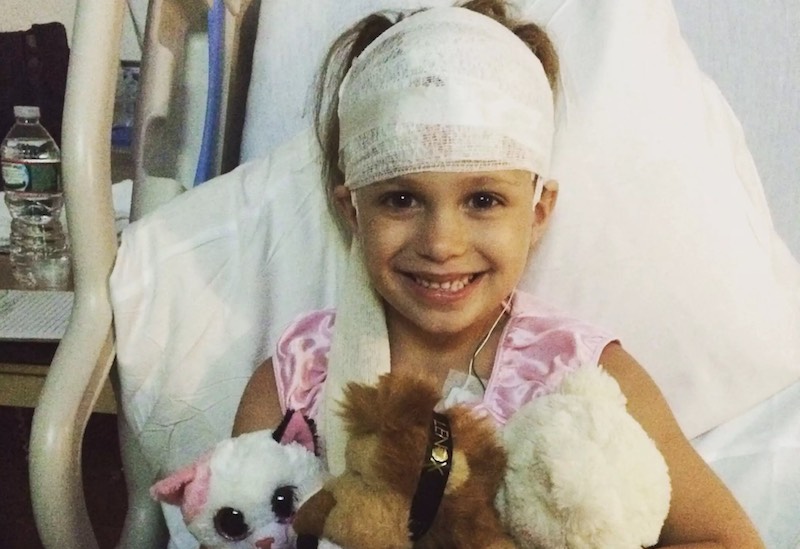
The seizures, as they always do, had a different plan. On the morning of July 13, we had just finished church service when Libby got sick in the car. We had noticed that her seizure activity had significantly increased the previous day or two, and this concerned us.
We made the drive into Washington, D.C., and spent a week inpatient while the doctors there monitored Libby’s seizures and consulted with their former colleague, Dr. Phillip Pearl, who had recently been appointed the director of the Epilepsy Center at Boston Children’s. Libby’s seizures were not responding to medicine in the manner that we had all hoped, so after much consultation it was determined that Libby would head to Boston for surgery.
Back to Boston for surgery
Upon arriving in Boston, we had the opportunity to listen to the surgical plan, including grids and strips, with the hope to remove the brain tissue that was causing the seizures. Grids and strips is an invasive type of monitoring to try to locate the source of the seizures by implanting electrodes in the brain. This procedure is done only when it’s very difficult to locate the seizures. Dr. Pearl took more time than I ever would have expected to listen to our journey and to clearly explain the risks involved.
Neurosurgeon Dr. Joseph Madsen and the team would be conducting surgery in a “high-rent district” of the brain, an area that controls not only language reception, but also homeostasis of the body as well as mood and heart rate.
After much deliberation and consultation, we kissed our girl on the cheek and laid her on the surgical table. We handed her life and our hearts over to Dr. Madsen and the amazing neurosurgical team that day and were thrilled when Libby remained seizure-free for a little over a year following that first round of surgery.
More seizures lead to another round of surgery
However, once we began to wean her off the medication, the seizure activity returned and the second round of surgery was scheduled. This time Dr. Scellig Stone, newly on the team, was brought in to coordinate with Dr. Madsen on a new type of monitoring called stereoelectroenphalography (SEEG). SEEG is a procedure that allows for deeper brain monitoring, even though it is less invasive and better tolerated in kids. Dr. Stone showed a level of care that I can’t say enough about. He treated Libby as one of his own.
Seeing improvements, facing all challenges
Since that time, we have seen tremendous improvements. Although Libby is not completely free from abnormal EEG readings at this time and remains on one anti-seizure medication, we are no longer losing sleep each night counting her seizures or telling Libby to sit down every time she hears an aura. And Libby is no longer concerned about having multiple seizures during her school day.

Today, Libby is a 10-year-old young lady who has the grit and perseverance to face any challenges that come her way. She is in the fourth grade, riding bikes, doing handstands, engaging in the classroom, and playing with friends. Life is good and her future is bright. We thank her entire team at Boston Children’s for the role they played in getting her to this point in her life.
Learn more about the Epilepsy Center.
Related Posts :
-

Mapping ‘neighborhoods’ in aggressive childhood brain tumors
The third-most common kind of childhood brain tumor, supratentorial ependymoma, is an aggressive cancer that often returns after surgery and ...
-

The dopamine reset: Restoring what’s missing in AADC deficiency
In March 2023, a young girl came to Boston Children’s Hospital unable to hold up her head — one striking symptom ...
-

“Princess June” reigns supreme over Rasmussen syndrome
What do you call a “girly” 5-year-old who adores dolls and frilly nightgowns? If you’re one of June Pelletier’...
-

What orthopedic trauma surgeons wish more parents knew about lawnmower injuries
Summer is full of delights: lemonade, ice cream, and fresh-cut grass to name a few. Unfortunately, the warmer months can ...





