Could leukemia be stopped before it starts?
Acute myeloid leukemia (AML), a blood cancer affecting both adults and children, requires more than one genetic “hit” to develop. As we age, many of us acquire a mutation that enables certain of our blood cells to multiply faster than others, forming their own distinct population. This first hit, known as “clonal hematopoiesis of indeterminate potential,” or CHIP, isn’t necessarily harmful.
But if a second hit comes that makes those cells malignant, “it’s essentially a guarantee you will get leukemia in the not-too-distant future,” says Scott Armstrong, MD, PhD, president of the Dana-Farber/Boston Children’s Cancer and Blood Disorders Center. The result is a rapid buildup of immature, dysfunctional blood cells.
In new research, Armstrong and his colleagues suggest that interfering with this second hit, using a compound that is in preclinical studies and appears so far to be safe, could prevent AML before it gets started. Their study was published last week in Science.
Update: Clinical trial now enrolling
This study and related research have now led to a clinical trial of this therapeutic approach, using a drug called SNDX-5613. The trial began in adults and is now open to children as young as 1 month of age with relapsed or refractory acute leukemia (ALL, AML, or mixed lineage). Patients with NPM1 mutations or KMT2A (MLL) gene rearrangements are eligible. See the trial protocol for more information.
“The idea is that you would screen people and follow those who have clonal hematopoiesis, and treat people who develop the second mutation,” says Armstrong.
Early intervention for acute myeloid leukemia
The researchers worked with mice that had the first hit, a mutation in the gene DNMT3A that is associated with CHIP. When they introduced the second hit, a mutation in the gene NPM1, the mice went on to develop leukemia. But if these mice were treated early with a compound called VTP-50469, the premalignant blood cells stopped multiplying and leukemia never developed. There were no apparent toxic effects.
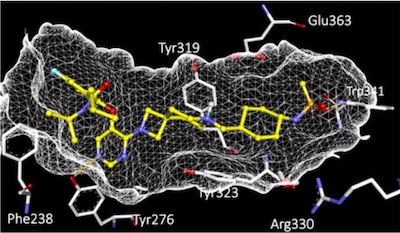
“We eradicated the cells that would ultimately become leukemia cells,” says Armstrong. “This is one of first times we’ve had a molecule that’s effective and can act selectively on preleukemic cells rather than normal cells. We treated the mice for many weeks, and they’re just fine.”
Learning from infant leukemias
VTP-50469 came out of earlier research by Armstrong and colleagues on rare, high-risk infant leukemias known as MLL-rearranged leukemias. The compound targets a complex of proteins that join together and turn on the genes driving the leukemia. VTP-50469 disrupts two proteins in this complex, Menin and MLL, and the complex falls apart, so the leukemia genes turn off.
In the infant leukemia study, done in mice and leukemia cell lines, VTP-50469 treatment led to sharp decreases in the number of leukemia cells, and, in some animals, remission of the cancer. Normal blood cells were unharmed.
“It also turns out that more common adult leukemias are using these same mechanisms,” says Armstrong.
A close cousin of VTP-50469 is now in clinical trials in adults with relapsed AML, and Armstrong hopes to see a similar trial launched in children with AML this year.
A model for preventive care?
While screening everyone over a certain age for clonal hematopoiesis may not be practical yet, one could imagine screening people who are thought to be at heightened risk for AML, such as those who have had chemotherapy before, or in whom problems in the blood system are suspected.

The same preventive care concept could potentially also apply to other cancers that involve multiple hits, Armstrong believes.
“You need to know which mutations are important, and the order of the mutations, and you need to have a drug that’s relatively nontoxic, since you’re talking about a patient that, at that time, isn’t sick,” he says. “If you have a molecule that targets one of the early mutations, that’s really the holy grail: being able to intervene early in the cancer development process.”
Hannah J. Uckelmann of Dana-Farber/Boston Children’s Cancer and Blood Disorders Center was first author on the Science paper. The study was supported by the National Institutes of Health (CA176745, CA204639, CA066996, CA206963, P30 CA008748 and U54 OD020355-04), Wicked Good Cause, Cookies for Kids’ Cancer, SFB, the German Research Foundation (DFG, UC77/1-1) and Cancer Research UK (C22324/A23015).
Related Posts :
-

Mapping ‘neighborhoods’ in aggressive childhood brain tumors
The third-most common kind of childhood brain tumor, supratentorial ependymoma, is an aggressive cancer that often returns after surgery and ...
-

A true hero’s journey: How a team approach helped Wolfie overcome pancreatitis
Wolfgang, affectionately known as “Wolfie,” is a bright and energetic 7-year-old with a quick wit and a love for making ...
-

A toast to BRD4: How acidity changes the immune response
It started with wine. Or more precisely, a conversation about it. "My colleagues and I were talking about how some ...
-

A new druggable cancer target: RNA-binding proteins on the cell surface
In 2021, research led by Ryan Flynn, MD, PhD, and his mentor, Nobel laureate Carolyn Bertozzi, PhD, opened a new chapter ...





