Biocontainment Unit supports nurses on the frontlines of infection control
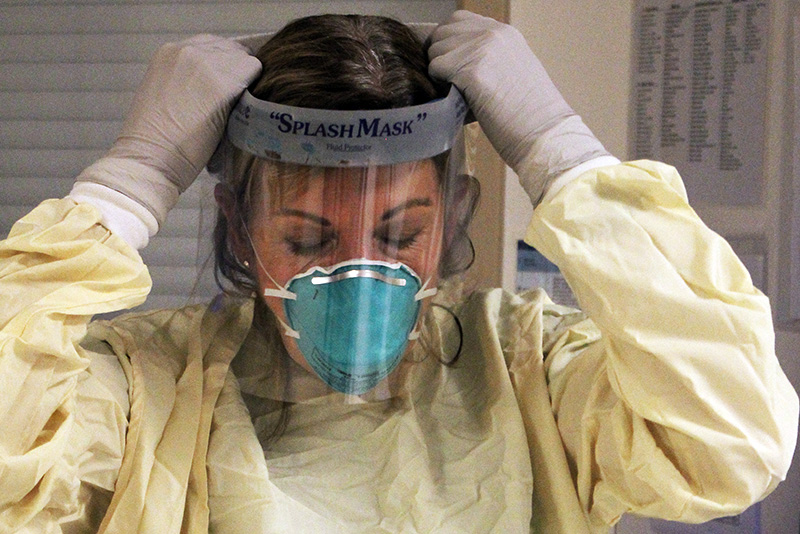
When cases of COVID-19 began to mount this winter, Boston Children’s Hospital was ready to spring into action — in fact, the hospital has been preparing for such a pandemic for six years. In collaboration with Boston Children’s Chief of Medical Critical Care, Michael Agus, MD; Hospital Epidemiologist and Medical Director of Infection Prevention and Control, Thomas Sandora, MD, MPH; and Jon Whiting, MSN, RN, CCRN, director of Nursing Patient Operations for the hospital’s Medical Intensive Care Unit (MICU), Biocontainment Unit (BCU), and Life Support Programs, a team of highly specialized nurses from throughout the hospital was activated. Their mission: to educate and support staff in suiting up and carefully removing personal protective equipment (PPE) while keeping themselves safe and reducing the potential to inadvertently spread the virus in the process.
The BCU is comprised of a small inpatient setting staffed by a virtual team drawn from nurses and other clinicians throughout Boston Children’s. The unit was originally established in response to a prior infectious disease outbreak. When the Ebola crisis took hold in West Africa in 2014, “We viewed this as an opportunity to expand our own preparedness,” says Whiting, who — with the support and advocacy of Patricia A. Hickey, PhD, RN, NEA-BC, FAAN, vice president and associate chief nurse of Cardiovascular and Critical Care Nursing Patient Operations — collaborated with other forward-thinking Boston Children’s clinicians to develop hospital guidelines and protocols for the care of patients with highly infectious diseases.
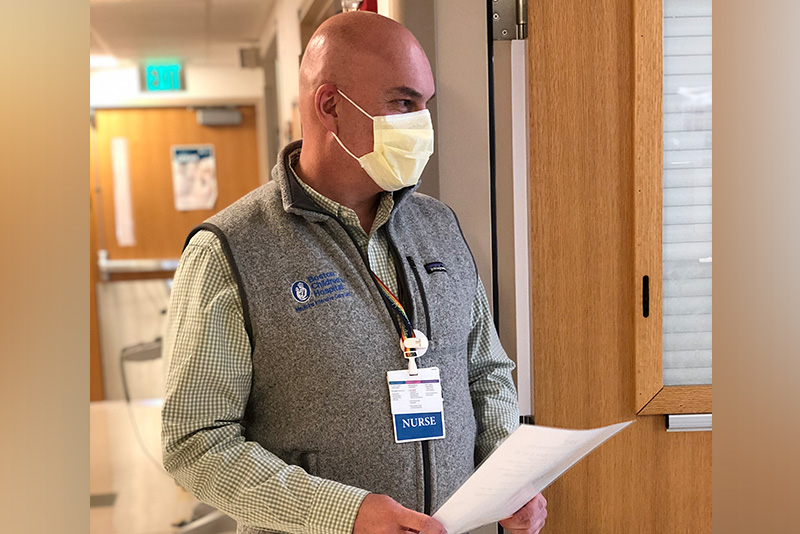
“The BCU team is available 24/7 to educate and support frontline staff in the use of PPE, assist with patient transfers, and prepare frontline clinical and support staff to care for these patients,” explains Pascale Audain, BSN, RN, CCRN, who works in the hospital’s MICU and BCU. The BCU team nurses possess a broad range of clinical experience, including inpatient acute care, intensive care, cardiology, and emergency medicine. Many, including Audain and her colleague, Nick Barry, BSN, RN, have been volunteering in the BCU since its inception. “We act as a common thread between different parts of the hospital, facilitating communication between nursing, intensive care, infection control, environmental services, respiratory therapy, and physician colleagues,” says Barry.
Simulation has been tightly integrated into the work of the BCU since its inception. The clinical team has long practiced full-scale simulated drills to prepare staff for the arrival of a patient with a highly infectious disease. During these drills, “We’ve spent up to four hours in the BCU to learn how to optimize care delivery processes before we’re in a real high-stakes situation,” says Barry.
Today, as clinical team members and nurses find themselves in the midst of just such a circumstance, that preparation has paid off. “In a time characterized by so much uncertainty, this work has been very grounding,” says Audain. “There’s a real appreciation at Boston Children’s for the role of nurses as central to care delivery and the patient and family experience — we’re all working towards the same goal.” And it’s powerful proof that when it comes to innovation, nurses don’t just have a seat at the table. They’re leading the way.
Related Posts :
-

“Observe. Be open.”: How Boston Children’s nurses are changing the future of global health
Ashley Birch, MSN, CPNP, a Boston Children’s pediatric nurse practitioner and Global Nursing fellow, didn’t expect a trash ...
-

Model enables study of age-specific responses to COVID mRNA vaccines in a dish
mRNA vaccines clearly saved lives during the COVID-19 pandemic, but several studies suggest that older people had a somewhat reduced ...
-

New insight into the effects of PPIs in children
Proton-pump inhibitors (PPIs) are frequently prescribed to suppress stomach acid in patients with gastroesophageal reflux disease (GERD). Prescribing rates of ...
-

Creating the next generation of mRNA vaccines
During the COVID-19 pandemic, mRNA vaccines came to the rescue, developed in record time and saving lives worldwide. Researchers in ...