When surgery shapes your life: Moyamoya patient turned doctor

Elizabeth Kwak is living proof of how far the treatment of moyamoya has come. Twenty-four years ago, Elizabeth had pial synangiosis, a surgical treatment for moyamoya that was pioneered by Boston Children’s Hospital neurosurgeon Dr. R. Michael Scott in 1985. Today, Elizabeth is a fourth-year medical student at Drexel University College of Medicine. She talks about her experience with moyamoya and how it has dramatically shaped the course of her life.
What do you remember about having moyamoya as a child?
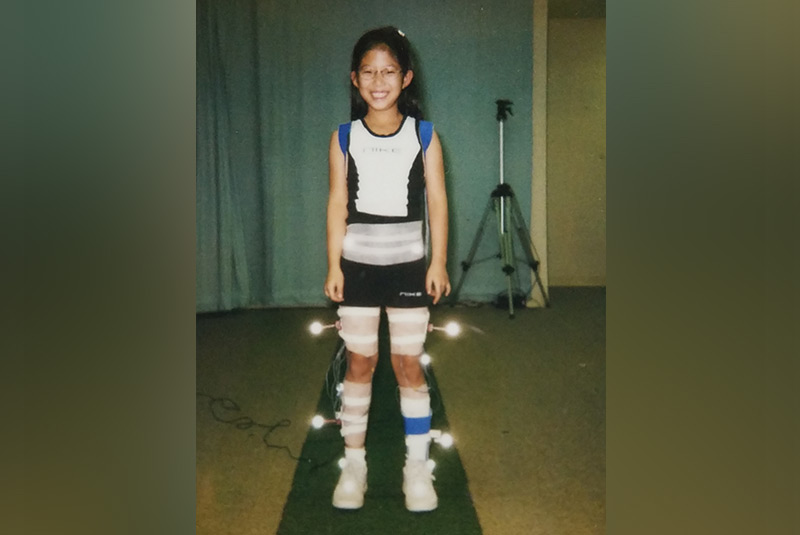
I don’t remember much, as I was so young. But, I do remember I tripped a lot because of the weakness on the left side. I had complete paralysis on the lower left side from a stroke that happened before I was diagnosed. I needed intensive physical therapy to strengthen the left side for many years. Despite this, I could still play and have fun like other kids my age. I even took ballet lessons and joined a soccer league. I still trip over my left leg a little bit when I’m tired, but it’s not interfering with my daily life.
What do you remember about your treatment for moyamoya?
I was diagnosed with moyamoya a few months before I turned 3 years old, and vaguely recall traveling with my parents from our home in Tennessee to Boston for treatment. It was a really long surgery and my parents were very worried. I remember telling my mom, “Don’t worry, I’ll be fine,” prior to being wheeled to surgery.
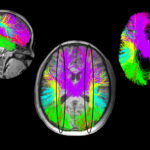
As I was growing up, my parents shared pieces of my treatment and recovery with me, but it wasn’t until I was a sophomore in high school that I had the capacity to understand what really happened to me. That year, I had been assigned an open-ended project presentation and chose moyamoya as the topic to learn more about it. I showed the class scans of my brain on one of those old-fashioned projectors and explained how moyamoya caused the blood vessels to narrow.
When did you know you wanted to be a doctor?
As I did my research, I found Dr. Scott and learned about the innovations he had implemented for moyamoya surgery. I remember thinking as I saw his photo, that he looked like the nicest, sweetest person. As I reflected on how my life had been changed for the better by Dr. Scott, I felt compelled to pay it forward just like Dr. Scott did for me. That was the deciding point. I knew I could help people through medicine.
What brought you to back to Boston Children’s?
When I was a junior in college, I came back as a research assistant in Dr. Edward Smith’s lab to help the larger medical community understand moyamoya. For three months, I researched the genetic underpinnings of moyamoya by looking at our patients’ family trees. It’s really important for us to understand how likely it is that a child will have moyamoya if one of their family members does. In addition to research, I went into the operating room with Dr. Smith and observed the same surgery I had undergone years ago. It was surreal. I also observed Dr. Smith with patients and their families, and saw the impact of listening to families and compassionately addressing their health concerns.
How has your personal experience with moyamoya motivated you?
When I observed Dr. Smith in consultation and in surgery, I saw first-hand how affected the families were by the new diagnosis. This reaffirmed my commitment and passion for medicine. My love for children and medicine came together. The core of my soul is pediatric medicine. I can draw upon my own experience with brain surgery, migraines, and seizures to provide hope and medical care through a partnership with the patients and families.
What do you think makes a great doctor?
Apart from competence, it’s very important to listen to the patient and their family. It is crucial to create a treatment plan in partnership with the patient and family by truly listening, to formulate what works best for them. Being able to connect with them through understanding their worries and fears will build trust and enhance the doctor-patient partnership.

What’s next for you?
I just finished a rotation in child neurology at Boston Children’s. I knew immediately when I started the rotation and had the chance to work with the amazing faculty here that I wanted to apply to child neurology residency programs. I am currently in the midst of interviews and will hopefully know in mid-March where I will continue my training.
Learn more about the Moyamoya Program.
Related Posts :
-

The dopamine reset: Restoring what’s missing in AADC deficiency
In March 2023, a young girl came to Boston Children’s Hospital unable to hold up her head — one striking symptom ...
-

Unveiling the hidden impact of moyamoya disease: Brain injury without symptoms
Moyamoya disease — a rare, progressive condition that narrows the brain’s blood vessels — leads to an increased risk of stroke ...
-

The thalamus: A potential therapeutic target for neurodevelopmental disorders
Years ago, as a neurology resident, Chinfei Chen, MD, PhD, cared for a 20-year-old woman who had experienced a very ...
-

Could peripheral neuropathy be stopped before it starts?
An increase in high-fat, high-fructose foods in people’s diets has contributed to a dramatic increase in type 2 diabetes. This, ...