Immune cells “sculpt” brain circuits — by eating excess connections
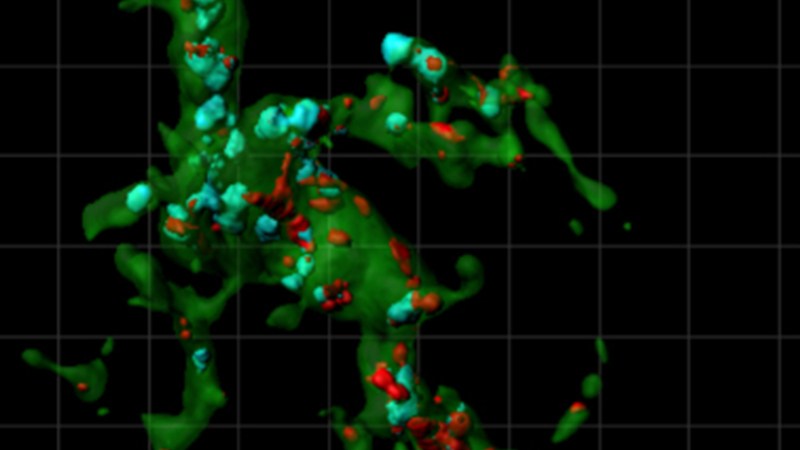
The image above and the movie below show an immune cell caught in the act of tending the brain. The cell below has just eaten away unnecessary connections, or synapses, between neurons.
That’s not something these cells, known as microglia, were previously thought to do. As immune cells, it was thought that their job was to rid the body of unwanted pathogens and debris, by engulfing and digesting them.
The involvement of microglia in the brain’s development has started to be recognized only recently. The latest research finds that microglia tune into the brain’s cues, akin to the way they survey their environment for invading microbes, and get rid of excess synapses the same way they’d dispatch these invaders—by eating them.
It’s a whole other way of understanding how the healthy brain develops—at the hands of cells that were once thought to be merely nerve “glue” (the literal meaning of “glia” from the Greek), playing a protective role to neurons, say investigators Beth Stevens, PhD, and Dori Schafer, PhD, of the F.M. Kirby Neurobiology Center at Boston Children’s Hospital.
“In the field of neuroscience, glia have often been ignored,” says Stevens. “But glia aren’t the nerve glue, they’re actively communicating with neurons. People have gotten a new respect for glia and are hungry to know more about them.”
Such knowledge could eventually shed light on brain disorders ranging from autism to Alzheimer’s.
The “eat me” sign
We’re all born with more brain connections than we need. As we begin to encounter our world, they’re trimmed back to fine-tune our circuitry. It’s a bit of an oversimplification, but Stevens and Schafer demonstrated last week in the journal Neuron that when two neurons start talking to each other less – because their connection is no longer important to our lives– the microglia notice that and prune the synapse away.
To study microglia’s pruning activity, Stevens and Schafer used a time-honored model: the visual system. When you cover one eye soon after birth, you force the brain to rewire: Brain connections with the covered eye weaken and those synapses eventually get eliminated.
“\We think that weaker synapses are being tagged, and that microglia are eliminating them just as macrophages would eliminate bacteria.” –Beth Stevens, PhD
Using this model, Stevens and Schafer showed that microglia take their cues from a set of signals also used by the immune system, known as the complement cascade. Specifically, microglia carry receptors that recognize the complement protein C3 — the same protein found on synapses that are destined for elimination.
“We think that weaker synapses are being tagged with C3, and that microglia are eliminating them just as macrophages would eliminate bacteria,” says Schafer. “C3 is like an ‘eat me’ signal.”
As a postdoctoral fellow in 2007, Stevens showed that neurons are loaded with complement proteins soon after birth, just when pruning is at its peak. In the new study, she and Schafer deliberately disrupted complement signaling in mice—stripping the microglia of C3 receptors, or blocking those receptors with a drug. When they did so, pruning of irrelevant synapses didn’t occur.
Stevens thinks their findings might have relevance for brain disorders. Developmental brain disorders such as autism, epilepsy or schizophrenia are increasingly seen as disorders of synapse development, and some data suggest that microglia and/or the complement cascade are involved.
At the other end of the spectrum, scientists have noted that microglia — normally in a resting state in adults — are activated in neurodegenerative diseases like glaucoma, Alzheimer’s disease, Lou Gehrig’s disease, Huntington’s disease and Parkinson’s disease. Subtle changes have been found in synapses that might cause them to be targeted for elimination.
So could targeting microglia or the complement cascade prevent synapse loss or alter pruning in these diseases? “All this is still very speculative,” Stevens cautions. “We first need to understand normal brain development.”
Related Posts :
-

Small gains with big meaning: Loic’s story of deep brain stimulation for PKAN care
Loic, 5, lives in Montana with his parents, Sherine and Mark, and his sister, Selah. He loves Spider-Man, sushi, and the ...
-

The hidden burden of solitude: How social withdrawal influences the adolescent brain
Adolescence is a period of social reorientation: a shift from a world centered on parents and family to one shaped ...
-

The journey to a treatment for hereditary spastic paraplegia
In 2016, Darius Ebrahimi-Fakhari, MD, PhD, then a neurology fellow at Boston Children’s Hospital, met two little girls with spasticity ...
-

The dopamine reset: Restoring what’s missing in AADC deficiency
In March 2023, a young girl came to Boston Children’s Hospital unable to hold up her head — one striking symptom ...





