Five things parents should know about vascular rings

If your child has a high-pitched cough, breathes loudly, wheezes, has difficulty eating or swallowing, or always seems to be coming down with pneumonia or respiratory infections, the problem could be more complex than you realize. Although rare, abnormal formations of the blood vessels called vascular rings can compress the trachea, esophagus, or both. While some vascular rings may never cause problems, others can trigger symptoms ranging from mild to life threatening.
“First, we need to understand the issue,” says Dr. Russell Jennings, surgical director of the Esophageal and Airway Treatment (EAT) Center at Boston Children’s Hospital. “Each patient is unique and special and deserves a customized approach to correct their condition.” Here are five things every family should know about vascular rings.
1. There are many types of vascular rings.
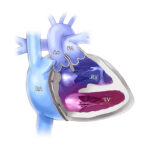
In general, a vascular ring occurs when a child’s aorta — the body’s largest blood vessel — or its branches form abnormally, so that it encircles and constricts the trachea and esophagus. The type of vascular ring a child has can be as unique as they are, but some are more common than others. For example, in a common type of vascular ring called double aortic arch, a child is born with two aortic arches. The branches from these two aortic arches surround the trachea and esophagus.
In another type of vascular ring called right aortic arch with aberrant subclavian and left ligamentum, the child’s aortic arch curves right and the left subclavian artery, which branches from the aortic arch, passes behind their esophagus and airway instead of in front of the airway. The ligamentum arteriosus (a blood vessel remnant) passes between the left subclavian artery and left pulmonary artery, completing the ring.
2. It’s not just a blood vessel problem.
As their name suggests, vascular rings are caused by malformed blood vessels. But the vessels themselves aren’t really the issue, explains Dr. Jennings. Instead, symptoms occur when a vascular ring puts pressure on a child’s esophagus, trachea, or both. Not all patients with vascular rings need surgery. In fact, some people without symptoms may live their entire lives not even realizing that they have a vascular ring. More often, however, the condition causes a variety of respiratory and digestive woes. Because few physicians are well versed in vascular rings, the symptoms they cause can go untreated or may be misdiagnosed as asthma or recurrent croup.
3. Vascular rings often accompany tracheomalacia.
For some kids, vascular rings seem to go hand in hand with an airway disorder called tracheomalacia. In this condition, the trachea narrows or collapses when your child exhales, which makes it feel hard to breathe and may lead to a vibrating noise or cough. Tracheomalacia can result in recurring respiratory illnesses or make it difficult to recover from a respiratory illness. In the long term, it can lead to progressive lung injury. Like vascular rings, tracheomalacia can be present at birth, or it can develop in response to vascular rings or other anomalies.
4. Accurate diagnosis is key.
If your child has any symptoms of a vascular ring — particularly noisy breathing — your child’s doctor may refer you for testing. The gold standard for evaluating and identifying vascular rings is a computed tomography (CT) scan, says Dr. Jennings. This technique allows physicians to visualize your child’s vascular anatomy properly. Vascular rings can be diagnosed at any age, including while a child is still in the womb.
5. Comprehensive surgery is best.
Children who have symptoms from vascular rings usually need to surgery to relieve pressure on the airway and esophagus. Surgeons may use a variety of techniques to accomplish this, but the most effective approach involves a combination of procedures to move the aorta and any other blood vessels, as well as a complete resection of the diverticulum of Kommerell, which is typically left as an out-pouching of the aorta and compresses the esophagus and airway from the back. Surgeons may also treat tracheomalacia at this time.
Boston Children’s is the only hospital to address all of these problems in one comprehensive surgical repair. “At Boston Children’s, we are able to combine the specialties of cardiothoracic surgery with the EAT Center,” says Dr. Christopher Baird, a pediatric cardiac surgeon who performs these procedures with Dr. Jennings. “Combining our experience with the vascular structures and EAT’s experience with the esophagus allows us to provide the best outcomes when operating in the posterior mediastinum. This approach allows us to address all the problems at once rather than having to have multiple surgeries.”
Learn about the Esophageal and Airway Treatment Center.
Related Posts :
-

Biventricular repair linked to better outcomes in superior-inferior ventricles treatment
The complexity of superior-inferior ventricles — a condition in which one ventricle is positioned on top of the other — has often ...
-

A reunion of the heart: Grace and Amy bond through HLHS
At first glance, Grace and Amy have a pretty typical friendship: they joke around, cheer each other on, and keep ...
-

First-of-its-kind pressurization test could improve Ross procedure outcomes
The Ross procedure is a preferred surgery to treat severe aortic valve disease. The procedure replaces the failing valve ...
-

How a meniscal transplant made me a Boston sports fan
I was in kindergarten when my knee started popping and cracking. My parents and I didn’t know it at ...