Babies’ EEG patterns predict whether they will develop autism

Signs of autism spectrum disorder (ASD) typically start to become apparent only in a child’s second year of life or later, but earlier identification could allow children to receive interventions as babies, when they have greater brain plasticity and thus may receive more benefit. A new study in Nature Communications finds that periodic EEGs in babies, starting as young as 3 months of age, could allow ASD to be detected in a child’s first year, well before they start to show autism-like behaviors.
“There is an urgent need to develop objective biomarkers of autism that can be implemented in the first year of life,” says Charles Nelson, PhD, director of the Laboratories of Cognitive Neuroscience at Boston Children’s Hospital and Harvard Medical School and senior investigator on the study, part of the lab’s larger Infant Sibling Project. “First, such biomarkers might tell us which infants should be targeted for early intervention. Second, they may tell us something about the errors in brain development that lead to autism. And third, they may allow us to develop more personalized treatment strategies and determine which subgroups of children will respond best to which treatments.”
EEGs, available in most pediatric practices, measure brain electrical activity, and are usually used to diagnose or evaluate epilepsy. But the EEG signal also contains other kinds of information about the brain. One of them is strength of the different oscillations of different EEG frequency waves: alpha, beta, gamma, theta, and delta. Prior studies have linked each of these frequencies with different kinds of brain activity.
Tracking babies’ brain waves
The study enrolled 102 infants who were at higher risk for ASD by virtue of having an affected sibling, as well as 69 low risk infants — infants with a typically developing older sibling and no first- or second-degree family members with ASD. EEG measurements were taken at 3, 6, 9, 12, 18, 24, and 36 months of age, and the power of each frequency band was computed and tracked over time in both groups.
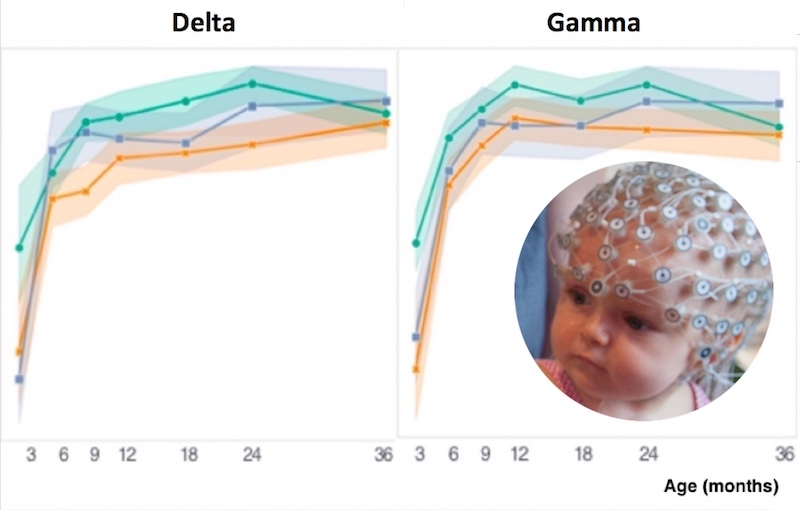
“Measuring EEGs in the same infants over years allowed us to test when in development EEG oscillations best differentiate later ASD outcomes,” says Laurel Gabard-Durnam, PhD, a research fellow in the Laboratories of Cognitive Neuroscience. “This longitudinal approach also enabled us to test whether measures of developmental change are themselves meaningful biomarkers of later outcomes compared to measures taken at a single age.”
Of the original 102 high-risk infants, 31 eventually met criteria for ASD. The data were then grouped and analyzed for three developmental time periods — 3 to 12 months of age, 12 to 24 months, and 3 to 36 months – in the frontal part of the brain, the temporal-parietal area and the whole brain. Infants were formally evaluated for ASD at 24 and 36 months of age using the standardized Autism Diagnostic Observation Schedule (ADOS) and clinical observations.
The key findings:
- EEG power in the frontal lobes within the first year of life best predicted whether a child would ultimately be diagnosed with ASD. Measurements closer to the age of diagnosis (when behavioral symptoms are more evident) did not add further useful information.
- Both single-timepoint EEG measures and EEG power trajectories (measures of developmental change in EEG frequency bands) emerged as robust predictors.
- Analysis of specific EEG frequency bands found that delta and gamma power trajectories consistently distinguished infants with eventual ASD diagnoses from the others. Infants ultimately diagnosed with ASD had steeper rates of increase in summed delta power during their first year, and further changes in delta power over the next two years added further predictive information. Over the first three years, summed gamma power also distinguished children with ASD from the others. High-risk infants later diagnosed with ASD had lower frontal gamma power at age 6 months and a lower rate of increase through age 3 years compared to the other groups.
The researchers see great promise in developing early EEG biomarkers for autism, but call for more research to validate their findings in independent samples.
“These results suggest that early brain development can provide a window to detect future ASD outcomes before behavioral symptoms emerge,” says Gabard-Durnam. “This early detection would give clinicians the best chance of improving outcomes for these infants through existing and new interventions.”
Coauthors on the study were Carol Wilkinson, Division of Developmental Medicine, Boston Children’s Hospital; Kush Kapur, Department of Neurology, Boston Children’s Hospital; Helen Tager-Flusberg, Boston University; and April Levin, Division of Developmental Medicine and Department of Neurology, Boston Children’s Hospital. The research was supported by the Autism Science Foundation, the American Brain Foundation, the Rett Syndrome Research Foundation, the Nancy Lurie Marks Family Foundation, the Brain and Behavior Research Foundation, the FRAXA Research Foundation and the National Institutes of Health (1T32MH112510, R01-DC010290).
Related Posts :
-

The hidden burden of solitude: How social withdrawal influences the adolescent brain
Adolescence is a period of social reorientation: a shift from a world centered on parents and family to one shaped ...
-

The journey to a treatment for hereditary spastic paraplegia
In 2016, Darius Ebrahimi-Fakhari, MD, PhD, then a neurology fellow at Boston Children’s Hospital, met two little girls with spasticity ...
-

New research shows caregiver instability affects development
According to some estimates, more than 100 million children around the world experience separations from their caregiver every year. Previous research — ...
-

The thalamus: A potential therapeutic target for neurodevelopmental disorders
Years ago, as a neurology resident, Chinfei Chen, MD, PhD, cared for a 20-year-old woman who had experienced a very ...





