Double stem cell transplant and other tools are helping children survive neuroblastoma
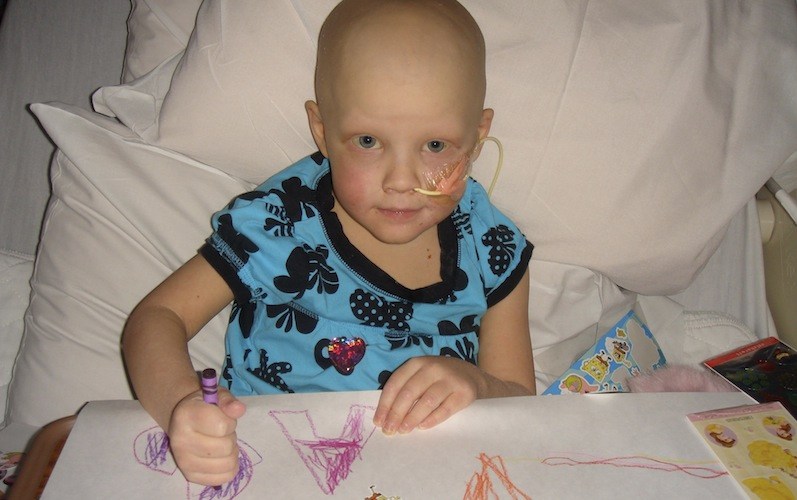
When Emily Coughlin complained of a sore knee in May 2009, doctors initially suspected Lyme disease. After antibiotics failed to relieve the pain, Emily was diagnosed with neuroblastoma, a cancer that begins in nerve cells outside the brain, just shy of her fourth birthday. Though neuroblastomia is rare — about 700 new cases occur annually in the United States — it is the most common cancer in infants and toddlers.
In the early 1990s, when Lisa Diller, MD, was starting her career at Dana-Farber/Boston Children’s Cancer and Blood Disorders Center, Emily would have faced five-year survival odds of less than 15 percent. “It was a devastating diagnosis,” recalls Diller, now chief medical officer of Dana-Farber/Boston Children’s.
Instead Emily, who loves drawing and soccer and her family’s golden doodle dogs, Obi and Agnes, has been cancer-free since 2010. “I don’t really think about it,” she says. She just celebrated her 11th birthday with a trip to the pool with friends, followed by pizza and cake at her Cape Cod home.
Emily successfully withstood newer, extremely rigorous treatments that spell hope for today’s neuroblastoma patients. In 2009, she participated in a randomized, multi-center Phase 3 trial that involved chemotherapy followed by back-to-back stem cell transplants. The transplants utilized Emily’s own previously harvested blood stem cells, allowing her to tolerate the extremely high doses of chemotherapy needed to destroy her cancer.
The recently announced results of this trial, co-led by Diller, herald a new standard of care for high-risk neuroblastoma, establishing that double transplants yield significantly better outcomes than a single transplant, the previous standard. Emily also benefited from the immunotherapy drug dinutuximab approved last year by the federal Food and Drug Administration, its first approval of a medication for high-risk neuroblastoma.
Today, neuroblastoma’s overall long-term survival rate exceeds 50 percent.
Double jeopardy for neuroblastoma
The road to improved outcomes began three decades ago, when researchers noticed that, in a laboratory dish, higher doses of chemotherapy killed neuroblastoma cells, while lower doses were ineffective.
At the time, the only way to deliver such high-dose chemotherapy was with the help of a bone marrow transplant. Patient’s bone marrow cells were harvested for safekeeping and returned to the body after intensive chemotherapy that would have destroyed the marrow. It was possible to harvest enough bone marrow cells from a young child for a single transplant, but not enough for a second transplant.
In the early 1990s, clinicians began harvesting circulating blood stem cells, instead of bone marrow, for transplants in adults. Could this technology — involving catheters, collection machines and many hours of time — be used in young children and infants? Convinced the problems could be surmounted, Diller and her colleagues developed the technology to safely harvest young children’s stem cells.
“Then,” Diller recalls, “we began to think, if one transplant is good, maybe two are better.”
Armed with the stem-cell collection technique, Dana-Farber/Boston Children’s pioneered tandem transplants for neuroblastoma, beginning in 1994. In 2007, the Children’s Oncology Group opened the randomized trial to definitively compare two transplants versus one.
The trial enrolled 652 patients newly diagnosed with high-risk neuroblastoma, most with Stage 4 (metastatic) disease. Their median age at diagnosis was 3.1 years. All were initially treated with surgery and six cycles of high-dose chemotherapy, with stem cells harvested for transplant after two rounds.
The results were striking. Three years after treatment, 62 percent of the children who received two transplants were alive and cancer-free, compared to 49 percent of those who underwent a single transplant, according to findings Diller and Julie R. Park, MD, of Seattle Children’s Hospital, recently presented to the American Society of Clinical Oncology.
Children who also received immunotherapy after transplant, as part of a second, linked study, fared even better: 74 percent of tandem transplant patients and 56 percent of single transplant patients were alive and cancer-free three years after treatment.
“The findings define a new standard for treatment,” Diller says.
Emily’s story
For Emily Coughlin’s parents, the decision to participate in the trial was difficult. “There was the possibility of subjecting her to a second transplant, and the transplants were only two weeks apart,” says Amy McHugh, Emily’s mother.
Emily first had six rounds of chemotherapy to reduce the softball-sized tumor, followed by an eight-hour operation to remove the tumor, which had shrunk to the size of a golf ball. Next came the back-to-back transplants, followed by 21 treatments with radiation and six months of antibody immunotherapy.
“Our other daughter was in first grade,” says McHugh. “My husband and I switched between hospital and home and didn’t see each other for 18 months. It was hard, but when you have to do something you just do it.”
The double transplant, as expected, was challenging. “Emily was in the intensive care unit twice during the first one,” McHugh recalls. “It was awful to have the intense experience of the first one and know she was going to go through it again. Luckily, the second one was a little easier for her.”
Today, Emily has put the experience behind her, though side effects of treatment remain.
“The protocol was so intense that many kids have issues,” McHugh says. “Emily has 25 percent of her kidneys and uses hearing aids because she lost 65 percent of her hearing. She has stunted growth, endocrine issues and sparse hair. But academically she does really well. She plays sports and has good friends. She has some collateral damage, physically, but her quality of life is really, really high.”
Only one of the children Diller treated for high-risk neuroblastoma in her early days as a pediatric oncologist survived his cancer. Today the Dana-Farber/Boston Children’s survivorship program cares for dozens of long-term survivors of the disease.
“As encouraging these new tools are, the fact remains that we are treating some of our youngest patients with the most toxic therapies in our arsenal,” Diller says. “While we continue to strive to improve survival, we must also seek ways to reduce the toxicity of our treatments.”
Learn more about Dana-Farber/Boston Children’s neuroblastoma program.
Read more of the greatest children’s stories.
Related Posts :
-

Mapping ‘neighborhoods’ in aggressive childhood brain tumors
The third-most common kind of childhood brain tumor, supratentorial ependymoma, is an aggressive cancer that often returns after surgery and ...
-

A true hero’s journey: How a team approach helped Wolfie overcome pancreatitis
Wolfgang, affectionately known as “Wolfie,” is a bright and energetic 7-year-old with a quick wit and a love for making ...
-

A toast to BRD4: How acidity changes the immune response
It started with wine. Or more precisely, a conversation about it. "My colleagues and I were talking about how some ...
-

A new druggable cancer target: RNA-binding proteins on the cell surface
In 2021, research led by Ryan Flynn, MD, PhD, and his mentor, Nobel laureate Carolyn Bertozzi, PhD, opened a new chapter ...







