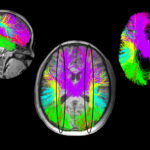
Sharing our journey with cavernous malformations
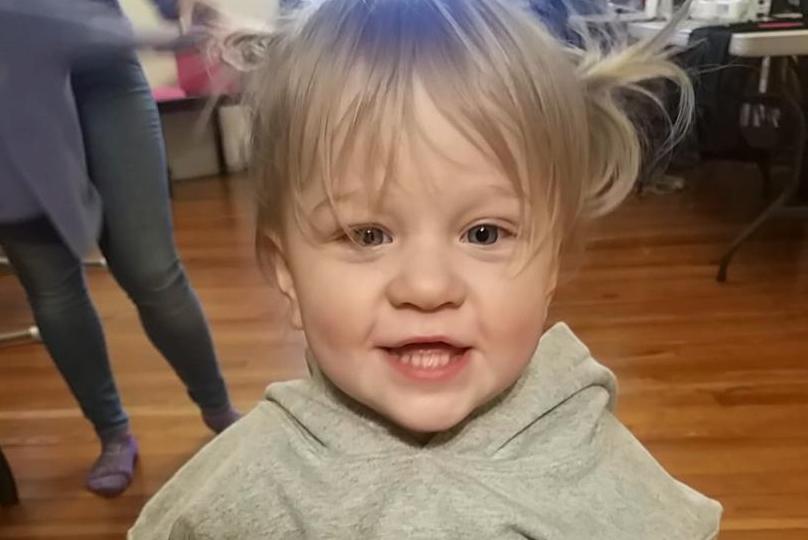
Finley and her twin sister, Rowan, were born seven weeks premature on November 7, 2017 in Scranton, Pennsylvania. In July 2019, Finley was diagnosed with a cavernous malformation, an abnormal mass of thin-walled blood vessels, in a part of her brain called the cerebellum. My wife, Jolene, and I were shocked. Although I was diagnosed with a cerebral cavernous malformation at age 27, I had been told that the condition happens later in life, and never considered our 20-month-old daughter could have it.
I hope sharing the steps of our treatment journey with other families helps to alleviate some of the anxiety and confusion that’s inevitable when your child is diagnosed with a serious illness.
Finley takes a fall
Early in July 2019, Finley lost her balance, fell down three steps, and hit her head. We took her to our local hospital and they decided she didn’t need a CT scan since she had never lost consciousness, did not vomit, and was running around the room.
Diagnosis: Brain bleed
A few weeks later, we noticed Finley seemed clumsier than usual and was drifting to the left when she walked. We took her to the pediatrician and soon she started vomiting and her balance seemed worse. The doctor said it was probably a virus. Not long after that, she could not stand and she vomited every time she moved. We rushed her to the hospital, where they performed more tests.
At the hospital, we got the worst news we could hear — Finley had a bleed in her brain. The doctors thought the bleed had created instability in Finley’s gait, contributing to her fall earlier in the month.
The emergency room doctor told us there was a mass in Finley’s brain near the bleed and speculated it was a tumor. It was soon after that the doctors diagnosed Finley with a cerebral cavernous malformation in her cerebellum.

Searching for, and finding, care
After extensive research, I learned that the expert for treating cerebral cavernous malformations in children is Dr. Edward Smith of Boston Children’s Hospital. I contacted him to get a second opinion and he responded immediately. He confirmed Finley’s diagnosis and said that while he was not one to rush to surgery, because of the size and location of the malformation, as well as Finley’s age, it needed to be removed soon. He suggested waiting four to six weeks to give Finley’s brain time to heal from the bleed.
Preparing for brain surgery
During the month leading up to Finley’s surgery we kept an open line of communication with Dr. Smith and his team. We worked with the team on insurance coverage and the schedule for Finley’s surgery.
When we walked through the doors at Boston Children’s for Finley’s pre-op MRI in late August 2019, we marveled at how focused everyone was on Finley. They made her comfort their number one priority. Every staff member put Finley at ease. Our previous hospital stays were traumatic and put us on high alert, but at Boston’s Children’s we could relax and focus on caring for Finley.
On the day before surgery, we met with Dr. Smith and his team to discuss Finley’s surgical plan. They answered every question in detail.
The day of surgery
On August 28, 2019, we arrived at Boston Children’s at 7 a.m., checked in, and were directed to the pre-op area. In pre-op, staff members came by to go over their part of the surgery, answer questions, and make sure Finley was calm, happy, and occupied. A nurse let Finely watch her favorite video — Queen’s 1985 Live Aid performance — on her cell phone. We were directed to a comfortable waiting room, and in no time we were getting updates on Finley. Before we knew it, we were on our way to see her.

Post-op and going home
Finley stayed in the Medical-Surgical Intensive Care Unit (MSICU) for one night, and was moved to the neurosurgery inpatient floor the next day. The nurses and staff were all wonderful, following Finley’s cues and including her in their assessments. Finley had a follow-up scan to check the area of surgery, and it looked great. When we left the hospital, Finley was smiling and we were feeling completely relieved.
Looking toward the future
Finley will need some physical therapy to help with weakness in her left leg from her first brain bleed, but thanks to Dr. Smith and his team, she will have zero permanent deficits. We will need to monitor Finley’s condition for the rest of her life, and it’s possible the same condition may affect our other children. But we have Dr. Smith and team to help every step of the way. Boston Children’s will always be the trusted place for our children’s care.
Learn more about the Cerebrovascular Surgery and Interventions Center.
Related Posts :
-

Small gains with big meaning: Loic’s story of deep brain stimulation for PKAN care
Loic, 5, lives in Montana with his parents, Sherine and Mark, and his sister, Selah. He loves Spider-Man, sushi, and the ...
-

Mapping ‘neighborhoods’ in aggressive childhood brain tumors
The third-most common kind of childhood brain tumor, supratentorial ependymoma, is an aggressive cancer that often returns after surgery and ...
-

Promising advances in fetal therapy for vein of Galen malformation
In 2024, Megan Ingram* of California and her husband were preparing for the birth of their third child when a 34-week ...
-

Unveiling the hidden impact of moyamoya disease: Brain injury without symptoms
Moyamoya disease — a rare, progressive condition that narrows the brain’s blood vessels — leads to an increased risk of stroke ...