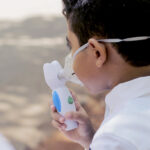
Asthma and COVID: Four things families need to know now

It’s an ongoing message from the media: People with underlying health conditions appear to be at higher risk for developing complications of COVID-19. So it’s no wonder that kids with asthma and their parents are worried. “Almost every family I speak with has questions about COVID-19,” says Elizabeth Klements, a pediatric nurse practitioner at Bridgewater Pediatrics, part of the Boston Children’s Primary Care Alliance, who specializes in treating asthma.
For expert guidance on this topic, we sought answers from Klements and her Boston Children’s colleague, pediatric nurse practitioner Kendall McCarty. Here’s what families of kids with asthma should know.
1. The risk of complications from COVID-19 may be greater.
There’s still much we don’t know about the new coronavirus and its effects on health — especially in kids. That said, chronic lung disease, including asthma, was the most common underlying condition among 345 children with COVID-19 for whom information on underlying conditions was available, according to the latest report on children and COVID-19 by the Centers for Disease Control and Prevention (CDC). That may be because, like asthma, COVID-19 can affect the respiratory tract, making it difficult to breathe.
The takeaway? “Like any other virus or respiratory illness, COVID-19 can trigger asthma,” says McCarty. “That means it’s even more important to take precautions.”
2. Prevention is key.
Both children and adults with asthma should follow the same preventive measures to help protect against COVID-19. That means washing your hands with soap and water thoroughly and often, refraining from touching your face, disinfecting surfaces, staying home as much as possible, and practicing physical distancing of at least six feet in public. “These are the best ways we know to help stop the spread of COVID-19,” says Klements.
3. Follow your asthma plan.
An asthma action plan is a personalized approach to helping manage asthma based on levels of symptom severity. “Every Boston Children’s asthma patient has an individual action plan to help prevent and control attacks and should continue to follow it now,” says Klements. If you don’t have an asthma action plan, call the office of your primary care provider, and they can email or mail you a copy.
4. Stay the course with asthma meds.
Clinicians typically recommend managing asthma with two types of inhalers. Quick-relief inhalers, known as bronchodilators, open airways on an as-needed basis, while inhaled corticosteroids are used to manage inflammation in the long term. “We already advise patients to use their inhalers at the first sign of a cough or wheeze,” Klements explains. “That recommendation still holds true now.” Follow the instructions on your asthma action plan.
For all patients with asthma, McCarty reports that clinicians are opting to use inhalers with spacers rather than nebulizers to deliver asthma meds. You can use a nebulizer at home, if this is your child’s preferred method to take their asthma medicine. The hospital, as well as clinics, is now avoiding the use of nebulizers, so that the mist from them will not carry germs into the air. “We’re hopeful that this approach will help decrease the chances of spreading COVID-19,” she says.
While this can be a scary time for kids with asthma and their families, prevention still remains the best medicine. “There isn’t any secret formula,” she says. “The most effective things families can do right now are to protect against COVID-19 and keep asthma under control.”
Get more answers about Boston Children’s response to COVID-19.
Related Posts :
-

Model enables study of age-specific responses to COVID mRNA vaccines in a dish
mRNA vaccines clearly saved lives during the COVID-19 pandemic, but several studies suggest that older people had a somewhat reduced ...
-

Will early intervention prevent asthma in school-age children?
Asthma affects about 1 in 10 children, often sending them to the emergency room or causing them to miss school. Allergic conditions ...
-

New insight into the effects of PPIs in children
Proton-pump inhibitors (PPIs) are frequently prescribed to suppress stomach acid in patients with gastroesophageal reflux disease (GERD). Prescribing rates of ...
-

Creating the next generation of mRNA vaccines
During the COVID-19 pandemic, mRNA vaccines came to the rescue, developed in record time and saving lives worldwide. Researchers in ...