Modeling urinary tract disorders on a chip: Zohreh Izadifar

When a new tissue sample arrives from the Department of Urology, the Boston Children’s Hospital lab of Zohreh Izadifar, PhD springs into action. The tissue, from a child with urinary tract pathology, is whisked into the tissue culture room. Under a hood, lab members Dasvit Shetty, PhD, and Gretchen Carpenter, MSc, carefully isolate the cells that form the inner wall of the urinary tract.
They then seed the cells into an organ-on-a-chip device — a small piece of flexible and breathable plastic that will house the cells for the next two weeks. Fluid or air flowed through channels inside the organ chip will help the cells feel more like they do inside the body.
Izadifar snaps the chip into a holder and slides it into an incubator. Over time, the cells will grow and arrange themselves as mechanical and chemical cues are applied, mimicking cells in the body. The final product will allow her to study the biology of conditions such as urinary tract infection and test new treatments.

Like most engineers, Izadifar is a problem solver. She initially trained as a civil and geological engineer at the University of Saskatchewan, but midway through she switched to biomedical engineering. “I liked its sophistication and the multidisciplinary approach to complex natural phenomena,” she says. “I also liked that engineers can learn from the intelligence in biological systems and leverage that to solve medical problems.”
Building a bioengineering toolbox
Izadifar’s PhD project was in tissue engineering, growing cartilage tissue from cells in the laboratory. “Cartilage looks simple, but it’s not so simple to engineer,” she says. “It’s a soft tissue, but it tolerates massive amounts of mechanical forces, for example, up to 10 times our body weight in the knees.”
Using biofabrication techniques, Izadifar created microenvironments where cartilage cells could grow and form a mechanically robust tissue. She developed a 3D bioprinting method that creates cartilage and bone tissue constructs with living cells, as well as a new X-ray imaging technique to observe how these engineered tissues grow in the body.
“My passion is using advanced technologies and different engineering and biological approaches to solve complex medical problems,” she says.
As a postdoctoral fellow at the University of Toronto, Izadifar grew her toolbox of technologies by learning stem cell and regenerative medicine techniques. Moving on to her position at the Wyss Institute, she expanded into organs-on-a-chip, leading the development of a human cervix-on-a-chip.
Modeling the cervix
To create the Cervix Chip, Izadifar and her colleagues layered epithelial cells, which line the inner surface of the cervix, and fibroblasts, which make structural and connective proteins like collagen, inside the chip. They successfully engineered the upper and lower tissues of the cervical canal and even reproduced mucus production, closely mimicking mucus secretion by the human cervix.
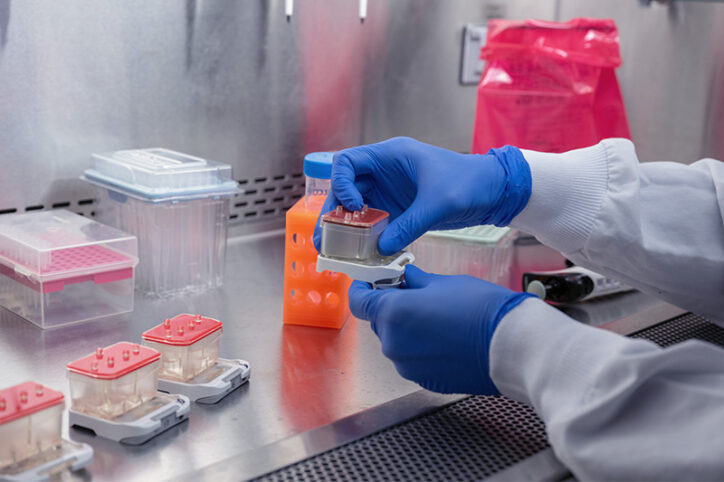
As described last year in Nature Communications, the team observed how the Cervix Chip model responded to sex hormones, acidity levels, and bacterial infection just as the cervix does in the body. The chip also replicated the influence of cervicovaginal microbiome: Healthy “good” bacteria thickened and enhanced the mucus layer, while “bad” infectious bacteria compromised the epithelial layer’s barrier function and spurred production of inflammatory proteins.
Now at Boston Children’s, Izadifar is using the Cervix Chip to study bacterial vaginosis, a hard-to-treat condition that can increase susceptibility to sexually transmitted diseases and preterm deliveries. Through collaborations, she is building chip models using cells from a wide range of patients to better understand why some women are more susceptible to bacterial vaginosis.
Modeling UTI, neurogenic bladder, urinary incontinence, and interstitial cystitis
Izadifar’s new human lower urinary tract organ chips will enable her to better understand the physiology and pathophysiology of the urinary tract’s mucosal lining and the role of factors like the microbiome in making people more or less susceptible to UTI.
“Some people think it’s the urogenital anatomy that makes, for example, females prone to UTIs,” she says. “But I believe there is much more yet to be discovered.”

Eventually, Izadifar hopes to use these human organ-chip models to develop and test new treatments for UTIs that have become resistant to antibiotics. She also plans to create models of neurogenic bladder, urinary incontinence, and interstitial cystitis, also known as painful bladder syndrome, and investigate factors that contribute to these conditions. Aiding this effort is a collaboration with Richard S. Lee, MD, in the Department of Urology to obtain tissues from his comprehensive repository of patient samples.
“Urology has a lot of research and translational gaps,” Izadifar says. “We still don’t know the cause of many chronic conditions or why current treatment options don’t always work. We hope these studies will give us more options for patients suffering from these conditions.”
Learn more about research in the Department of Urology and read more profiles of our researchers.
Related Posts :
-

Two rising stars in kidney genetics: Nina Mann and Amar Majmundar
A healthy, functional kidney must maintain a delicate balance of water, nutrients, and electrolytes so it can properly filter the ...
-

Making a change: After a second opinion for spina bifida care, Sydney is thriving
At almost 10 years old, Sydney MacKay is sassy, spunky, and wants to be as independent as possible. Because she was ...
-

Helping manage ‘sensitive issues’: How our psychosocial team helps kids with urologic concerns
In Boston Children’s Department of Urology, urologists, pediatricians, and nurses aren’t the only ones who care for kids ...
-

Skin organoid could guide new treatments for skin conditions, hair loss
What does it take to build healthy skin? Two research groups converged on this question from different angles. They've now ...